Scleral surgery for the treatment of presbyopia: where are we today?
- PMID: 29497624
- PMCID: PMC5827891
- DOI: 10.1186/s40662-018-0098-x
Scleral surgery for the treatment of presbyopia: where are we today?
Abstract
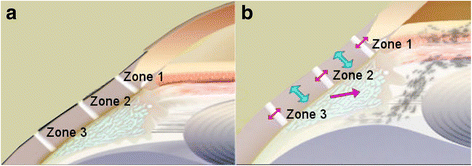
Presbyopia corrections traditionally have been approached with attempts to exchange power, either at the cornea or the lens planes, inducing multifocality, or altering asphericity to impact the optical system. Treatments that affect the visual axis, such as spectacle and contact lens correction, refractive surgeries, corneal onlays and inlays, and intraocular lenses are typically unable to restore true accommodation to the presbyopic eye. Their aim is instead to enhance 'pseudoaccommodation' by facilitating an extended depth-of-focus for which vision is sufficient. There is a true lack of technology that approaches presbyopia from a treatment based or therapy based solution, rather than a 'vision correction' solution that compromises other components of the optical system. Scleral surgical procedures seek to restore true accommodation combined with pseudoaccommodation and have several advantages over other more invasive options to treat presbyopia. While the theoretical justification of scleral surgical procedures remains controversial, there has nevertheless been increasing interest and evidence to support scleral surgical and therapeutic approaches to treat presbyopia. Enormous progress in scleral surgery techniques and understanding of the mechanisms of action have been achieved since the 1970s, and this remains an active area of research. In this article, we discuss the historic scleral surgical procedures, the two scleral procedures currently available, as well as an outlook of the future for the scleral surgical space for treating presbyopia.
Keywords: Accommodation; Presbyopia; Presbyopia treatment; Scleral surgery.
Conflict of interest statement
Data presented regarding LaserACE were obtained from IRB monitored and registered international clinical pilot studies (Trial Registration: NCT01491360), which followed the tenets of the Declaration of Helsinki.The LaserACE patients provided written consent for imaging and release of personal identifying information including medical record details.AMH reports personal fees and non-financial support from Ace Vision Group Inc. during the conduct of the study. In addition, Dr. Hipsley has a patent 7,871,404 issued to Ace Vision Group Inc., a patent 8,348,932 issued to Ace Vision Group, Inc., a patent 20,150,157,406 pending to Ace Vision Group, Inc., a patent 20,140,316,388 pending to Ace Vision Group, Inc., a patent 20,140,163,597 pending to Ace Vision Group, Inc., a patent 20,120,165,849 pending to Ace Vision Group, Inc., a patent 20,110,190,798 pending to Ace Vision Group, Inc., a patent 20,080,058,779 pending to Ace Vision Group, Inc., and a patent 20,070,016,175 pending to Ace Vision Group, Inc. BH reports personal fees from Ace Vision Group Inc. during the conduct of the study.
Figures

Similar articles
-
Presbyopia: Effectiveness of correction strategies.Prog Retin Eye Res. 2019 Jan;68:124-143. doi: 10.1016/j.preteyeres.2018.09.004. Epub 2018 Sep 19. Prog Retin Eye Res. 2019. PMID: 30244049 Review.
-
Developments in the correction of presbyopia II: surgical approaches.Ophthalmic Physiol Opt. 2014 Jul;34(4):397-426. doi: 10.1111/opo.12129. Epub 2014 Apr 10. Ophthalmic Physiol Opt. 2014. PMID: 24716827 Review.
-
A review of the surgical options for the correction of presbyopia.Br J Ophthalmol. 2016 Jan;100(1):62-70. doi: 10.1136/bjophthalmol-2015-306663. Epub 2015 Apr 23. Br J Ophthalmol. 2016. PMID: 25908836 Review.
-
Developments in the correction of presbyopia I: spectacle and contact lenses.Ophthalmic Physiol Opt. 2014 Jan;34(1):8-29. doi: 10.1111/opo.12091. Epub 2013 Nov 10. Ophthalmic Physiol Opt. 2014. PMID: 24205890 Review.
-
Refractive lens exchange for presbyopia.Cont Lens Anterior Eye. 2008 Jun;31(3):117-21. doi: 10.1016/j.clae.2008.03.005. Epub 2008 Apr 11. Cont Lens Anterior Eye. 2008. PMID: 18406656 Review.
Cited by
-
Review of Presbyopia Treatment with Corneal Inlays and New Developments.Clin Ophthalmol. 2022 Aug 24;16:2781-2795. doi: 10.2147/OPTH.S375577. eCollection 2022. Clin Ophthalmol. 2022. PMID: 36042913 Free PMC article. Review.
-
Laser refractive correction of presbyopia.Indian J Ophthalmol. 2024 Sep 1;72(9):1236-1243. doi: 10.4103/IJO.IJO_3074_23. Epub 2024 Aug 23. Indian J Ophthalmol. 2024. PMID: 39185826 Free PMC article. Review.
-
Surgical interventions for presbyopia.Cochrane Database Syst Rev. 2025 Apr 14;4(4):CD015711. doi: 10.1002/14651858.CD015711.pub2. Cochrane Database Syst Rev. 2025. PMID: 40226888
-
Scleral structure and biomechanics.Prog Retin Eye Res. 2020 Jan;74:100773. doi: 10.1016/j.preteyeres.2019.100773. Epub 2019 Aug 11. Prog Retin Eye Res. 2020. PMID: 31412277 Free PMC article. Review.
-
IRIS® Registry (Intelligent Research In Sight) Analysis of the Incidence of Monovision in Cataract Patients with Bilateral Monofocal Intraocular Lens Implantation.Clin Ophthalmol. 2023 Oct 19;17:3123-3129. doi: 10.2147/OPTH.S424195. eCollection 2023. Clin Ophthalmol. 2023. PMID: 37877114 Free PMC article.
References
-
- Millodot M. Dictionary of optometry and visual science. Philadelphia: Elsevier Health Sciences; 2014. p. 4.
-
- Richdale K, Sinnott LT, Bullimore MA, Wassenaar PA, Schmalbrock P, Kao CY, et al. Quantification of age-related and per diopter accommodative changes of the lens and ciliary muscle in the emmetropic human eye. Invest Ophthalmol Vis Sci. 2013;54:1095–1105. doi: 10.1167/iovs.12-10619. - DOI - PMC - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources
Molecular Biology Databases

