Patient Preferences for Surgery or Antibiotics for the Treatment of Acute Appendicitis
- PMID: 29322168
- PMCID: PMC5875347
- DOI: 10.1001/jamasurg.2017.5310
Patient Preferences for Surgery or Antibiotics for the Treatment of Acute Appendicitis
Abstract
Importance: Studies have compared surgical with nonsurgical therapy for acute uncomplicated appendicitis, but none of these studies have a patient-centered perspective.
Objectives: To evaluate how patients might choose between surgical and nonsurgical therapy for acute uncomplicated appendicitis and to identify targets to make antibiotic treatment more appealing.
Design, setting, and participants: This study comprised an online survey and an in-person sensitivity analysis survey. For the web survey, a convenience sample of 1728 respondents were asked to imagine that they or their child had acute uncomplicated appendicitis, provided information about laparoscopic and open appendectomy and antibiotic treatment alone, and asked which treatment they might choose. The web survey was open from April 17, 2016, through June 16, 2016, and was disseminated via email link, a poster with a Quick Response code, and social media. For the sensitivity analysis, 220 respondents were given the same scenario and options. Those who chose surgery were asked whether certain factors influenced their decision; each factor was incrementally improved during questioning about whether respondents would consider switching to antibiotics. These participants were recruited at public venues from June 3, 2016, to July 31, 2016. Web survey data were analyzed from June 17, 2016, to September 21, 2017. Sensitivity analysis data were analyzed from August 1, 2016, to September 21, 2017.
Main outcomes and measures: Treatment preferences.
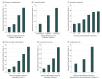
Results: Among the 1728 web survey respondents, 1225 (70.9%) were female and 500 (28.9%) were male (3 [0.2%] either did not answer or responded as "gender fluid" within the comments section of the survey), and most self-reported being between 50 and 59 years of age (391 [22.6%]) and being non-Hispanic white (1563 [90.5%]). For themselves, 1482 respondents (85.8%) chose laparoscopic appendectomy, 84 (4.9%) chose open appendectomy, and 162 (9.4%) chose antibiotics alone. For their child, 1372 respondents (79.4%) chose laparoscopic appendectomy, 106 (6.1%) open appendectomy, and 250 (14.5%) antibiotics alone. Respondents were somewhat more likely to choose antibiotics for themselves if they had education beyond college (105 [12.6%]; P < .001), identified as other than non-Hispanic white (24 [14.9%]; P < .001), or did not know anyone who had previously been hospitalized (12 [15.8%]; P = .02), but they were less likely to choose antibiotics if they were surgeons (11 [5.4%]; P = .008). Of the 220 participants interviewed for the sensitivity analysis, 120 (54.5%) were female and 100 (45.5%) were male, and most self-reported being between 18 and 24 years of age (53 [24.1%]) and being non-Hispanic white (204 [92.7%]). Their responses suggested that improvements in the short- and long-term failure rate of antibiotic treatment-rather than reductions in the duration of hospitalization or antibiotic treatment-were more likely to increase the desirability of choosing antibiotics.
Conclusions and relevance: Most patients may choose surgical intervention over antibiotics alone in treatment of acute uncomplicated appendicitis, but a meaningful number may choose nonoperative management. Therefore, from a patient-centered perspective, this option should be discussed with patients, and future research could be directed at reducing the failure and recurrence rates of antibiotic treatment for appendicitis.
Conflict of interest statement
Figures
Comment in
-
Questionable Assumptions Provided in Nonoperative Treatment of Appendicitis Survey.JAMA Surg. 2018 Oct 1;153(10):969-970. doi: 10.1001/jamasurg.2018.2060. JAMA Surg. 2018. PMID: 29971340 No abstract available.
-
Questionable Assumptions Provided in Nonoperative Treatment of Appendicitis Survey-Reply.JAMA Surg. 2018 Oct 1;153(10):970. doi: 10.1001/jamasurg.2018.2063. JAMA Surg. 2018. PMID: 29971345 No abstract available.
References
-
- Minneci PC, Mahida JB, Lodwick DL, et al. . Effectiveness of patient choice in nonoperative vs surgical management of pediatric uncomplicated acute appendicitis. JAMA Surg. 2016;151(5):408-415. - PubMed
-
- Georgiou R, Eaton S, Stanton MP, Pierro A, Hall NJ. Efficacy and safety of nonoperative treatment for acute appendicitis: a meta-analysis. Pediatrics. 2017;139(3):e20163003. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous