Alzheimer's Disease: Past, Present, and Future
- PMID: 29198280
- PMCID: PMC5830188
- DOI: 10.1017/S135561771700100X
Alzheimer's Disease: Past, Present, and Future
Abstract
Although dementia has been described in ancient texts over many centuries (e.g., "Be kind to your father, even if his mind fail him." - Old Testament: Sirach 3:12), our knowledge of its underlying causes is little more than a century old. Alzheimer published his now famous case study only 110 years ago, and our modern understanding of the disease that bears his name, and its neuropsychological consequences, really only began to accelerate in the 1980s. Since then we have witnessed an explosion of basic and translational research into the causes, characterizations, and possible treatments for Alzheimer's disease (AD) and other dementias. We review this lineage of work beginning with Alzheimer's own writings and drawings, then jump to the modern era beginning in the 1970s and early 1980s and provide a sampling of neuropsychological and other contextual work from each ensuing decade. During the 1980s our field began its foundational studies of profiling the neuropsychological deficits associated with AD and its differentiation from other dementias (e.g., cortical vs. subcortical dementias). The 1990s continued these efforts and began to identify the specific cognitive mechanisms affected by various neuropathologic substrates. The 2000s ushered in a focus on the study of prodromal stages of neurodegenerative disease before the full-blown dementia syndrome (i.e., mild cognitive impairment). The current decade has seen the rise of imaging and other biomarkers to characterize preclinical disease before the development of significant cognitive decline. Finally, we suggest future directions and predictions for dementia-related research and potential therapeutic interventions. (JINS, 2017, 23, 818-831).
Keywords: Alzheimer’s disease; Biomarkers; Clinical trials; Cognition; Mild cognitive impairment; Neuroimaging; Neuropsychology; Neuroscience.
Figures



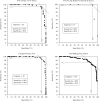

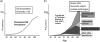
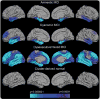
References
-
- Albert MS, DeKosky ST, Dickson D, Dubois B, Feldman HH, Fox NC, Phelps CH. The diagnosis of mild cognitive impairment due to Alzheimer’s disease: Recommendations from the National Institute on Aging-Alzheimer’s Association workgroups on diagnostic guidelines for Alzheimer’s disease. Alzheimer’s & Dementia. 2011;7:270–279. - PMC - PubMed
-
- Alzheimer A. über eine eigenartige Erkankung der Hirnrinde. Allgemeine Zeitschrift fur Psychiatrie under Psychisch-Gerichtliche Medizin. 1907;64:146–148.
-
- Alzheimer A. Über eigenartige Krankheitsfälle des späteren Alters. Zeitschrift für die Gesamte Neurologie und Psychiatrie. 1911;4:356–385.
-
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. 2. Washington, DC: American Psychiatric Association; 1968.
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

