Novel Approaches to the Diagnosis of Chronic Disorders of Consciousness: Detecting Peripersonal Space by Using Ultrasonics
- PMID: 29459847
- PMCID: PMC5807342
- DOI: 10.3389/fneur.2018.00047
Novel Approaches to the Diagnosis of Chronic Disorders of Consciousness: Detecting Peripersonal Space by Using Ultrasonics
Abstract
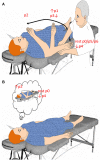
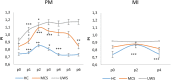
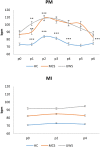
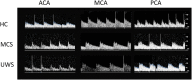
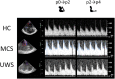
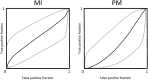
The assessment of behavioral responsiveness in patients suffering from chronic disorders of consciousness (DoC), including Unresponsive Wakefulness Syndrome (UWS) and Minimally Conscious State (MCS), is challenging. Even if a patient is unresponsive, he/she may be covertly aware in reason of a cognitive-motor dissociation, i.e., a preservation of cognitive functions despite a solely reflexive behavioral responsiveness. The approach of an external stimulus to the peripersonal space (PPS) modifies some biological measures (e.g., hand-blink reflex amplitude) to the purpose of defensive responses from threats. Such modulation depends on a top-down control of subcortical neural circuits, which can be explored through changes in cerebral blood flow velocity (CBFV), using functional transcranial Doppler (fTCD) and, thus, gaining useful, indirect information on brain connectivity. These data may be used for the DoC differential diagnosis. We evaluated the changes in CBFV by measuring the pulsatility index (PI) in 21 patients with DoC (10 patients with MCS and 11 with UWS) and 25 healthy controls (HC) during a passive movement and motor imagery (MI) task in which the hand of the subject approached and, then, moved away from the subject's face. In the passive movement task, the PI increased progressively in the HCs when the hand was moved toward the face and, then, it decreased when the hand was removed from the face. The PI increased when the hand was moved toward the face in patients with DoC, but then, it remained high when the hand was removed from the face and up to 30 s after the end of the movement in the patients with MCS (both MCS+ and MCS-) and 1 min in those with UWS, thus differentiating between patients with MCS and UWS. In the MI task, all the HCs, three out of four patients with MCS+, and one out of six patients with MCS- showed an increase-decrease PI change, whereas the remaining patients with MCS and all the patients with UWS showed no PI changes. Even though there is the possibility that our findings will not be replicated in all patients with DoC, we propose fTCD as a rapid and very easy tool to differentiate between patients with MCS and UWS, by identifying residual top-down modulation processes from higher-order cortical areas to sensory-motor integration networks related to the PPS, when using passive movement tasks.
Keywords: cerebral blood flow; chronic disorders of consciousness; motor imagery; peripersonal space; transcranial ultrasound.
Figures

References
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials
Miscellaneous

