Integrating community-based health promotion programs and primary care: a mixed methods analysis of feasibility
- PMID: 29386034
- PMCID: PMC5793407
- DOI: 10.1186/s12913-018-2866-7
Integrating community-based health promotion programs and primary care: a mixed methods analysis of feasibility
Abstract
Background: Implementation of evidence-based programs (EBPs) for disease self-management and prevention is a policy priority. It is challenging to implement EBPs offered in community settings and to integrate them with healthcare. We sought to understand, categorize, and richly describe key challenges and opportunities related to integrating EBPs into routine primary care practice in the United States.
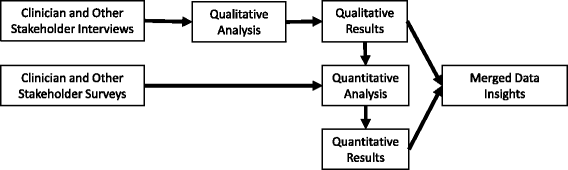
Methods: As part of a parent, participatory action research project, we conducted a mixed methods evaluation guided by the PRECEDE implementation planning model in an 11-county region of Southeast Minnesota. Our community-partnered research team interviewed and surveyed 15 and 190 primary care clinicians and 15 and 88 non-clinician stakeholders, respectively. We coded interviews according to pre-defined PRECEDE factors and by participant type and searched for emerging themes. We then categorized survey items-before looking at participant responses-according to their ability to generate further evidence supporting the PRECEDE factors and emerging themes. We statistically summarized data within and across responder groups. When consistent, we merged these with qualitative insight.
Results: The themes we found, "Two Systems, Two Worlds," "Not My Job," and "Seeing is Believing," highlighted the disparate nature of prescribed activities that different stakeholders do to contribute to health. For instance, primary care clinicians felt pressured to focus on activities of diagnosis and treatment and did not imagine ways in which EBPs could contribute to either. Quantitative analyses supported aspects of all three themes, highlighting clinicians' limited trust in community-placed activities, and the need for tailored education and system and policy-level changes to support their integration with primary care.
Conclusions: Primary care and community-based programs exist in disconnected worlds. Without urgent and intentional efforts to bridge well-care and sick-care, interventions that support people's efforts to be and stay well in their communities will remain outside of-if not at odds with-healthcare.
Keywords: CBPR; Chronic disease management; Chronic disease self-management program; Clinic-community linkages; Community-based participatory research; Evidence-based programs; Implementation; Mixed methods; Primary care.
Conflict of interest statement
Authors’ information
ALL is a physician and implementation scientist in the Knowledge and Evaluation Research Unit at Mayo Clinic.
Ethics approval and consent to participate
This study was approved by the Mayo Clinic Institutional Review Board through its Office of Community Engagement in Research under exempt status. All participants gave consent to participate in this study. The reference number for the study is: 15–002587-03
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Figures
References
-
- Cunningham PJ. Chronic burdens: the persistently high out-of-pocket health care expenses faced by many Americans with chronic conditions. Issue Brief (Commonw Fund) 2009;63:1–14. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical