Blood will out: vascular contributions to Alzheimer's disease
- PMID: 29388925
- PMCID: PMC5785254
- DOI: 10.1172/JCI97509
Blood will out: vascular contributions to Alzheimer's disease
Abstract
The fundamental pathology in Alzheimer's disease (AD) is neuronal dysfunction leading to cognitive impairment. The amyloid-β peptide (Aβ), derived from amyloid precursor protein, is one driver of AD, but how it leads to neuronal dysfunction is not established. In this Review, I discuss the complexity of AD and possible cause-and-effect relationships between Aβ and the vascular and hemostatic systems. AD can be considered a multifactorial syndrome with various contributing pathological mechanisms. Therefore, as is routinely done with cancer, it will be important to classify patients with respect to their disease signature so that specific pathologies, including vascular pathways, can be therapeutically targeted.
Conflict of interest statement
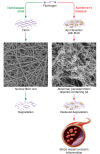
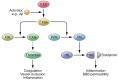
Figures

Similar articles
-
The Alzheimer's disease peptide β-amyloid promotes thrombin generation through activation of coagulation factor XII.J Thromb Haemost. 2016 May;14(5):995-1007. doi: 10.1111/jth.13209. Epub 2016 Feb 29. J Thromb Haemost. 2016. PMID: 26613657 Free PMC article.
-
Rho-associated protein kinase 1 (ROCK1) is increased in Alzheimer's disease and ROCK1 depletion reduces amyloid-β levels in brain.J Neurochem. 2016 Aug;138(4):525-31. doi: 10.1111/jnc.13688. Epub 2016 Jul 1. J Neurochem. 2016. PMID: 27246255 Free PMC article.
-
Alzheimer's disease.Subcell Biochem. 2012;65:329-52. doi: 10.1007/978-94-007-5416-4_14. Subcell Biochem. 2012. PMID: 23225010 Review.
-
Intracellular amyloid-β accumulation in calcium-binding protein-deficient neurons leads to amyloid-β plaque formation in animal model of Alzheimer's disease.J Alzheimers Dis. 2012;29(3):615-28. doi: 10.3233/JAD-2011-111778. J Alzheimers Dis. 2012. PMID: 22269161
-
Plaque formation and the intraneuronal accumulation of β-amyloid in Alzheimer's disease.Pathol Int. 2017 Apr;67(4):185-193. doi: 10.1111/pin.12520. Epub 2017 Mar 5. Pathol Int. 2017. PMID: 28261941 Review.
Cited by
-
Fibrin-targeting immunotherapy protects against neuroinflammation and neurodegeneration.Nat Immunol. 2018 Nov;19(11):1212-1223. doi: 10.1038/s41590-018-0232-x. Epub 2018 Oct 15. Nat Immunol. 2018. PMID: 30323343 Free PMC article.
-
Neprilysin inhibitors and risk of Alzheimer's disease: A future perspective.J Cell Mol Med. 2024 Jan;28(2):e17993. doi: 10.1111/jcmm.17993. Epub 2023 Oct 17. J Cell Mol Med. 2024. PMID: 37847125 Free PMC article. Review.
-
In vivo two-photon microscopy protocol for imaging microglial responses and spine elimination at sites of fibrinogen deposition in mouse brain.STAR Protoc. 2021 Jul 2;2(3):100638. doi: 10.1016/j.xpro.2021.100638. eCollection 2021 Sep 17. STAR Protoc. 2021. PMID: 34258598 Free PMC article.
-
Complement Activation in the Central Nervous System: A Biophysical Model for Immune Dysregulation in the Disease State.Front Mol Neurosci. 2021 Mar 4;14:620090. doi: 10.3389/fnmol.2021.620090. eCollection 2021. Front Mol Neurosci. 2021. PMID: 33746710 Free PMC article.
-
Increasing cerebral blood flow improves cognition into late stages in Alzheimer's disease mice.J Cereb Blood Flow Metab. 2020 Jul;40(7):1441-1452. doi: 10.1177/0271678X19873658. Epub 2019 Sep 7. J Cereb Blood Flow Metab. 2020. PMID: 31495298 Free PMC article.
References
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

