Functional Knowledge of Pre-Exposure Prophylaxis for HIV Prevention Among Participants in a Web-Based Survey of Sexually Active Gay, Bisexual, and Other Men Who Have Sex With Men: Cross-Sectional Study
- PMID: 29362213
- PMCID: PMC5801519
- DOI: 10.2196/publichealth.8089
Functional Knowledge of Pre-Exposure Prophylaxis for HIV Prevention Among Participants in a Web-Based Survey of Sexually Active Gay, Bisexual, and Other Men Who Have Sex With Men: Cross-Sectional Study
Abstract
Background: Awareness of pre-exposure prophylaxis (PrEP) for HIV prevention is increasing, but little is known about the functional knowledge of PrEP and its impact on willingness to use PrEP.
Objective: The objective of this study was to assess the functional knowledge of PrEP among a sample of gay, bisexual, and other men who have sex with men (MSM) participating in a Web-based survey of sexually active MSM.
Methods: Men at least 18 years old, residing in the United States, and reporting sex with a man in the previous 6 months were recruited through social networking websites. PrEP functional knowledge included the following 4 questions (1) efficacy of consistent PrEP use, (2) inconsistent PrEP use and effectiveness, (3) PrEP and condom use, and (4) effectiveness at reducing sexually transmitted infections (STIs). Ordinal logistic regression was used to identify respondent characteristics associated with PrEP functional knowledge. In a subsample of participants responding to HIV prevention questions, we compared willingness to use PrEP by response to PrEP functional knowledge using logistic regression analysis adjusted for age, race and ethnicity, and education level.
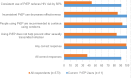
Results: Among 573 respondents, PrEP knowledge was high regarding adherence (488/573, 85.2%), condom use (532/573, 92.8%), and STIs (480/573, 83.8%), but only 252/573 (44.0%) identified the correct efficacy. Lower functional PrEP knowledge was associated with minority race/ethnicity (P=.005), lower education (P=.01), and not having an HIV test in the past year (P=.02). Higher PrEP knowledge was associated with willingness to use PrEP (P=.009). Younger age was not associated with higher PrEP functional knowledge or willingness to use PrEP.
Conclusions: PrEP knowledge was generally high in our study, including condom use and consistent use but may be lacking in higher risk MSM. The majority of respondents did not correctly identify PrEP efficacy with consistent use, which could impact motivation to seek out PrEP for HIV prevention. Targeted messaging to increase PrEP knowledge may increase PrEP use.
Keywords: human immunodeficiency virus; men who have sex with men; pre-exposure prophylaxis (PrEP).
©Erin M Kahle, Stephen Sullivan, Rob Stephenson. Originally published in JMIR Public Health and Surveillance (http://publichealth.jmir.org), 23.01.2018.
Conflict of interest statement
Conflicts of Interest: None declared.
Figures

Similar articles
-
Factors Associated With Willingness to Use Pre-Exposure Prophylaxis in Brazil, Mexico, and Peru: Web-Based Survey Among Men Who Have Sex With Men.JMIR Public Health Surveill. 2019 Jun 17;5(2):e13771. doi: 10.2196/13771. JMIR Public Health Surveill. 2019. PMID: 31210143 Free PMC article.
-
Awareness and Willingness to Use HIV Infection Pre-Exposure Prophylaxis among Rwandan Men Who Have Sex with Men: Findings from a Web-based Survey.medRxiv [Preprint]. 2023 Nov 1:2023.11.01.23297747. doi: 10.1101/2023.11.01.23297747. medRxiv. 2023. Update in: Front Public Health. 2024 Mar 01;12:1325029. doi: 10.3389/fpubh.2024.1325029. PMID: 37961327 Free PMC article. Updated. Preprint.
-
Awareness and willingness to use pre-exposure prophylaxis for HIV prevention among men who have sex with men in Rwanda: findings from a web-based survey.Front Public Health. 2024 Mar 1;12:1325029. doi: 10.3389/fpubh.2024.1325029. eCollection 2024. Front Public Health. 2024. PMID: 38496393 Free PMC article.
-
Bridging Awareness and Acceptance of Pre-Exposure Prophylaxis Among Men Who Have Sex With Men and the Need for Targeting Chemsex and HIV Testing: Cross-Sectional Survey.JMIR Public Health Surveill. 2019 Jul 3;5(3):e13083. doi: 10.2196/13083. JMIR Public Health Surveill. 2019. PMID: 31271148 Free PMC article.
-
HIV Pre-exposure Prophylaxis in the LGBTQ Community: A Review of Practice and Places.Cureus. 2021 Jun 8;13(6):e15518. doi: 10.7759/cureus.15518. eCollection 2021 Jun. Cureus. 2021. PMID: 34249580 Free PMC article. Review.
Cited by
-
Knowledge of Human Mpox (Monkeypox) and Attitude towards Mpox Vaccination among Male Sex Workers in China: A Cross-Sectional Study.Vaccines (Basel). 2023 Jan 28;11(2):285. doi: 10.3390/vaccines11020285. Vaccines (Basel). 2023. PMID: 36851163 Free PMC article.
-
Awareness of, willingness to use, and experiences with Pre-exposure prophylaxis among youth in Nigeria.BMC Health Serv Res. 2024 Sep 27;24(1):1128. doi: 10.1186/s12913-024-11459-1. BMC Health Serv Res. 2024. PMID: 39334111 Free PMC article.
-
Awareness and use of pre-exposure and postexposure prophylaxes among Nigerian university students: Findings from a cross-sectional survey.Medicine (Baltimore). 2018 Sep;97(36):e12226. doi: 10.1097/MD.0000000000012226. Medicine (Baltimore). 2018. PMID: 30200145 Free PMC article.
-
Pre-exposure prophylaxis engagement among sexual minority men in Taiwan: a behavioral health perspective.J Behav Med. 2025 Aug;48(4):694-705. doi: 10.1007/s10865-025-00572-z. Epub 2025 May 10. J Behav Med. 2025. PMID: 40348939
-
Interest in Taking HIV Pre-exposure Prophylaxis Is Associated with Behavioral Risk Indicators and Self-Perceived HIV Risk Among Men Who Have Sex with Men Attending HIV Testing Venues in Sweden.Arch Sex Behav. 2020 Aug;49(6):2165-2177. doi: 10.1007/s10508-020-01740-9. Epub 2020 Jun 3. Arch Sex Behav. 2020. PMID: 32495243 Free PMC article.
References
-
- Baeten JM, Donnell D, Ndase P, Mugo NR, Campbell JD, Wangisi J, Tappero JW, Bukusi EA, Cohen CR, Katabira E, Ronald A, Tumwesigye E, Were E, Fife KH, Kiarie J, Farquhar C, John-Stewart G, Kakia A, Odoyo J, Mucunguzi A, Nakku-Joloba E, Twesigye R, Ngure K, Apaka C, Tamooh H, Gabona F, Mujugira A, Panteleeff D, Thomas KK, Kidoguchi L, Krows M, Revall J, Morrison S, Haugen H, Emmanuel-Ogier M, Ondrejcek L, Coombs RW, Frenkel L, Hendrix C, Bumpus NN, Bangsberg D, Haberer JE, Stevens WS, Lingappa JR, Celum C, Partners PST. Antiretroviral prophylaxis for HIV prevention in heterosexual men and women. N Engl J Med. 2012 Aug 2;367(5):399–410. doi: 10.1056/NEJMoa1108524. http://europepmc.org/abstract/MED/22784037 - DOI - PMC - PubMed
-
- Grant RM, Lama JR, Anderson PL, McMahan V, Liu AY, Vargas L, Goicochea P, Casapía M, Guanira-Carranza JV, Ramirez-Cardich ME, Montoya-Herrera O, Fernández T, Veloso VG, Buchbinder SP, Chariyalertsak S, Schechter M, Bekker L, Mayer KH, Kallás EG, Amico KR, Mulligan K, Bushman LR, Hance RJ, Ganoza C, Defechereux P, Postle B, Wang F, McConnell JJ, Zheng J, Lee J, Rooney JF, Jaffe HS, Martinez AI, Burns DN, Glidden DV, iPrEx ST. Preexposure chemoprophylaxis for HIV prevention in men who have sex with men. N Engl J Med. 2010 Dec 30;363(27):2587–99. doi: 10.1056/NEJMoa1011205. http://europepmc.org/abstract/MED/21091279 - DOI - PMC - PubMed
-
- Thigpen MC, Kebaabetswe PM, Paxton LA, Smith DK, Rose CE, Segolodi TM, Henderson FL, Pathak SR, Soud FA, Chillag KL, Mutanhaurwa R, Chirwa LI, Kasonde M, Abebe D, Buliva E, Gvetadze RJ, Johnson S, Sukalac T, Thomas VT, Hart C, Johnson JA, Malotte CK, Hendrix CW, Brooks JT, TDF2 SG. Antiretroviral preexposure prophylaxis for heterosexual HIV transmission in Botswana. N Engl J Med. 2012 Aug 2;367(5):423–34. doi: 10.1056/NEJMoa1110711. - DOI - PubMed
-
- United States Food and Drug Administration [2018-01-08]. FDA approves first drug for reducing the risk of sexually acquired HIV infection https://aidsinfo.nih.gov/news/1254/fda-approves-first-drug-for-reducing-... 6wJxGm695.
-
- Liu AY, Cohen SE, Vittinghoff E, Anderson PL, Doblecki-Lewis S, Bacon O, Chege W, Postle BS, Matheson T, Amico KR, Liegler T, Rawlings MK, Trainor N, Blue RW, Estrada Y, Coleman ME, Cardenas G, Feaster DJ, Grant R, Philip SS, Elion R, Buchbinder S, Kolber MA. Preexposure prophylaxis for HIV infection integrated with municipal- and community-based sexual health services. J Am Med Assoc Intern Med. 2016 Jan;176(1):75–84. doi: 10.1001/jamainternmed.2015.4683. http://europepmc.org/abstract/MED/26571482 - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

