Can a supervised algorithmic assessment of men for prostate cancer improve the quality of care? A retrospective evaluation of a prostate assessment pathway in Saskatchewan
- PMID: 29382455
- PMCID: PMC5798437
- DOI: 10.5489/cuaj.4237
Can a supervised algorithmic assessment of men for prostate cancer improve the quality of care? A retrospective evaluation of a prostate assessment pathway in Saskatchewan
Abstract
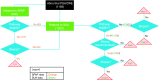
Introduction: The Saskatoon Prostate Assessment Pathway (SPAP) was developed in 2013 in part to decrease the wait times between physician referral and biopsy for patients with suspected prostate cancer. Using an algorithm carefully designed to optimize appropriate prostate biopsy rates, physicians can directly refer patients for biopsy through the SPAP without seeing a urologist. All other patients are referred to the Saskatoon Urology Associates (SUA). The present study evaluates the performance of the algorithm.
Methods: 971 patients seen at the SUA and 302 patients seen through the SPAP were identified. Information on age, biopsy status and outcome, risk stratification, and time between referral and biopsy was collected. Biopsy wait time data was analyzed using gamma distribution. Association between referral method and biopsy rate, and between referral method and risk stratification, was analyzed using Z-test.
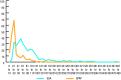
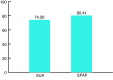
Results: The expected wait time from referral to biopsy for patients seen through SUA was 2.63 times longer than those seen through SPAP (34 vs. 91 days). The biopsy rate of patients seen in the SPAP was significantly higher than those by SUA (88% vs. 69%, 95% confidence interval [CI] 0.14-0.26; p<0.00001). There was no significant difference in positive biopsy rates for patients seen through the SPAP vs. SUA (81% vs. 74%, 95% CI -0.011,0.14; p=0.095), for detection of low-risk cancer, (12% vs. 10%, 95% CI -0.034,0.080; p=0.44), or for clinically relevant cancer, i.e., intermediate- and high-risk cancer, for SPAP vs. SUA (56.54% vs. 56.68%, 95% CI -0.091,0.089; p=0.49).
Conclusions: The algorithm used in the SPAP is effective in decreasing wait time to prostate biopsy and has the same cancer/pre-cancer detection rate, but at the cost of a higher biopsy rate. Both referral mechanisms result in few low-risk cancer detection biopsies, finding primarily cases of high- or intermediate-risk cancer.
Conflict of interest statement
Figures


Similar articles
-
Not All Multiparametric Magnetic Resonance Imaging-targeted Biopsies Are Equal: The Impact of the Type of Approach and Operator Expertise on the Detection of Clinically Significant Prostate Cancer.Eur Urol Oncol. 2018 Jun;1(2):120-128. doi: 10.1016/j.euo.2018.02.002. Epub 2018 May 15. Eur Urol Oncol. 2018. PMID: 31100235
-
Assessment of the Diagnostic Accuracy of Biparametric Magnetic Resonance Imaging for Prostate Cancer in Biopsy-Naive Men: The Biparametric MRI for Detection of Prostate Cancer (BIDOC) Study.JAMA Netw Open. 2018 Jun 1;1(2):e180219. doi: 10.1001/jamanetworkopen.2018.0219. JAMA Netw Open. 2018. PMID: 30646066 Free PMC article.
-
The 4Kscore® Test Reduces Prostate Biopsy Rates in Community and Academic Urology Practices.Rev Urol. 2015;17(4):231-40. Rev Urol. 2015. PMID: 26839521 Free PMC article.
-
Is magnetic resonance imaging-targeted biopsy a useful addition to systematic confirmatory biopsy in men on active surveillance for low-risk prostate cancer? A systematic review and meta-analysis.BJU Int. 2018 Dec;122(6):946-958. doi: 10.1111/bju.14358. Epub 2018 Jun 6. BJU Int. 2018. PMID: 29679430
-
Pretherapeutic evaluation of patients with upper gastrointestinal tract cancer using endoscopic and laparoscopic ultrasonography.Dan Med J. 2012 Dec;59(12):B4568. Dan Med J. 2012. PMID: 23290296 Review.
References
-
- Canadian Strategy for Cancer Control Governing Council. Health Canada. 2006. Canadian Strategy for Cancer Control: A Cancer Plan for Canada.
-
- Stevens C, Bondy SJ, Loblaw DA. Wait times in prostate cancer diagnosis and radiation treatment. Can Urol Assoc J. 2010;4:243–8. https://doi.org/10.5489/cuaj.09122. - DOI - PMC - PubMed
-
- Schröder F, Kattan MW. The comparability of models for predicting the risk of a positive prostate biopsy with prostate-specific antigen alone: A systematic review. Eur Urol. 2008;54:274–90. https://doi.org/10.1016/j.eururo.2008.05.022. - DOI - PubMed
-
- Finne P, Finne R, Bangma C, et al. Algorithms based on prostate-specific antigen (PSA), free PSA, digital rectal examination, and prostate volume reduce false-positive PSA results in prostate cancer screening. Int J Cancer. 2004;111:310–5. https://doi.org/10.1002/ijc.20250. - DOI - PubMed
-
- Brocken P, Prins JB, Dekhuijzen PNR, et al. The faster the better? A systematic review on distress in the diagnostic phase of suspected cancer, and the influence of rapid diagnostic pathways. Psychooncology. 2012;21:1–10. https://doi.org/10.1002/pon.1929. - DOI - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources
