Chemotherapy-induced metastasis: mechanisms and translational opportunities
- PMID: 29307118
- PMCID: PMC6035114
- DOI: 10.1007/s10585-017-9870-x
Chemotherapy-induced metastasis: mechanisms and translational opportunities
Abstract
Tumors often overcome the cytotoxic effects of chemotherapy through either acquired or environment-mediated drug resistance. In addition, signals from the microenvironment obfuscate the beneficial effects of chemotherapy and may facilitate progression and metastatic dissemination. Seminal mediators in chemotherapy-induced metastasis appear to be a wide range of hematopoietic, mesenchymal and immune progenitor cells, originating from the bone marrow. The actual purpose of these cells is to orchestrate the repair response to the cytotoxic damage of chemotherapy. However, these repair responses are exploited by tumor cells at every step of the metastatic cascade, ranging from tumor cell invasion, intravasation and hematogenous dissemination to extravasation and effective colonization at the metastatic site. A better understanding of the mechanistic underpinnings of chemotherapy-induced metastasis will allow us to better predict which patients are more likely to exhibit pro-metastatic responses to chemotherapy and will help develop new therapeutic strategies to neutralize chemotherapy-driven prometastatic changes.
Keywords: Bone marrow-derived cells; Cancer cell dissemination; Macrophages; MenaCalc; Mesenchymal stem cells; TMEM.
Conflict of interest statement
MHO and JSC are inventors on a patent application (#96700/2505) submitted by the Albert Einstein College of Medicine that covers methods detecting and reducing chemotherapy-induced prometastatic changes in breast tumors. GSK declares no competing interests.
Figures

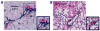
References
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

