Decreased Lung Function and All-Cause Mortality in HIV-infected Individuals
- PMID: 29313714
- PMCID: PMC5822404
- DOI: 10.1513/AnnalsATS.201606-492OC
Decreased Lung Function and All-Cause Mortality in HIV-infected Individuals
Abstract
Rationale: Human immunodeficiency virus (HIV) infection is associated with pulmonary disease and worse lung function, but the relationship of lung function with survival in HIV is unknown.
Objectives: To determine whether lung function is associated with all-cause mortality in HIV-infected individuals.
Methods: HIV-infected participants from cohorts in three locations underwent pre- and post-bronchodilator spirometry and determination of single-breath diffusing capacity of the lung for carbon monoxide (DlCO) in 2008-2009, computed tomographic (CT) scanning of the chest for quantitative emphysema and airway measures, and echocardiography for estimated left ventricular systolic and diastolic function and tricuspid regurgitant velocity. Bivariate analysis and multivariable Cox proportional hazards models were used to determine whether decreased lung function was independently associated with increased all-cause mortality. Models were adjusted for covariates including age, sex, body mass index, smoking status, self-reported hepatitis C status, HIV viral levels, CD4+ T-cell counts, hemoglobin, antiretroviral therapy, and illicit drug use.
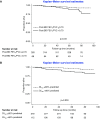
Results: Overall, 396 HIV-infected participants underwent pulmonary function testing. Thirty-two participants (8%) died during a median follow-up period of 69 months. A post-bronchodilator FEV1-to-FVC ratio less than 0.7 (hazard ratio [HR], 2.47; 95% confidence interval [CI], 1.10-5.58) and a DlCO less than 60% (HR, 2.28; 95% CI, 1.08-4.82) were independently associated with worse mortality. Also, hepatitis C (HR, 2.68; 95% CI, 1.22-5.89) and baseline plasma HIV RNA level (HR per ln RNA copies/ml, 1.50; 95% CI, 1.22-1.86) were associated with mortality in HIV-infected participants. The only CT or echocardiographic measure associated with greater mortality in univariate analysis was greater wall thickness of medium-sized airways (HR for wall area percent, 1.08; 95% CI, 1.00-1.18; P = 0.051), but none of the CT or echocardiogram measures were associated with mortality in multivariable analysis.
Conclusions: Airflow obstruction and impaired diffusing capacity appear to be associated with all-cause mortality in HIV-infected persons over an average of 6 years of follow-up. These data highlight the importance of lung dysfunction in HIV-infected persons and should be confirmed in larger cohorts and with extended follow-up periods. Clinical trial registered with www.clinicaltrials.gov (NCT00869544, NCT01326572).
Keywords: HIV; acquired immunodeficiency syndrome; chronic obstructive pulmonary disease.
Figures
Comment in
-
Abnormal Lung Function in HIV-infected Adults: An Under-recognized Risk Factor for Early Mortality.Ann Am Thorac Soc. 2018 Feb;15(2):160-162. doi: 10.1513/AnnalsATS.201711-904ED. Ann Am Thorac Soc. 2018. PMID: 29388812 Free PMC article. No abstract available.
References
-
- Helleberg M, Afzal S, Kronborg G, Larsen CS, Pedersen G, Pedersen C, et al. Mortality attributable to smoking among HIV-1–infected individuals: a nationwide, population-based cohort study. Clin Infect Dis. 2013;56:727–734. - PubMed
-
- Palella FJ, Jr, Baker RK, Moorman AC, Chmiel JS, Wood KC, Brooks JT, et al. HIV Outpatient Study Investigators. Mortality in the highly active antiretroviral therapy era: changing causes of death and disease in the HIV outpatient study. J Acquir Immune Defic Syndr. 2006;43:27–34. - PubMed
-
- Walensky RP, Paltiel AD, Losina E, Mercincavage LM, Schackman BR, Sax PE, et al. The survival benefits of AIDS treatment in the United States. J Infect Dis. 2006;194:11–19. - PubMed
-
- World Health Organization. The top 10 causes of death. 2016 [updated 2017 Jan; accessed 2016 Mar 10]. Available from: http://www.who.int/mediacentre/factsheets/fs310/en/
-
- Neas LM, Schwartz J. Pulmonary function levels as predictors of mortality in a national sample of US adults. Am J Epidemiol. 1998;147:1011–1018. - PubMed
Publication types
MeSH terms
Substances
Associated data
Grants and funding
- K24 HL123342/HL/NHLBI NIH HHS/United States
- UL1 TR000005/TR/NCATS NIH HHS/United States
- R01 HL083461/HL/NHLBI NIH HHS/United States
- U01 AI034989/AI/NIAID NIH HHS/United States
- U01 AI035041/AI/NIAID NIH HHS/United States
- K23 HL108697/HL/NHLBI NIH HHS/United States
- UM1 AI035043/AI/NIAID NIH HHS/United States
- K24 HL087713/HL/NHLBI NIH HHS/United States
- UL1 TR000454/TR/NCATS NIH HHS/United States
- UL1 TR000424/TR/NCATS NIH HHS/United States
- U01 AI035040/AI/NIAID NIH HHS/United States
- UL1 TR000004/TR/NCATS NIH HHS/United States
- R01 HL120398/HL/NHLBI NIH HHS/United States
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials

