Pulmonary Complications after Surgery for Rectal Cancer in Elderly Patients: Evaluation of Laparoscopic versus Open Approach from a Multicenter Study on 477 Consecutive Cases
- PMID: 29201047
- PMCID: PMC5671719
- DOI: 10.1155/2017/5893890
Pulmonary Complications after Surgery for Rectal Cancer in Elderly Patients: Evaluation of Laparoscopic versus Open Approach from a Multicenter Study on 477 Consecutive Cases
Abstract
Aim: To evaluate the impact of open or laparoscopic rectal surgery on pulmonary complications in elderly (>75 years old) patients.
Methods: Data from consecutive patients who underwent elective laparoscopic or open rectal surgery for cancer were collected prospectively from 3 institutions. Pulmonary complications were defined according to the ACS/NSQUIP definition.
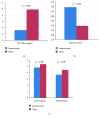
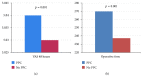
Results: A total of 477 patients (laparoscopic group: 242, open group: 235) were included in the analysis. Postoperative pulmonary complications were significantly more common after open surgery (8 out of 242 patients (3.3%) versus 23 out of 235 patients (9.8%); p = 0.005). In addition, PPC occurrence was associated with the increasing of postoperative pain (5.04 ± 1.62 versus 5.03 ± 1.58; p = 0.001) and the increasing of operative time (270.06 ± 51.49 versus 237.37 ± 65.97; p = 0.001).
Conclusion: Our results are encouraging to consider laparoscopic surgery a safety and effective way to treat rectal cancer in elderly patients, highlighting that laparoscopic surgery reduces the occurrence of postoperative pulmonary complications.
Figures
References
-
- Schiphorst A. H., Verweij N. M., Pronk A., Borel Rinkes I. H., Hamaker M. E. Non-surgical complications after laparoscopic and open surgery for colorectal cancer—a systematic review of randomised controlled trials. European Journal of Surgical Oncology. 2015;41(9):1118–1127. doi: 10.1016/j.ejso.2015.04.007. - DOI - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources

