Decreased Lymphocyte-to-Monocyte Ratio Predicts Poor Prognosis of Acute Ischemic Stroke Treated with Thrombolysis
- PMID: 29220346
- PMCID: PMC5731214
- DOI: 10.12659/msm.907919
Decreased Lymphocyte-to-Monocyte Ratio Predicts Poor Prognosis of Acute Ischemic Stroke Treated with Thrombolysis
Abstract
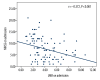
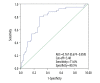
BACKGROUND Our previous study found that lower lymphocyte-to-monocyte ratio (LMR) is an independent risk factor of clinical outcome of acute ischemic stroke (AIS). However, whether lower LMR is independently associated with adverse prognosis of AIS treated with thrombolysis has not been determined. In this study, we explored the relationship between LMR and prognosis of AIS treated with thrombolysis. MATERIAL AND METHODS We retrospectively enrolled 108 patients treated with thrombolysis. LMR was calculated according to lymphocyte count and monocyte count on admission. Patients were classified into 3 groups according to LMR values on admission (group 1 LMR >4.34, group 2 LMR 2.79 to 4.34, group 3 LMR <2.79). Neurologic impairment was estimated by use of the National Institute of Health Stroke Scale. Clinical prognosis at 3 months was assessed by modified Rankin Scale. The relationship between LMR and neurologic impairment was analyzed by Spearman rank correlation. Receiver operating characteristic curve (ROC) was used to evaluate the ability of LMR to predict outcome. RESULTS Patients in group 3 had lower lymphocyte counts and LMR values and higher monocyte counts (P<0.001). LMR value was negatively correlated with the degree of neurologic impairment (r=-0.372, P<0.001). The ROC suggested a moderate sensitivity (71.6%) and specificity (80.5%) of LMR for predicting prognosis with an optimal cut-off point at 3.48. Higher LMR value was an independent protective factor against adverse prognosis (odds ratio 0.683, 95% confidence interval 0.490-0.952, P=0.024). CONCLUSIONS A lower LMR value is an independent predictor of poor prognosis of AIS treated with thrombolytic therapy.
Conflict of interest statement
None.
Figures
Similar articles
-
Lymphocyte-to-Monocyte Ratio: A Novel Predictor of the Prognosis of Acute Ischemic Stroke.J Stroke Cerebrovasc Dis. 2017 Nov;26(11):2595-2602. doi: 10.1016/j.jstrokecerebrovasdis.2017.06.019. Epub 2017 Aug 26. J Stroke Cerebrovasc Dis. 2017. PMID: 28847530
-
The Prognosis of Neutrophil-to-Lymphocyte Ratio and Lymphocyte-to-Monocyte Ratio in Elderly with Acute Ischemic Stroke.Clin Interv Aging. 2024 Oct 19;19:1715-1720. doi: 10.2147/CIA.S491753. eCollection 2024. Clin Interv Aging. 2024. PMID: 39444392 Free PMC article.
-
High Neutrophil-Lymphocyte Ratio and Low Lymphocyte-Monocyte Ratio Combination after Thrombolysis Is a Potential Predictor of Poor Functional Outcome of Acute Ischemic Stroke.J Pers Med. 2022 Jul 27;12(8):1221. doi: 10.3390/jpm12081221. J Pers Med. 2022. PMID: 35893315 Free PMC article.
-
Prognostic value of lymphocyte-to-monocyte ratio in acute ischemic stroke: a systematic review and meta-analysis.Front Neurol. 2025 May 7;16:1567112. doi: 10.3389/fneur.2025.1567112. eCollection 2025. Front Neurol. 2025. PMID: 40401022 Free PMC article. Review.
-
The predictive value of lymphocyte-to-monocyte ratio in the prognosis of acute coronary syndrome patients: a systematic review and meta-analysis.BMC Cardiovasc Disord. 2020 Jul 15;20(1):338. doi: 10.1186/s12872-020-01614-x. BMC Cardiovasc Disord. 2020. PMID: 32669086 Free PMC article.
Cited by
-
SDL Index Predicts Stroke-Associated Pneumonia in Patients After Endovascular Therapy.Front Neurol. 2021 Feb 16;12:622272. doi: 10.3389/fneur.2021.622272. eCollection 2021. Front Neurol. 2021. PMID: 33664704 Free PMC article.
-
Immunoreactive Cells After Cerebral Ischemia.Front Immunol. 2019 Nov 26;10:2781. doi: 10.3389/fimmu.2019.02781. eCollection 2019. Front Immunol. 2019. PMID: 31849964 Free PMC article. Review.
-
Chocolate Consumers and Lymphocyte-to-Monocyte Ratio: A Working Hypothesis from a Preliminary Report of a Pilot Study in Celiac Subjects.Antioxidants (Basel). 2019 Oct 1;8(10):440. doi: 10.3390/antiox8100440. Antioxidants (Basel). 2019. PMID: 31581490 Free PMC article.
-
CD163 as a Potential Biomarker of Monocyte Activation in Ischemic Stroke Patients.Int J Mol Sci. 2021 Jun 23;22(13):6712. doi: 10.3390/ijms22136712. Int J Mol Sci. 2021. PMID: 34201498 Free PMC article.
-
Acute Inflammation in Cerebrovascular Disease: A Critical Reappraisal with Focus on Human Studies.Life (Basel). 2021 Oct 17;11(10):1103. doi: 10.3390/life11101103. Life (Basel). 2021. PMID: 34685473 Free PMC article. Review.
References
-
- Mozaffarian D, Benjamin EJ, Go AS, et al. Heart disease and stroke statistics – 2016 update: A report from the American Heart Association. Circulation. 2016;133:e38–360. - PubMed
-
- Powers WJ, Derdeyn CP, Biller J, et al. 2015 American Heart Association/American Stroke Association focused update of the 2013 guidelines for the early management of patients with acute ischemic stroke regarding endovascular treatment: A guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2015;46:3020–35. - PubMed
-
- Rodrigues SF, Granger DN. Leukocyte-mediated tissue injury in ischemic stroke. Curr Med Chem. 2014;21:2130–37. - PubMed
-
- Liberale L, Montecucco F, Bonaventura A, et al. Monocyte count at onset predicts post-stroke outcomes during a 90-day follow up. Eur J Clin Invest. 2017;47(10):702–10. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

