Biological and Clinical Implications of Comorbidities in Parkinson's Disease
- PMID: 29255414
- PMCID: PMC5722846
- DOI: 10.3389/fnagi.2017.00394
Biological and Clinical Implications of Comorbidities in Parkinson's Disease
Abstract
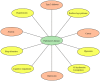
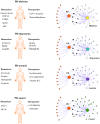
A wide spectrum of comorbidities has been associated with Parkinson's disease (PD), a progressive neurodegenerative disease that affects more than seven million people worldwide. Emerging evidence indicates that chronic diseases including diabetes, depression, anemia and cancer may be implicated in the pathogenesis and progression of PD. Recent epidemiological studies suggest that some of these comorbidities may increase the risk of PD and precede the onset of motor symptoms. Further, drugs to treat diabetes and cancer have elicited neuroprotective effects in PD models. Nonetheless, the mechanisms underlying the occurrence of these comorbidities remain elusive. Herein, we discuss the biological and clinical implications of comorbidities in the pathogenesis, progression, and clinical management, with an emphasis on personalized medicine applications for PD.
Keywords: Parkinson’s disease; anemia; cancer; comorbidities; depression; diabetes; personalized medicine.
Figures
References
Publication types
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

