Catheter-directed thrombolysis of deep vein thrombosis: literature review and practice considerations
- PMID: 29399526
- PMCID: PMC5778526
- DOI: 10.21037/cdt.2017.09.15
Catheter-directed thrombolysis of deep vein thrombosis: literature review and practice considerations
Abstract
Deep vein thrombosis (DVT) is a major health problem worldwide. The risk of pulmonary embolism following DVT is well established, but the long-term vascular sequelae of DVT are often underappreciated, costly to manage, and can have extremely detrimental effects on quality of life. Treatment of DVT classically involves oral anticoagulation, which reduces the risk of pulmonary embolism but does not remove the clot. Anticoagulation therefore does little to prevent the venous damage and scarring that occurs following DVT, leaving the patient at risk for permanent venous insufficiency and development of post-thrombotic syndrome (PTS). Catheter-directed thrombolysis (CDT) is a minimally invasive endovascular treatment that is used as an adjunct to anticoagulation. CDT lowers the risk of PTS by reducing clot burden and protecting against valvular damage. A catheter is advanced directly to the site of thrombosis under fluoroscopy followed by a slow, prolonged infusion of a relatively low dose of thrombolytic agent. CDT restores venous patency faster than anticoagulation, which hastens the relief of acute symptoms. Adjunctive CDT modalities have become increasingly popular among interventional radiologists, allowing for additional mechanical thrombectomy or ultrasound-enhanced thrombolysis at the time of catheter placement. These pharmacomechanical CDT (PCDT) techniques have the potential to reduce treatment time and associated healthcare costs. Numerous observational and retrospective studies have consistently shown a benefit of CDT plus anticoagulation over anticoagulation alone for prevention of PTS. Patients with long life expectancy and acute thrombosis involving the iliac and proximal femoral veins (iliofemoral DVT) have the greatest benefit from CDT, which may decrease the risk of PTS and/or decrease the severity of PTS symptoms if they do occur. Randomized controlled trials remain limited but generally support the observational data. CDT also plays an important role in those with acute limb-threatening venous occlusion or severe symptoms from DVT. Although adverse outcomes are rare, a potential devastating outcome is intracranial bleeding. While the available literature suggests the risk of serious morbidity from bleeding is quite rare, the absolute risk of bleeding is not clear and will require outcomes data from randomized trials. Future studies should also examine the cost-effectiveness of CDT for PTS prevention, particularly with respect to quality-adjusted life years, and compare the effectiveness of available PCDT devices.
Keywords: Catheter; catheter-directed thrombolysis (CDT); deep vein thrombosis (DVT); post-thrombotic syndrome (PTS); thrombolysis.
Conflict of interest statement
Conflicts of Interest: The authors have no conflicts of interest to declare.
Figures

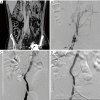
Similar articles
-
Thrombolytic strategies versus standard anticoagulation for acute deep vein thrombosis of the lower limb.Cochrane Database Syst Rev. 2021 Jan 19;1(1):CD002783. doi: 10.1002/14651858.CD002783.pub5. Cochrane Database Syst Rev. 2021. PMID: 33464575 Free PMC article.
-
Comparative outcomes of catheter-directed thrombolysis versus AngioJet pharmacomechanical catheter-directed thrombolysis for treatment of acute iliofemoral deep vein thrombosis.J Vasc Surg Venous Lymphat Disord. 2024 Jan;12(1):101669. doi: 10.1016/j.jvsv.2023.08.010. Epub 2023 Aug 23. J Vasc Surg Venous Lymphat Disord. 2024. PMID: 37625507 Free PMC article.
-
AngioJet Pharmacomechanical Thrombectomy and Catheter Directed Thrombolysis vs. Catheter Directed Thrombolysis Alone for the Treatment of Iliofemoral Deep Vein Thrombosis: A Single Centre Retrospective Cohort Study.Eur J Vasc Endovasc Surg. 2020 Oct;60(4):578-585. doi: 10.1016/j.ejvs.2020.05.006. Epub 2020 Jul 11. Eur J Vasc Endovasc Surg. 2020. PMID: 32665201
-
Evaluation of thrombolysis using tissue plasminogen activator in lower extremity deep venous thrombosis with concomitant femoral-popliteal venous segment involvement.J Vasc Surg Venous Lymphat Disord. 2017 Sep;5(5):613-620. doi: 10.1016/j.jvsv.2017.04.018. Epub 2017 Jun 21. J Vasc Surg Venous Lymphat Disord. 2017. PMID: 28818211
-
Endovascular Management of Acute Lower Limb Deep Vein Thrombosis: A Systematic Review and Meta-analysis.Ann Vasc Surg. 2019 Jul;58:363-370. doi: 10.1016/j.avsg.2018.12.067. Epub 2019 Feb 13. Ann Vasc Surg. 2019. PMID: 30769054
Cited by
-
Subclavian Effort Thrombosis: Pathophysiology, Diagnosis, and Management.Semin Intervent Radiol. 2022 Aug 31;39(3):304-311. doi: 10.1055/s-0042-1753481. eCollection 2022 Jun. Semin Intervent Radiol. 2022. PMID: 36062232 Free PMC article. Review.
-
Catheter-Directed Interventions for the Treatment of Lower Extremity Deep Vein Thrombosis.Life (Basel). 2022 Nov 27;12(12):1984. doi: 10.3390/life12121984. Life (Basel). 2022. PMID: 36556349 Free PMC article. Review.
-
Catheter-Directed Thrombolysis in Acute Iliofemoral Deep Vein Thrombosis with or without Stenting: A Case Series.J Tehran Heart Cent. 2018 Oct;13(4):186-190. J Tehran Heart Cent. 2018. PMID: 30972118 Free PMC article.
-
Massive Deep Venous Thrombosis in a Child with Necrotizing Pneumonia Due to Mycoplasma Pneumonia Infection.Infect Drug Resist. 2024 Nov 28;17:5299-5304. doi: 10.2147/IDR.S478213. eCollection 2024. Infect Drug Resist. 2024. PMID: 39624637 Free PMC article.
-
Deep venous thrombosis in an individual with statin-exposed anti-SRP myopathy: case report and review of literature.Thromb J. 2021 Nov 25;19(1):92. doi: 10.1186/s12959-021-00347-x. Thromb J. 2021. PMID: 34823539 Free PMC article.
References
-
- Office of the Surgeon G, National Heart L, Blood I. Publications and Reports of the Surgeon General. The Surgeon General's Call to Action to Prevent Deep Vein Thrombosis and Pulmonary Embolism. Rockville (MD): Office of the Surgeon General (US), 2008. - PubMed
Publication types
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
