Pediatric Craniopharyngiomas: A Primer for the Skull Base Surgeon
- PMID: 29404243
- PMCID: PMC5796826
- DOI: 10.1055/s-0037-1621738
Pediatric Craniopharyngiomas: A Primer for the Skull Base Surgeon
Abstract
Pediatric craniopharyngioma is a rare sellar-region epithelial tumor that, in spite of its typically benign pathology, has the potential to be clinically devastating, and presents a host of formidable management challenges for the skull base surgeon. Strategies in craniopharyngioma care have been the cause of considerable controversy, with respect to both philosophical and technical issues. Key questions remain unresolved, and include optimizing extent-of-resection goals; the ideal radiation modality and its role as an alternative, adjuvant, or salvage treatment; appropriate indications for expanded endoscopic endonasal surgery as an alternative to transcranial microsurgery; risks and benefits of skull base techniques in a pediatric population; benefits of and indications for intracavitary therapies; and the preferred management of common treatment complications. Correspondingly, we sought to review the preceding basic science and clinical outcomes literature on pediatric craniopharyngioma, so as to synthesize overarching recommendations, highlight major points of evidence and their conflicts, and assemble a general algorithm for skull base surgeons to use in tailoring treatment plans to the individual patient, tumor, and clinical course. In general terms, we concluded that safe, maximal, hypothalamic-sparing resection provides very good tumor control while minimizing severe deficits. Endoscopic endonasal, intraventricular, and transcranial skull base technique all have clear roles in the armamentarium, alongside standard craniotomies; these roles frequently overlap, and may be further optimized by using the approaches in adaptive combinations. Where aggressive subtotal resection is achieved, patients should be closely followed, with radiation initiated at the time of progression or recurrence-ideally via proton beam therapy, although three-dimensional conformal radiotherapy, intensity-modulated radiotherapy, and stereotactic radiosurgery are very appropriate in a range of circumstances, governed by access, patient age, disease architecture, and character of the recurrence. Perhaps most importantly, outcomes appear to be optimized by consolidated, multidisciplinary care. As such, we recommend treatment in highly experienced centers wherever possible, and emphasize the importance of longitudinal follow-up-particularly given the high incidence of recurrences and complications in a benign disease that effects a young patient population at risk of severe morbidity from hypothalamic or pituitary injury in childhood.
Keywords: hypothalamic injury; pediatric craniopharyngioma; pituitary injury; proton beam; radiotherapy; skull base; stereotactic radiosurgery; transsphenoidal surgery.
Conflict of interest statement
Figures
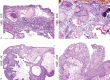
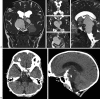
References
-
- Hoffman H J, Hendrick E B, Humphreys R P, Buncic J R, Armstrong D L, Jenkin R D. Management of craniopharyngioma in children. J Neurosurg. 1977;47(02):218–227. - PubMed
-
- Matson D D, Crigler J F., Jr Management of craniopharyngioma in childhood. J Neurosurg. 1969;30(04):377–390. - PubMed
-
- Shiminski-Maher T, Rosenberg M. Late effects associated with treatment of craniopharyngiomas in childhood. J Neurosci Nurs. 1990;22(04):220–226. - PubMed
-
- Burger P C, Scheithauer B W, Vogel F S. New York: Churchill Livingstone; 1991. Surgical Pathology of the Nervous System and Its Coverings.
-
- McLendon R E, Rosenblum M K, Bigner D D. London, UK: CRC Press; 2006. Russell & Rubinstein's Pathology of Tumors of the Nervous System 7ed.
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials

