An Observational Study of the Efficacy of Cisatracurium Compared with Vecuronium in Patients with or at Risk for Acute Respiratory Distress Syndrome
- PMID: 29241014
- PMCID: PMC6020402
- DOI: 10.1164/rccm.201706-1132OC
An Observational Study of the Efficacy of Cisatracurium Compared with Vecuronium in Patients with or at Risk for Acute Respiratory Distress Syndrome
Abstract
Rationale: The neuromuscular blocking agent cisatracurium may improve mortality for patients with moderate-to-severe acute respiratory distress syndrome (ARDS). Other neuromuscular blocking agents, such as vecuronium, are commonly used and have different mechanisms of action, side effects, cost, and availability in the setting of drug shortages.
Objectives: To determine whether cisatracurium is associated with improved outcomes when compared with vecuronium in patients at risk for and with ARDS.
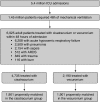
Methods: Using a nationally representative database, patients who were admitted to the ICU with a diagnosis of ARDS or an ARDS risk factor, received mechanical ventilation, and were treated with a continuous infusion of neuromuscular blocking agent for at least 2 days within 2 days of hospital admission were included. Patients were stratified into two groups: those who received cisatracurium or vecuronium. Propensity matching was used to balance both patient- and hospital-specific factors. Outcomes included hospital mortality, duration of mechanical ventilation, ICU and hospital duration, and discharge location.
Measurements and main results: Propensity matching successfully balanced all covariates for 3,802 patients (1,901 per group). There was no significant difference in mortality (odds ratio, 0.932; P = 0.40) or hospital days (-0.66 d; P = 0.411) between groups. However, patients treated with cisatracurium had fewer ventilator days (-1.01 d; P = 0.005) and ICU days (-0.98 d; P = 0.028) but were equally likely to be discharged home (odds ratio, 1.19; P = 0.056).
Conclusions: When compared with vecuronium, cisatracurium was not associated with a difference in mortality but was associated with improvements in other clinically important outcomes. These data suggest that cisatracurium may be the preferred neuromuscular blocking agent for patients at risk for and with ARDS.
Keywords: acute respiratory distress syndrome; mechanical ventilators; neuromuscular blockade; patient outcome assessment.
Figures
Comment in
-
Is Cisatracurium the Neuromuscular Blocking Agent of Choice in Acute Respiratory Distress Syndrome?Am J Respir Crit Care Med. 2018 Apr 1;197(7):849-850. doi: 10.1164/rccm.201712-2610ED. Am J Respir Crit Care Med. 2018. PMID: 29324189 No abstract available.
Similar articles
-
Comparison of Cisatracurium Versus Atracurium in Early ARDS.Respir Care. 2017 Jul;62(7):947-952. doi: 10.4187/respcare.05102. Epub 2017 Mar 28. Respir Care. 2017. PMID: 28351905
-
Efficacy and Safety of Cisatracurium Compared to Vecuronium for Neuromuscular Blockade in Acute Respiratory Distress Syndrome.J Intensive Care Med. 2023 Feb;38(2):188-195. doi: 10.1177/08850666221113504. Epub 2022 Jul 12. J Intensive Care Med. 2023. PMID: 35821572
-
Neuromuscular blockers in early acute respiratory distress syndrome.N Engl J Med. 2010 Sep 16;363(12):1107-16. doi: 10.1056/NEJMoa1005372. N Engl J Med. 2010. PMID: 20843245 Clinical Trial.
-
Newer neuromuscular blocking agents: how do they compare with established agents?Drugs. 2001;61(7):919-42. doi: 10.2165/00003495-200161070-00003. Drugs. 2001. PMID: 11434449 Review.
-
To Block or Not: Updates in Neuromuscular Blockade in Acute Respiratory Distress Syndrome.Ann Pharmacother. 2020 Sep;54(9):899-906. doi: 10.1177/1060028020910132. Epub 2020 Feb 28. Ann Pharmacother. 2020. PMID: 32111121 Review.
Cited by
-
Myorelaxants in ARDS patients.Intensive Care Med. 2020 Dec;46(12):2357-2372. doi: 10.1007/s00134-020-06297-8. Epub 2020 Nov 7. Intensive Care Med. 2020. PMID: 33159530 Free PMC article. Review.
-
Noninvasive Ventilation Use in Critically Ill Patients with Acute Asthma Exacerbations.Am J Respir Crit Care Med. 2020 Dec 1;202(11):1520-1530. doi: 10.1164/rccm.201910-2021OC. Am J Respir Crit Care Med. 2020. PMID: 32663410 Free PMC article.
-
Ventilator dyssynchrony - Detection, pathophysiology, and clinical relevance: A Narrative review.Ann Thorac Med. 2020 Oct-Dec;15(4):190-198. doi: 10.4103/atm.ATM_63_20. Epub 2020 Oct 10. Ann Thorac Med. 2020. PMID: 33381233 Free PMC article. Review.
-
Reducing the dose of neuromuscular blocking agents with adjuncts: a systematic review and meta-analysis.Br J Anaesth. 2021 Mar;126(3):608-621. doi: 10.1016/j.bja.2020.09.048. Epub 2020 Nov 17. Br J Anaesth. 2021. PMID: 33218672 Free PMC article.
-
Neuromuscular Blockade in the Pre- and COVID-19 ARDS Patients.J Pers Med. 2022 Sep 19;12(9):1538. doi: 10.3390/jpm12091538. J Pers Med. 2022. PMID: 36143323 Free PMC article. Review.
References
-
- Ashbaugh DG, Bigelow DB, Petty TL, Levine BE, Ashbaugh DG, Bigelow DB, Petty TL, Levine BE. Acute respiratory distress in adults. The Lancet, Saturday 12 August 1967 [review of the classics] Crit Care Resusc. 2005;7:60–61. - PubMed
-
- Webb HH, Tierney DF. Experimental pulmonary edema due to intermittent positive pressure ventilation with high inflation pressures: protection by positive end-expiratory pressure. Am Rev Respir Dis. 1974;110:556–565. - PubMed
-
- Brower RG, Matthay MA, Morris A, Schoenfeld D, Thompson BT, Wheeler A Acute Respiratory Distress Syndrome Network. Ventilation with lower tidal volumes as compared with traditional tidal volumes for acute lung injury and the acute respiratory distress syndrome. N Engl J Med. 2000;342:1301–1308. - PubMed
-
- Futier E, Constantin J-M, Paugam-Burtz C, Pascal J, Eurin M, Neuschwander A, et al. IMPROVE Study Group. A trial of intraoperative low-tidal-volume ventilation in abdominal surgery. N Engl J Med. 2013;369:428–437. - PubMed
-
- Serpa Neto A, Cardoso SO, Manetta JA, Pereira VGM, Espósito DC, Pasqualucci MDOP, et al. Association between use of lung-protective ventilation with lower tidal volumes and clinical outcomes among patients without acute respiratory distress syndrome: a meta-analysis. JAMA. 2012;308:1651–1659. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources