Use of Tachycardia in Patients With Submassive Pulmonary Emboli to Risk Stratify for Early Initiation of Thrombolytic Therapy: A Case Series Comparing Early Versus Late Thrombolytic Initiation
- PMID: 29276710
- PMCID: PMC5734466
- DOI: 10.1177/2324709617744232
Use of Tachycardia in Patients With Submassive Pulmonary Emboli to Risk Stratify for Early Initiation of Thrombolytic Therapy: A Case Series Comparing Early Versus Late Thrombolytic Initiation
Abstract
Pulmonary embolism (PE) represents a prevalent cause of morbidity and mortality in the United States, with approximately 600 000 cases diagnosed annually. The mortality rate for untreated PE is as high as 30%. Right ventricular (RV) dysfunction is a sign of possible adverse outcomes with right-sided heart failure being the usual cause of death from PE. There is a spectrum of clinical presentations associated with PE diagnoses, from incidental and asymptomatic to rapid hemodynamic collapse. Despite successes in identifying patients with "high-risk" PEs for aggressive thrombolytic interventions and "low-risk" PEs for outpatient anticoagulation, a significant lack of consensus exists regarding intervention modalities for PEs identified as "intermediate risk" or "submassive," defined as normotensive (systolic blood pressure ≥90 mm Hg) with acute RV dysfunction and myocardial injury. In this case series, we review the management and outcomes of 2 patients with submassive PEs and sustained tachycardia in the setting of normal blood pressures, and we address the need to recognize tachycardia as an ominous RV compensatory sign, indicative of impending hemodynamic collapse, that should lead to aggressive therapy with vascular intervention.
Keywords: intermediate-risk pulmonary embolism; pulmonary embolism; right ventricular strain and PE; submassive pulmonary embolism; tachycardia and PE; thrombolytics in pulmonary embolism.
Conflict of interest statement
Declaration of Conflicting Interests: The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Figures
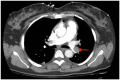
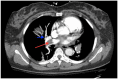
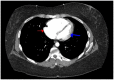
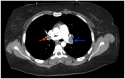
Similar articles
-
Current Controversies in Thrombolytic Use in Acute Pulmonary Embolism.J Emerg Med. 2016 Jul;51(1):37-44. doi: 10.1016/j.jemermed.2016.02.024. Epub 2016 Apr 9. J Emerg Med. 2016. PMID: 27071316
-
Thrombolytic therapy for acute pulmonary embolism: a critical appraisal.Chest. 2009 May;135(5):1321-1329. doi: 10.1378/chest.08-2125. Chest. 2009. PMID: 19420199 Review.
-
Fibrinolysis for acute pulmonary embolism.Vasc Med. 2010 Oct;15(5):419-28. doi: 10.1177/1358863X10380304. Vasc Med. 2010. PMID: 20926501 Review.
-
Usefulness of right ventricular myocardial strain in assessment of response to thrombolytic therapy in acute pulmonary embolism.Eur J Echocardiogr. 2010 Dec;11(10):892-5. doi: 10.1093/ejechocard/jeq091. Epub 2010 Sep 6. Eur J Echocardiogr. 2010. PMID: 20819837
-
Diagnosis and management of life-threatening pulmonary embolism.J Intensive Care Med. 2011 Sep-Oct;26(5):275-94. doi: 10.1177/0885066610392658. Epub 2011 May 23. J Intensive Care Med. 2011. PMID: 21606060 Review.
References
-
- Dalen JE, Alpert JS. Natural history of pulmonary embolism. Prog Cardiovasc Dis. 1975;17:259-270. - PubMed
-
- Goldhaber SZ. Thrombolysis for pulmonary embolism. N Engl J Med. 2002;347:1131-1132. - PubMed
-
- Konstantinides S, Geibel A, Heusel G, Heinrich F, Kasper W; Management Strategies and Prognosis of Pulmonary Embolism-3 Trial Investigators. Heparin plus alteplase compared with heparin alone in patients with submassive pulmonary embolism. N Engl J Med. 2002;347:1143-1150. - PubMed
-
- Jaff MR, McMurtry MS, Archer SL, et al. Management of massive and submassive pulmonary embolism, iliofemoral deep vein thrombosis, and chronic thromboembolic pulmonary hypertension: a scientific statement from the American Heart Association. Circulation. 2011;123:1788-1830. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources

