Effect of a Low-Intensity PSA-Based Screening Intervention on Prostate Cancer Mortality: The CAP Randomized Clinical Trial
- PMID: 29509864
- PMCID: PMC5885905
- DOI: 10.1001/jama.2018.0154
Effect of a Low-Intensity PSA-Based Screening Intervention on Prostate Cancer Mortality: The CAP Randomized Clinical Trial
Abstract
Importance: Prostate cancer screening remains controversial because potential mortality or quality-of-life benefits may be outweighed by harms from overdetection and overtreatment.
Objective: To evaluate the effect of a single prostate-specific antigen (PSA) screening intervention and standardized diagnostic pathway on prostate cancer-specific mortality.
Design, setting, and participants: The Cluster Randomized Trial of PSA Testing for Prostate Cancer (CAP) included 419 582 men aged 50 to 69 years and was conducted at 573 primary care practices across the United Kingdom. Randomization and recruitment of the practices occurred between 2001 and 2009; patient follow-up ended on March 31, 2016.
Intervention: An invitation to attend a PSA testing clinic and receive a single PSA test vs standard (unscreened) practice.
Main outcomes and measures: Primary outcome: prostate cancer-specific mortality at a median follow-up of 10 years. Prespecified secondary outcomes: diagnostic cancer stage and Gleason grade (range, 2-10; higher scores indicate a poorer prognosis) of prostate cancers identified, all-cause mortality, and an instrumental variable analysis estimating the causal effect of attending the PSA screening clinic.
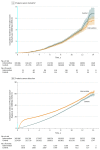
Results: Among 415 357 randomized men (mean [SD] age, 59.0 [5.6] years), 189 386 in the intervention group and 219 439 in the control group were included in the analysis (n = 408 825; 98%). In the intervention group, 75 707 (40%) attended the PSA testing clinic and 67 313 (36%) underwent PSA testing. Of 64 436 with a valid PSA test result, 6857 (11%) had a PSA level between 3 ng/mL and 19.9 ng/mL, of whom 5850 (85%) had a prostate biopsy. After a median follow-up of 10 years, 549 (0.30 per 1000 person-years) died of prostate cancer in the intervention group vs 647 (0.31 per 1000 person-years) in the control group (rate difference, -0.013 per 1000 person-years [95% CI, -0.047 to 0.022]; rate ratio [RR], 0.96 [95% CI, 0.85 to 1.08]; P = .50). The number diagnosed with prostate cancer was higher in the intervention group (n = 8054; 4.3%) than in the control group (n = 7853; 3.6%) (RR, 1.19 [95% CI, 1.14 to 1.25]; P < .001). More prostate cancer tumors with a Gleason grade of 6 or lower were identified in the intervention group (n = 3263/189 386 [1.7%]) than in the control group (n = 2440/219 439 [1.1%]) (difference per 1000 men, 6.11 [95% CI, 5.38 to 6.84]; P < .001). In the analysis of all-cause mortality, there were 25 459 deaths in the intervention group vs 28 306 deaths in the control group (RR, 0.99 [95% CI, 0.94 to 1.03]; P = .49). In the instrumental variable analysis for prostate cancer mortality, the adherence-adjusted causal RR was 0.93 (95% CI, 0.67 to 1.29; P = .66).
Conclusions and relevance: Among practices randomized to a single PSA screening intervention vs standard practice without screening, there was no significant difference in prostate cancer mortality after a median follow-up of 10 years but the detection of low-risk prostate cancer cases increased. Although longer-term follow-up is under way, the findings do not support single PSA testing for population-based screening.
Trial registration: ISRCTN Identifier: ISRCTN92187251.
Conflict of interest statement
Figures

Comment in
-
Screening for Prostate Cancer: Is the Third Trial the Charm?JAMA. 2018 Mar 6;319(9):868-869. doi: 10.1001/jama.2018.0153. JAMA. 2018. PMID: 29509848 No abstract available.
-
Prostate cancer: Solo PSA test does not lower mortality.Nat Rev Urol. 2018 May;15(5):262-263. doi: 10.1038/nrurol.2018.41. Epub 2018 Mar 27. Nat Rev Urol. 2018. PMID: 29581571 No abstract available.
-
[Effect of performing a single PSA screening : The CAP trial].Urologe A. 2018 Sep;57(9):1137-1138. doi: 10.1007/s00120-018-0678-3. Urologe A. 2018. PMID: 29796696 German. No abstract available.
-
Power of a Trial Investigating a Low-Intensity PSA-Based Screening Intervention.JAMA. 2018 Aug 14;320(6):600. doi: 10.1001/jama.2018.7327. JAMA. 2018. PMID: 30120468 No abstract available.
-
Re: Effect of a Low-Intensity PSA-Based Screening Intervention on Prostate Cancer Mortality: The CAP Randomized Clinical Trial.J Urol. 2018 Oct;200(4):699. doi: 10.1016/j.juro.2018.07.028. Epub 2018 Jul 17. J Urol. 2018. PMID: 30227582 No abstract available.
-
PSA Screening and Prostate Cancer Mortality.JAMA. 2024 Sep 10;332(10):842-843. doi: 10.1001/jama.2024.13803. JAMA. 2024. PMID: 39145957 No abstract available.
References
-
- Schröder FH, Hugosson J, Roobol MJ, et al. ; ERSPC Investigators . Screening and prostate-cancer mortality in a randomized European study. N Engl J Med. 2009;360(13):1320-1328. - PubMed
-
- Moyer VA; US Preventive Services Task Force . Screening for prostate cancer: US Preventive Services Task Force recommendation statement. Ann Intern Med. 2012;157(2):120-134. - PubMed
-
- Pinsky PF, Prorok PC, Kramer BS. Prostate cancer screening—a perspective on the current state of the evidence. N Engl J Med. 2017;376(13):1285-1289. - PubMed
-
- Hamdy FC, Donovan JL, Lane JA, et al. ; ProtecT Study Group . 10-year outcomes after monitoring, surgery, or radiotherapy for localized prostate cancer. N Engl J Med. 2016;375(15):1415-1424. - PubMed
Publication types
MeSH terms
Substances
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

