Molecular imaging of prostate cancer
- PMID: 29243485
- PMCID: PMC5966010
- DOI: 10.1259/bjr.20170736
Molecular imaging of prostate cancer
Abstract
Prostate cancer is a common malignancy with various treatments from surveillance, surgery, radiation and chemotherapy. The institution of appropriate, effective treatment relies in part on accurate imaging. Molecular imaging techniques offer an opportunity for increased timely detection of prostate cancer, its recurrence, as well as metastatic disease. Advancements within the field of molecular imaging have been complex with some agents targeting receptors and others acting as metabolic intermediaries. In this article, we provide an overview of the most clinically relevant radiotracers to date based on a combination of the five states model and the National Comprehensive Cancer Network Guidelines.
Figures
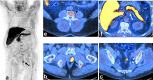
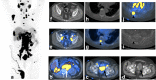
References
-
- National Comprehensive Cancer Network. Prostate cancer guidelines; 2017. Available from: www.nccn.org/professionals/physician_gls/pdf/prostate.pdf.
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

