Prognostic utility of baseline neutrophil-to-lymphocyte ratio in patients receiving immune checkpoint inhibitors: a review and meta-analysis
- PMID: 29503570
- PMCID: PMC5827677
- DOI: 10.2147/OTT.S153290
Prognostic utility of baseline neutrophil-to-lymphocyte ratio in patients receiving immune checkpoint inhibitors: a review and meta-analysis
Abstract
Introduction: Systemic inflammation is associated with prognosis in solid tumors. The neutrophil-to-lymphocyte ratio (NLR) is a marker for the general immune response to various stress stimuli. Studies have shown correlation of NLR to outcomes in immune checkpoint blockade, peripheral neutrophil count to intratumor neutrophil population, and NLR to intratumoral levels of myeloid-derived suppressor cells. Studies have shown elevated peripheral blood regulator T cells accompanied by elevated NLR are associated with poor outcomes further highlighting the importance of inflammation in the prognosis of cancer patients.
Methods: We performed a meta-analysis of published articles on the utility of baseline NLR in predicting outcomes in patients treated with immune checkpoint inhibitors (ICIs) using Review Manager, version 5.3. Seven studies on the prognostic utility of NLR in ICI treatment were included in this analysis. For outcomes of interest, the hazard ratios (HRs) were computed. Subgroup analyses were planned based on type of malignancy and type of immune checkpoint inhibitor.
Results/discussion: A high NLR resulted in worse overall survival (OS) (HR, 1.92; 95% CI, 1.29-2.87; p=0.001) and progression-free survival (PFS; HR, 1.66; 95% CI, 1.38-2.01; p<0.00001) across types of malignancies studied (melanoma, non-small-cell lung cancer, and genitourinary cancer). Subgroup analysis across different types of malignancies treated with ICI showed similar results for OS and PFS. The single study on genitourinary cancers also showed worse OS and PFS (OS: HR, 1.82; 95% CI, 1.29-2.87; p=0.001 and PFS: HR, 1.83; 95% CI, 0.97-3.44; p=0.06). A high NLR also showed worse OS and PFS across all ICIs (ipilimumab, nivolumab, and unspecified or pooled pembrolizumab and nivolumab; OS: HR, 1.92; 95% CI, 1.29-2.87; p=0.001 and PFS: HR, 1.66; 95% CI, 1.38-2.01; p<0.00001). Subgroup analysis by type of ICI showed similar results.
Conclusion: A high NLR is associated with poorer outcomes across studies. This shows that NLR has the potential as a readily available prognostic indicator for patients receiving ICI based on available studies. Studies utilizing more stringent design may serve to better determine the utility of this tool.
Keywords: biomarkers; immunotherapy; inflammation; neutrophil-to-lymphocyte ratio.
Conflict of interest statement
Disclosure The authors report no conflicts of interest in this work.
Figures

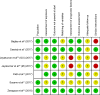




References
-
- Badoual C, Hans S, Fridman W, Brasnu D. Revisiting the prognostic value of regulatory T cells in patients with cancer. J Clin Oncol. 2009;27(19):e5–e6. - PubMed
-
- Bagley SJ, Kothari S, Aggarwal C, et al. Pretreatment neutrophil-to-lymphocyte ratio as a marker of outcomes in nivolumab-treated patients with advanced non-small-cell lung cancer. Lung Cancer. 2017;106:1–7. - PubMed
-
- Blank C, Enk A. Therapeutic use of anti-CTLA-4 antibodies. Int Immunol. 2014;27(1):3–10. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources

