Paratracheal Paraseptal Emphysema and Expiratory Central Airway Collapse in Smokers
- PMID: 29298081
- PMCID: PMC5879141
- DOI: 10.1513/AnnalsATS.201709-713OC
Paratracheal Paraseptal Emphysema and Expiratory Central Airway Collapse in Smokers
Abstract
Rationale: Expiratory central airway collapse is associated with respiratory morbidity independent of underlying lung disease. However, not all smokers develop expiratory central airway collapse, and the etiology of expiratory central airway collapse in adult smokers is unclear. Paraseptal emphysema in the paratracheal location, by untethering airway walls, may predispose smokers to developing expiratory central airway collapse.
Objectives: To evaluate whether paratracheal paraseptal emphysema is associated with expiratory central airway collapse.
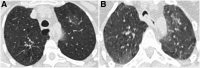
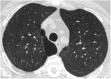
Methods: We analyzed paired inspiratory and expiratory computed tomography scans from participants enrolled in a multicenter study (Genetic Epidemiology of Chronic Obstructive Pulmonary Disease) of smokers aged 45 to 80 years. Expiratory central airway collapse was defined as greater than or equal to 50% reduction in cross-sectional area of the trachea during expiration. In a nested case-control design, participants with and without expiratory central airway collapse were included in a 1:2 fashion, and inspiratory scans were further analyzed using the Fleischner Society criteria for presence of centrilobular emphysema, paraseptal emphysema, airway wall thickening, and paratracheal paraseptal emphysema (maximal diameter ≥ 0.5 cm).
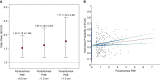
Results: A total of 1,320 patients were included, 440 with and 880 without expiratory central airway collapse. Those with expiratory central airway collapse were older, had higher body mass index, and were less likely to be men or current smokers. Paratracheal paraseptal emphysema was more frequent in those with expiratory central airway collapse than control subjects (16.6 vs. 11.8%; P = 0.016), and after adjustment for age, race, sex, body mass index, smoking pack-years, and forced expiratory volume in 1 second, paratracheal paraseptal emphysema was independently associated with expiratory central airway collapse (adjusted odds ratio, 1.53; 95% confidence interval, 1.18-1.98; P = 0.001). Furthermore, increasing size of paratracheal paraseptal emphysema (maximal diameter of at least 1 cm and 1.5 cm) was associated with greater odds of expiratory central airway collapse (adjusted odds ratio, 1.63; 95% confidence interval, 1.18-2.25; P = 0.003 and 1.77; 95% confidence interval, 1.19-2.64; P = 0.005, respectively).
Conclusions: Paraseptal emphysema adjacent to the trachea is associated with expiratory central airway collapse. The identification of this risk factor on inspiratory scans should prompt further evaluation for expiratory central airway collapse. Clinical trial registered with ClinicalTrials.gov (NCT 00608764).
Figures
Comment in
-
The Road to Precision Medicine in Chronic Obstructive Pulmonary Disease: Squeezing More Out of Chest Computed Tomography Scans.Ann Am Thorac Soc. 2018 Apr;15(4):428-429. doi: 10.1513/AnnalsATS.201712-945ED. Ann Am Thorac Soc. 2018. PMID: 29923738 Free PMC article. No abstract available.
References
-
- Murgu S, Colt H. Tracheobronchomalacia and excessive dynamic airway collapse. Clin Chest Med. 2013;34:527–555. - PubMed
-
- Kandaswamy C, Balasubramanian V. Review of adult tracheomalacia and its relationship with chronic obstructive pulmonary disease. Curr Opin Pulm Med. 2009;15:113–119. - PubMed
-
- Jokinen K, Palva T, Sutinen S, Nuutinen J. Acquired tracheobronchomalacia. Ann Clin Res. 1977;9:52–57. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

