A NATURAL BODY WINDOW TO STUDY HUMAN PANCREATIC ISLET CELL FUNCTION AND SURVIVAL
- PMID: 29497630
- PMCID: PMC5828509
A NATURAL BODY WINDOW TO STUDY HUMAN PANCREATIC ISLET CELL FUNCTION AND SURVIVAL
Abstract
The World Health Organization projects diabetes prevalence worldwide to be at 4.4% in 2030 compared to 2.8% in the year 2000. These alarming predictions come amid vigorous efforts in diabetes research which have failed so far to deliver effective therapies. Our incomplete understanding of the pathogenesis of diabetes is likely to contribute to the "disconnect" between our research efforts and their translation into successful therapies. Technically, studying the pathophysiology of the pancreatic islets is hindered by the anatomical location of the pancreas, which is deeply embedded in the body, and by lack of experimental tools that enable comprehensive interrogation of the pancreatic islets with sufficient resolution in the context of the natural in vivo environment non-invasively and longitudinally. Emerging evidence also indicates that challenges in successful translation of findings in animal models to the human setting are complicated by some inherent structural and functional differences between the mouse and human islets. In this review, we briefly describe the advantages and shortcomings of existing intravital imaging approaches used to study the pancreatic islet biology in vivo, and we contrast such techniques with a recently established intravital approach using pancreatic islet transplantation into the anterior chamber of the eye. We also provide a summary of recent structure-function studies in the human pancreas to reveal distinctive features of human islets compared with mouse islets. We finally touch on a recently renewed discussion of the validity of animal models in studying human health and disease, and we highlight the potential utility of "humanized" animal models in studying different aspects of human islet biology and improving our understanding of diabetes.
Keywords: Diabetes; Human pancreatic islet cell; Islets of Langerhans; in vivo imaging.
Figures


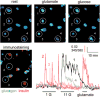
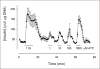
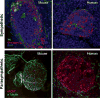
Similar articles
-
Islet inflammation in plain sight.Diabetes Obes Metab. 2013 Sep;15 Suppl 3(0 3):105-16. doi: 10.1111/dom.12160. Diabetes Obes Metab. 2013. PMID: 24003927 Free PMC article. Review.
-
Transplantation of Islets of Langerhans into the Anterior Chamber of the Eye for Longitudinal In Vivo Imaging.Methods Mol Biol. 2020;2128:149-157. doi: 10.1007/978-1-0716-0385-7_11. Methods Mol Biol. 2020. PMID: 32180192
-
Intraocular in vivo imaging of pancreatic islet cell physiology/pathology.Mol Metab. 2017 May 4;6(9):1002-1009. doi: 10.1016/j.molmet.2017.03.014. eCollection 2017 Sep. Mol Metab. 2017. PMID: 28951824 Free PMC article. Review.
-
In vivo imaging of type 1 diabetes immunopathology using eye-transplanted islets in NOD mice.Diabetologia. 2019 Jul;62(7):1237-1250. doi: 10.1007/s00125-019-4879-0. Epub 2019 May 14. Diabetologia. 2019. PMID: 31087105 Free PMC article.
-
Mouse models and human islet transplantation sites for intravital imaging.Front Endocrinol (Lausanne). 2022 Oct 5;13:992540. doi: 10.3389/fendo.2022.992540. eCollection 2022. Front Endocrinol (Lausanne). 2022. PMID: 36277698 Free PMC article. Review.
Cited by
-
Machine-learning-guided recognition of α and β cells from label-free infrared micrographs of living human islets of Langerhans.Sci Rep. 2024 Jun 20;14(1):14235. doi: 10.1038/s41598-024-65161-7. Sci Rep. 2024. PMID: 38902357 Free PMC article.
-
Pancreatic injury induces β-cell regeneration in axolotl.bioRxiv [Preprint]. 2025 Jan 23:2025.01.23.634564. doi: 10.1101/2025.01.23.634564. bioRxiv. 2025. Update in: Dev Dyn. 2025 Jul 18. doi: 10.1002/dvdy.70060. PMID: 39896453 Free PMC article. Updated. Preprint.
-
Comparative transcriptomics in human and mouse.Nat Rev Genet. 2017 Jul;18(7):425-440. doi: 10.1038/nrg.2017.19. Epub 2017 May 8. Nat Rev Genet. 2017. PMID: 28479595 Free PMC article. Review.
-
Clinical intraocular islet transplantation is not a number issue.CellR4 Repair Replace Regen Reprogram. 2016;4(4):e2120. Epub 2016 Jul 26. CellR4 Repair Replace Regen Reprogram. 2016. PMID: 29497631 Free PMC article.
-
Pancreatic Diseases: Genetics and Modeling Using Human Pluripotent Stem Cells.Int J Stem Cells. 2024 Aug 30;17(3):253-269. doi: 10.15283/ijsc24036. Epub 2024 Apr 26. Int J Stem Cells. 2024. PMID: 38664226 Free PMC article. Review.
References
-
- Prescher A, Mory C, Martin M, Fiedler M, Uhlmann D. Effect of FTY720 treatment on postischemic pancreatic microhemodynamics. Transplant Proc. 2010;42:3984–3985. - PubMed
-
- Toso C, Vallee JP, Morel P, Ris F, Demuylder-Mischler S, Lepetit-Coiffe M, Marangon N, Saudek F, James Shapiro AM, Bosco D, Berney T. Clinical magnetic resonance imaging of pancreatic islet grafts after iron nanoparticle labeling. Am J Transplant. 2008;8:701–706. - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
