Prevalence, treatment patterns and control rates of metabolic syndrome in a Chinese diabetic population: China Cardiometabolic Registries 3B study
- PMID: 29205907
- PMCID: PMC6031517
- DOI: 10.1111/jdi.12785
Prevalence, treatment patterns and control rates of metabolic syndrome in a Chinese diabetic population: China Cardiometabolic Registries 3B study
Abstract
Aims/introduction: To investigate the prevalence and risk factors of metabolic syndrome (MetS) in Chinese type 2 diabetes mellitus patients, and assess the effect of MetS on the treatment patterns and blood glucose, blood pressure and blood lipids goal achievements.
Materials and methods: Data from 25,454 type 2 diabetes mellitus patients including demographic data, anthropometric measurements, treatment patterns, and blood glucose and lipid profiles were retrospectively analyzed.
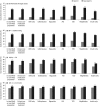
Results: Using modified Adult Treatment Panel III MetS criteria, the prevalence of MetS was 57.4% in type 2 diabetes mellitus patients. Multivariable logistic regression analysis showed that type 2 diabetes mellitus patients, who also fulfilled the criteria for MetS, tended to be women, living in the northeast, with a diabetes duration ≥5 years and leading a sedentary lifestyle. Most MetS (53.4%) and non-MetS (57%) diabetes patients received oral hypoglycemic drugs. Insulin or insulin combination therapies were more applied in MetS (37.5%) than in non-MetS (33.1%) diabetes patients, and the percentages of MetS diabetes patients receiving antihypertensive and lipid-modulating drugs were 52.9% and 28.2% vs 38.3% and 19.3% of the non-MetS diabetes patients. Just 37.5%, 15.6% and 32.9% of the MetS diabetes patients vs 54.6%, 45.6% and 40.4% of the non-MetS diabetes patients achieved the individual target goals for control of blood glucose (glycosylated hemoglobin <7%), blood pressure (systolic blood pressure <130 mmHg, diastolic blood pressure <80 mmHg) and blood lipids (total cholesterol <4.5 mmol/L), whereas just 2.1% achieved all three target goals.
Conclusions: MetS with a high prevalence in Chinese type 2 diabetes mellitus patients is associated with poor blood glucose, blood pressure and blood lipids control rate.
Keywords: Blood lipids; Diabetes mellitus; Metabolic syndrome.
© 2017 Merck Sharp & Dohme Corp. Journal of Diabetes Investigation published by Asian Association for the Study of Diabetes (AASD) and John Wiley & Sons Australia, Ltd.
Figures
Similar articles
-
Prevalence of Obesity and Its Influence on Achievement of Cardiometabolic Therapeutic Goals in Chinese Type 2 Diabetes Patients: An Analysis of the Nationwide, Cross-Sectional 3B Study.PLoS One. 2016 Jan 4;11(1):e0144179. doi: 10.1371/journal.pone.0144179. eCollection 2016. PLoS One. 2016. PMID: 26726883 Free PMC article.
-
[The relationship between non-alcoholic fatty liver disease and metabolic syndrome in patients with latent autoimmune diabetes in adults].Zhonghua Yi Xue Za Zhi. 2018 Aug 14;98(30):2398-2402. doi: 10.3760/cma.j.issn.0376-2491.2018.30.006. Zhonghua Yi Xue Za Zhi. 2018. PMID: 30138983 Chinese.
-
Metabolic syndrome and risk of major coronary events among the urban diabetic patients: North Indian Diabetes and Cardiovascular Disease Study-NIDCVD-2.J Diabetes Complications. 2016 Jan-Feb;30(1):72-8. doi: 10.1016/j.jdiacomp.2015.07.008. Epub 2015 Jul 20. J Diabetes Complications. 2016. PMID: 26271411
-
Prevalence and clustering of metabolic risk factors for type 2 diabetes among Chinese adults in Shanghai, China.BMC Public Health. 2010 Nov 9;10:683. doi: 10.1186/1471-2458-10-683. BMC Public Health. 2010. PMID: 21062480 Free PMC article.
-
Anthocyanins in the Management of Metabolic Syndrome: A Pharmacological and Biopharmaceutical Review.Front Pharmacol. 2018 Dec 4;9:1310. doi: 10.3389/fphar.2018.01310. eCollection 2018. Front Pharmacol. 2018. PMID: 30564116 Free PMC article. Review.
Cited by
-
Prevalence and co-prevalence of comorbidities among Chinese adult patients with type 2 diabetes mellitus: a cross-sectional, multicenter, retrospective, observational study based on 3B study database.Front Endocrinol (Lausanne). 2024 Jun 11;15:1362433. doi: 10.3389/fendo.2024.1362433. eCollection 2024. Front Endocrinol (Lausanne). 2024. PMID: 38919489 Free PMC article.
-
Association of Insulin Glargine Treatment with Bone Mineral Density in Patients with Type 2 Diabetes Mellitus.Diabetes Metab Syndr Obes. 2021 Apr 29;14:1909-1917. doi: 10.2147/DMSO.S302627. eCollection 2021. Diabetes Metab Syndr Obes. 2021. PMID: 33953588 Free PMC article.
-
Association of Health Information Literacy and Health Outcomes Among Individuals with Type 2 Diabetes and Metabolic Syndrome.Nurs Rep. 2025 Mar 5;15(3):90. doi: 10.3390/nursrep15030090. Nurs Rep. 2025. PMID: 40137663 Free PMC article.
-
Metabolic Syndrome in Patients With Diabetes Mellitus.Cureus. 2022 Apr 25;14(4):e24469. doi: 10.7759/cureus.24469. eCollection 2022 Apr. Cureus. 2022. PMID: 35637809 Free PMC article.
-
Gamma-glutamyl transferase to high-density lipoprotein cholesterol ratio is a more powerful marker than TyG index for predicting metabolic syndrome in patients with type 2 diabetes mellitus.Front Endocrinol (Lausanne). 2023 Oct 3;14:1248614. doi: 10.3389/fendo.2023.1248614. eCollection 2023. Front Endocrinol (Lausanne). 2023. PMID: 37854188 Free PMC article.
References
-
- Reaven GM. Banting lecture 1988. Role of insulin resistance in human disease. Diabetes 1988; 37: 1595–1607. - PubMed
-
- Grundy SM, Cleeman JI, Daniels SR, et al Diagnosis and management of the metabolic syndrome: an American Heart Association/National Heart, Lung, and Blood Institute Scientific Statement. Circulation 2005; 112: 2735–2752. - PubMed
-
- Luk AO, Ma RC, So WY, et al The NCEP‐ATPIII but not the IDF criteria for the metabolic syndrome identify Type 2 diabetic patients at increased risk of chronic kidney disease. Diabet Med 2008; 25: 1419–1425. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

