Tumor necrosis factor-α antagonist diminishes osteocytic RANKL and sclerostin expression in diabetes rats with periodontitis
- PMID: 29240821
- PMCID: PMC5730195
- DOI: 10.1371/journal.pone.0189702
Tumor necrosis factor-α antagonist diminishes osteocytic RANKL and sclerostin expression in diabetes rats with periodontitis
Abstract
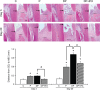
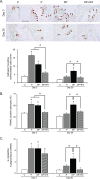
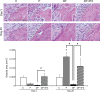
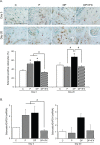
Type 1 diabetes with periodontitis shows elevated TNF-α expression. Tumor necrosis factor (TNF)-α stimulates the expression of receptor activator of nuclear factor-κB ligand (RANKL) and sclerostin. The objective of this study was to determine the effect of TNF-α expression of osteocytic RANKL and sclerostin in type 1 diabetes rats with periodontitis using infliximab (IFX), a TNF-α antagonist. Rats were divided into two timepoint groups: day 3 and day 20. Each timepoint group was then divided into four subgroups: 1) control (C, n = 6 for each time point); 2) periodontitis (P, n = 6 for each time point); 3) diabetes with periodontitis (DP, n = 8 for each time point); and 4) diabetes with periodontitis treated with IFX (DP+IFX, n = 8 for each time point). To induce type 1 diabetes, rats were injected with streptozotocin (50 mg/kg dissolved in 0.1 M citrate buffer). Periodontitis was then induced by ligature of the mandibular first molars at day 7 after STZ injection (day 0). IFX was administered once for the 3 day group (on day 0) and twice for the 20 day group (on days 7 and 14). The DP group showed greater alveolar bone loss than the P group on day 20 (P = 0.020). On day 3, higher osteoclast formation and RANKL-positive osteocytes in P group (P = 0.000 and P = 0.011, respectively) and DP group (P = 0.006 and P = 0.017, respectively) than those in C group were observed. However, there was no significant difference in osteoclast formation or RANKL-positive osteocytes between P and DP groups. The DP+IFX group exhibited lower alveolar bone loss (P = 0.041), osteoclast formation (P = 0.019), and RANKL-positive osteocytes (P = 0.009) than that of the DP group. On day 20, DP group showed a lower osteoid area (P = 0.001) and more sclerostin-positive osteocytes (P = 0.000) than P group. On days 3 and 20, the DP+IFX group showed more osteoid area (P = 0.048 and 0.040, respectively) but lower sclerostin-positive osteocytes (both P = 0.000) than DP group. Taken together, these results suggest that TNF-α antagonist can diminish osteocytic RANKL/sclerostin expression and osteoclast formation, eventually recovering osteoid formation. Therefore, TNF-α might mediate alveolar bone loss via inducing expression of osteocytic RANKL and sclerostin in type 1 diabetes rats with periodontitis.
Conflict of interest statement
Figures
References
-
- Zofkova I, Matucha P. New insights into the physiology of bone regulation: the role of neurohormones. Physiol Res. 2014;63(4):421–7. . - PubMed
-
- Almeida M, O'Brien CA. Basic biology of skeletal aging: role of stress response pathways. J Gerontol A Biol Sci Med Sci. 2013;68(10):1197–208. doi: 10.1093/gerona/glt079 ; PubMed Central PMCID: PMCPMC3779633. - DOI - PMC - PubMed
-
- Hofbauer LC, Heufelder AE. Role of receptor activator of nuclear factor-κB ligand and osteoprotegerin in bone cell biology. J Mol Med (Berl). 2001;79(5–6):243–53. . - PubMed
-
- Nakashima T, Hayashi M, Fukunaga T, Kurata K, Oh-Hora M, Feng JQ, et al. Evidence for osteocyte regulation of bone homeostasis through RANKL expression. Nat Med. 2011;17(10):1231–4. doi: 10.1038/nm.2452 . - DOI - PubMed
-
- Kim JH, Lee DE, Cha JH, Bak EJ, Yoo YJ. Receptor activator of nuclear factor-κB ligand and sclerostin expression in osteocytes of alveolar bone in rats with ligature-induced periodontitis. J Periodontol. 2014;85(11):e370–8. doi: 10.1902/jop.2014.140230 . - DOI - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Molecular Biology Databases

