Pharmacology of Corticosteroids for Diabetic Macular Edema
- PMID: 29297055
- PMCID: PMC5961100
- DOI: 10.1167/iovs.17-22259
Pharmacology of Corticosteroids for Diabetic Macular Edema
Abstract
Purpose: Corticosteroids remain the mainstay of treatment for inflammatory diseases almost 80 years after their first clinical use. Topical ophthalmic formulations of corticosteroids have been available to treat disease of the anterior segment of the eye, but the approval of corticosteroids to treat vitreoretinal diseases, including vein occlusion, diabetic macular edema, and uveitis, has occurred only recently. Although most diseases respond to corticosteroid therapy, some patients are resistant to this therapy and side effects, including cataract and elevated intraocular pressure, can limit their use. The purpose of this review is to detail the basic science of corticosteroids focusing on differences in potency, drug delivery, pharmacokinetics, and gene activation, and how these differences affect safety and efficacy in the treatment of diabetic macular edema.
Methods: A review was conducted of basic science and pharmacology of the corticosteroids used to treat diabetic macular edema.
Results: Clinically available corticosteroids not only have differing potency and pharmacokinetics, but also activate different genes in different target tissues. These differences are associated with distinct efficacy, pharmacokinetic, and safety profiles. It is important to understand these differences in selecting corticosteroids to treat diabetic macular edema.
Conclusions: Recent advances in our understanding of the basic science of corticosteroids can explain clinical differences in these agents regarding efficacy and safety. Importantly, this understanding should allow the future discovery of additional novel corticosteroids to treat diabetic macular edema.
Figures

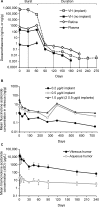



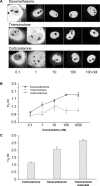
References
-
- Hench PS, Kendall EC, Slocumb CH, Polley HF. . The effect of a hormone of the adrenal cortex (17-hydroxy-11-dehydrocorticosterone; compound E) and of pituitary adrenocorticotropic hormone on rheumatoid arthritis. . 1949; 24: 181– 197. - PubMed
-
- Duke-Elder S, Perkins ES. . London: Henry Kimpton Publishers; 1966: 176.
-
- Kasper DL, Fauci AS, Hauser S, Longo D, Jameson JL, Loscalzo J. . Harrison's Principles of Internal Medicine. 19th ed. New York: McGraw Hill Professional; 2015.
-
- Nussenblatt RB, Whitcup SM. . Uveitis Fundamentals and Clinical Practice. 4th ed. Elsevier Health Sciences; 2010.
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

