Extended-Release Naltrexone Improves Viral Suppression Among Incarcerated Persons Living With HIV With Opioid Use Disorders Transitioning to the Community: Results of a Double-Blind, Placebo-Controlled Randomized Trial
- PMID: 29373393
- PMCID: PMC5889326
- DOI: 10.1097/QAI.0000000000001634
Extended-Release Naltrexone Improves Viral Suppression Among Incarcerated Persons Living With HIV With Opioid Use Disorders Transitioning to the Community: Results of a Double-Blind, Placebo-Controlled Randomized Trial
Abstract
Objective: To determine whether extended-release naltrexone (XR-NTX) would improve or maintain viral suppression (VS) among prisoners or jail detainees with HIV and opioid use disorder (OUD) transitioning to the community.
Design: A 4-site, prospective randomized double-blind, placebo-controlled trial was conducted among prison and jail inmates with HIV and OUD transitioning to the community from September 2010 through March 2016.
Methods: Eligible participants (N = 93) were randomized 2:1 to receive 6 monthly injections of XR-NTX (n = 66) or placebo (n = 27) starting at release and observed for 6 months. The primary outcome was the proportion that maintained or improved VS (<50 copies/mL) from baseline to 6 months.
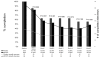
Results: Participants allocated to XR-NTX significantly improved to VS (<50 copies/mL) from baseline (37.9%) to 6 months (60.6%) (P = 0.002), whereas the placebo group did not (55.6% at baseline to 40.7% at 6 months P = 0.294). There was, however, no statistical significant difference in VS levels at 6 months between XR-NTX (60.6%) vs. placebo (40.7%) (P = 0.087). After controlling for other factors, only allocation to XR-NTX (adjusted odds ratio = 2.90; 95% confidence interval = 1.04 to 8.14, P = 0.043) was associated with the primary outcome. Trajectories in VS from baseline to 6 months differed significantly (P = 0.017) between treatment groups, and the differences in the discordant values were significantly different as well (P = 0.041): the XR-NTX group was more likely than the placebo group to improve VS (30.3% vs. 18.5%), maintain VS (30.3% vs. 27.3), and less likely to lose VS (7.6% vs. 33.3%) by 6 months.
Conclusions: XR-NTX improves or maintains VS after release to the community for incarcerated people living with HIV with OUD.
Trial registration: ClinicalTrials.gov NCT01246401.
Figures


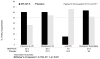

References
-
- Thompson MA, Mugavero MJ, Amico KR, et al. Guidelines for improving entry into and retention in care and antiretroviral adherence for persons with HIV: evidence-based recommendations from an International Association of Physicians in AIDS Care panel. Ann Intern Med. 2012;156(11):817–833. W–284, W–285, W–286, W–287, W–288, W–289, W–290, W–291, W–292, W–293, W–294. - PMC - PubMed
-
- Peters RH, Greenbaum PE, Edens JF, Carter CR, Ortiz MM. Prevalence of DSM-IV substance abuse and dependence disorders among prison inmates. Am J Drug Alcohol Abuse. 1998;24(4):573–587. - PubMed
Publication types
MeSH terms
Substances
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

