Race and Socioeconomic Status Independently Affect Risk of Major Amputation in Peripheral Artery Disease
- PMID: 29330260
- PMCID: PMC5850162
- DOI: 10.1161/JAHA.117.007425
Race and Socioeconomic Status Independently Affect Risk of Major Amputation in Peripheral Artery Disease
Abstract
Background: Black race has been shown to be a risk factor for amputation in peripheral artery disease (PAD); however, race has been argued to be a marker for socioeconomic status (SES) rather than true disparity. The aim of this study is to study the impact of race and SES on amputation risk in PAD patients.
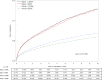
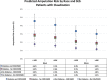
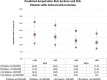
Methods and results: Patients with incident PAD in the national Veterans Affairs Corporate Data Warehouse were identified from 2003 to 2014 (N=155 647). The exposures were race and SES (measured by median income in residential ZIP codes). The outcome was incident major amputation. Black veterans were significantly more likely to live in low-SES neighborhoods and to present with advanced PAD. Black patients had a higher amputation risk in each SES stratum compared with white patients. In Cox models (adjusting for covariates), black race was associated with a 37% higher amputation risk compared with white race (hazard ratio: 1.37; 95% confidence interval, 1.30-1.45), whereas low SES was independently predictive of increased risk of amputation (hazard ratio: 1.12; 95% confidence interval, 1.06-1.17) and showed no evidence of interaction with race. In predicted amputation risk analysis, black race and low SES continued to be significant risk factors for amputation regardless of PAD presentation.
Conclusions: Black race significantly increases the risk of amputation within the same SES stratum compared with white race and has an independent effect on limb loss after controlling for comorbidities, severity of PAD at presentation, and use of medications.
Keywords: amputations; disparities; race; socioeconomic position.
© 2018 The Authors. Published on behalf of the American Heart Association, Inc., by Wiley.
Figures
References
-
- Fowkes FG, Rudan D, Rudan I, Aboyans V, Denenberg JO, McDermott MM, Norman PE, Sampson UK, Williams LJ, Mensah GA, Criqui MH. Comparison of global estimates of prevalence and risk factors for peripheral artery disease in 2000 and 2010: a systematic review and analysis. Lancet. 2013;382:1329–1340. - PubMed
-
- Allison MA, Ho E, Denenberg JO, Langer RD, Newman AB, Fabsitz RR, Criqui MH. Ethnic‐specific prevalence of peripheral arterial disease in the United States. Am J Prev Med. 2007;32:328–333. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

