Effects of liver cirrhosis on portal vein embolization prior to right hepatectomy in patients with primary liver cancer
- PMID: 29434832
- PMCID: PMC5777121
- DOI: 10.3892/ol.2017.7530
Effects of liver cirrhosis on portal vein embolization prior to right hepatectomy in patients with primary liver cancer
Abstract
Preoperative portal vein embolization (PVE) induces compensatory hyperplasia of the future liver remnants (FLR), thus increasing resectability in the non-cirrhotic patients with primary liver cancer (PLC). However, it is unclear if it is similar in patients with liver cirrhosis. Therefore, the present study investigated the PVE value prior to liver resection in patients with PLC, and the liver cirrhotic effects on the compensatory hypertrophy of FLRs following PVE. In the present study, 21 patients with PLC who successfully underwent hepatic resection subsequent to PVE, were retrospectively examined. The patients were divided into a non-cirrhosis group and a cirrhosis group according to the absence or presence of cirrhosis, respectively. The FLR volume between the two groups of patients was compared. There was a significant difference in the FLR volume for all patients prior to, and 4-6 weeks following, PVE (P<0.001). PVE induced significant compensatory hypertrophy in the FLRs whether in the non-cirrhosis group (P=0.002) or cirrhosis group (P<0.001). However, no significant difference was identified between the two groups with respect to FLR volume enlargement 4-6 weeks following PVE (P=0.373). In conclusion, PVE prior to hepatectomy may promote FLR compensatory hypertrophy and an increase in the resectability of PLC tumors. No significant effects of liver cirrhosis were identified on liver lobe hyperplasia following PVE.
Keywords: cirrhosis; embolization; hyperplasia; liver cancer; portal vein.
Figures
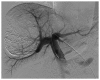
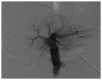
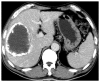
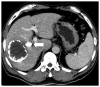
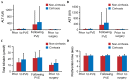
References
-
- Jarnagin WR, Gonen M, Fong Y, DeMatteo RP, Ben-Porat L, Little S, Corvera C, Weber S, Blumgart LH. Improvement in perioperative outcome after hepatic resection: Analysis of 1,803 consecutive cases over the past decade. Ann Surg. 2002;236:397–407. doi: 10.1097/00000658-200210000-00001. - DOI - PMC - PubMed
-
- Hwang S, Lee SG, Ko GY, Kim BS, Sung KB, Kim MH, Lee SK, Hong HN. Sequential preoperative ipsilateral hepatic vein embolization after portal vein embolization to induce further liver regeneration in patients with hepatobiliary malignancy. Ann Surg. 2009;249:608–616. doi: 10.1097/SLA.0b013e31819ecc5c. - DOI - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources
