Anterior scleritis following intravitreal injections in a patient with rheumatoid arthritis: A case report
- PMID: 29382031
- PMCID: PMC5709030
- DOI: 10.1097/MD.0000000000008925
Anterior scleritis following intravitreal injections in a patient with rheumatoid arthritis: A case report
Abstract
Rationale: Surgically induced scleritis is a rare complication following ophthalmologic surgery such as cataract surgery, pterygium excision, strabismus surgery, and retinal detachment repair. Rheumatoid arthritis (RA) is the connective tissue disease most commonly associated with scleritis.
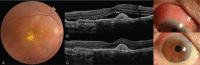
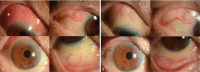
Patient concerns: A 70-year-old woman visited our clinic with complaint of visual disturbance, ocular pain, and conjunctival injection in her right eye of 1 month's duration. She had a stable state of rheumatoid factor positive RA and had a history of multiple intravitreal injections placed in the symptomatic right eye due to age-related macular degeneration.
Diagnoses: Anterior scleritis induced by multiple intravitreal injections.
Interventions: Topical and systemic steroids were administered.
Outcomes: Her symptoms and signs were relieved and no significant recurrence has been occurred with the maintenance of low dose oral steroid.
Lessons: Surgically induced scleritis can also be induced by not only major surgical trauma but also by relatively minor trauma such as intravitreal injection (especially in patients who have connective tissue disease such as RA).
Copyright © 2017 The Authors. Published by Wolters Kluwer Health, Inc. All rights reserved.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
Similar articles
-
Fungal Necrotizing Scleritis After Intravitreal Injection Therapy.Cornea. 2021 Dec 1;40(12):1617-1619. doi: 10.1097/ICO.0000000000002670. Cornea. 2021. PMID: 34749383 Review.
-
Scleritis following intravitreal brolucizumab injection: a case series.J Med Case Rep. 2024 Feb 29;18(1):80. doi: 10.1186/s13256-024-04402-9. J Med Case Rep. 2024. PMID: 38419100 Free PMC article.
-
A case of scleritis associated rheumatoid arthritis accompanying an intraocular elevated lesion.BMC Ophthalmol. 2018 May 30;18(1):129. doi: 10.1186/s12886-018-0797-z. BMC Ophthalmol. 2018. PMID: 29843653 Free PMC article.
-
Surgically induced necrotizing scleritis after pterygium excision and conjunctival autograft.Cornea. 2002 Apr;21(3):305-7. doi: 10.1097/00003226-200204000-00013. Cornea. 2002. PMID: 11917181
-
Necrotizing Scleritis and Rheumatoid Arthritis: A Clinical Case Report Supported by A Brief Review with Risk of Bias Analysis.Curr Rheumatol Rev. 2023 Jun 5;19(3):367-372. doi: 10.2174/1573397119666230222093007. Curr Rheumatol Rev. 2023. PMID: 36809968
Cited by
-
Rheumatoid Arthritis Associated Episcleritis and Scleritis: An Update on Treatment Perspectives.J Clin Med. 2021 May 14;10(10):2118. doi: 10.3390/jcm10102118. J Clin Med. 2021. PMID: 34068884 Free PMC article. Review.
-
Posterior scleritis after biweekly aflibercept intravitreal injections.Am J Ophthalmol Case Rep. 2022 Sep 6;28:101696. doi: 10.1016/j.ajoc.2022.101696. eCollection 2022 Dec. Am J Ophthalmol Case Rep. 2022. PMID: 36118279 Free PMC article.
References
-
- Akpek EK, Thorne JE, Qazi FA, et al. Evaluation of patients with scleritis for systemic disease. Ophthalmology 2004;111:501–6. - PubMed
-
- Wilhelmus K. Scleritis Associated with Rheumatoid-Arthritis and with Other Systemic Immune-Mediated Diseases-Discussion. Vol 101 Philadelphia, PA: Lippincott-Raven Publ; 1994:1287–1288. - PubMed
-
- Maffett MJ, Johns KJ, Parrish CM, et al. Sterile corneal ulceration after cataract extraction in patients with collagen vascular disease. Cornea 1990;9:279–85. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

