The efficiency and safety of local liposomal bupivacaine infiltration for pain control in total hip arthroplasty: A systematic review and meta-analysis
- PMID: 29245214
- PMCID: PMC5728829
- DOI: 10.1097/MD.0000000000008433
The efficiency and safety of local liposomal bupivacaine infiltration for pain control in total hip arthroplasty: A systematic review and meta-analysis
Abstract
Objective: This meta-analysis aimed to compare the efficiency and safety of local liposomal bupivacaine infiltration and traditional cocktail analgesia for pain management in total hip arthroplasty (THA).
Methods: PubMed, Embase, Web of science, Medline, and Cochrane library databases were systematically searched.
Inclusion criteria: Participants: patients planned for a THA with a diagnosis of hip osteoarthritis.
Interventions: liposomal bupivacaine was administrated in the experimental groups for pain control. Comparisons: the control groups received local infiltration of traditional analgesics.
Outcomes: pain scores, opioids consumption, and postoperative complications among the patients.
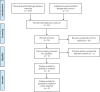
Study design: randomized control trials (RCTs) and non-RCTs. Methodological Index for Non-Randomized Studies scale was used to assess the methodological quality of the included studies. Meta-analysis was conducted by Stata 11.0 software. Systematic review registration number is CRD42017120981.
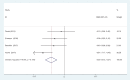
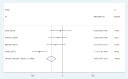
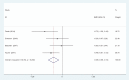
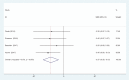
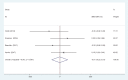
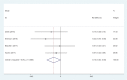
Results: Four articles involving 308 participants were included. Current meta-analysis revealed that there were significant differences regarding postoperative pain score at 12 hours (standard mean difference [SMD] = -0.496, 95% CI: -0.717 to -0.275, P = .000), 24 hours (SMD = -0.537, 95% CI: -0.760 to -0.313, P = .000), and 48 hours (SMD = -0.802, 95% CI: -1.029 to -0.576, P = .000). Liposomal bupivacaine intervention was found to significantly decrease opioid consumption at 12 hours (SMD = -0.544, 95% CI: -0.766 to -0.323, P = .000), 24 hours (SMD = -0.357, 95% CI: -0.577 to -0.138, P = .001), and 48 hours (SMD = -0.370, 95% CI: -0.589 to -0.151, P = .001).
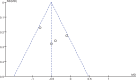
Conclusion: Local liposomal bupivacaine infiltration could significantly reduce visual analogue scale (VAS) scores and opioid consumption within the first 48 hours following THA surgery. In addition, there was a decreased risk of nausea and vomiting in liposomal bupivacaine groups. The overall evidence level was low, which means that further research is likely to significantly alter confidence levels in the effect, as well as potentially changing the estimates. In any subsequent research, further studies should focus on the optimal dose of local anesthetics and the potential adverse side effects. In addition, surgeries that can improve pain relief and enable faster rehabilitation and earlier discharges should also be explored. Several potential limitations of this study should be noted. Four articles are included and the sample size in each trial is small. Some important outcome parameters such as range of motion were not fully described and could not be included in the meta-analysis. All included studies were retrospectives which may decrease evidence levels for the meta-analysis. The evidence quality for each outcome was low which may influence the results of the meta-analysis. Short-term follow-ups may lead to the underestimation of complications, such as neurotoxicity and cardiotoxicity. Publication bias is an inherent weakness that exists in all meta-analyses.
Conflict of interest statement
The authors have no conflicts of interest to disclose.
Figures




References
-
- Amstutz HC, Thomas BJ, Jinnah R, et al. Treatment of primary osteoarthritis of the hip. A comparison of total joint and surface replacement arthroplasty. J Bone Joint Surg Am 1984;66:228–41. - PubMed
-
- Kurtz S, Ong K, Lau E, et al. Projections of primary and revision hip and knee arthroplasty in the United States from 2005 to 2030. J Bone Joint Surg Am 2007;89:780–5. - PubMed
-
- Kuchalik J, Granath B, Ljunggren A, et al. Postoperative pain relief after total hip arthroplasty: a randomized, double-blind comparison between intrathecal morphine and local infiltration analgesia. Br J Anaesth 2013;111:793–9. - PubMed
-
- Singelyn FJ, Ferrant T, Malisse MF, et al. Effects of intravenous patient-controlled analgesia with morphine, continuous epidural analgesia, and continuous femoral nerve sheath block on rehabilitation after unilateral total-hip arthroplasty. Reg Anesth Pain Med 2005;30:452–7. - PubMed
-
- Stevens M, Harrison G, McGrail M. A modified fascia iliaca compartment block has significant morphine-sparing effect after total hip arthroplasty. Anaesth Intensive Care 2007;35:949–52. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

