Chronic Hypopituitarism Associated with Increased Postconcussive Symptoms Is Prevalent after Blast-Induced Mild Traumatic Brain Injury
- PMID: 29515515
- PMCID: PMC5825904
- DOI: 10.3389/fneur.2018.00072
Chronic Hypopituitarism Associated with Increased Postconcussive Symptoms Is Prevalent after Blast-Induced Mild Traumatic Brain Injury
Abstract
The most frequent injury sustained by US service members deployed to Iraq or Afghanistan is mild traumatic brain injuries (mTBI), or concussion, by far most often caused by blast waves from improvised explosive devices or other explosive ordnance. TBI from all causes gives rise to chronic neuroendocrine disorders with an estimated prevalence of 25-50%. The current study expands upon our earlier finding that chronic pituitary gland dysfunction occurs with a similarly high frequency after blast-related concussions. We measured circulating hormone levels and accessed demographic and testing data from two groups of male veterans with hazardous duty experience in Iraq or Afghanistan. Veterans in the mTBI group had experienced one or more blast-related concussion. Members of the deployment control (DC) group encountered similar deployment conditions but had no history of blast-related mTBI. 12 of 39 (31%) of the mTBI participants and 3 of 20 (15%) veterans in the DC group screened positive for one or more neuroendocrine disorders. Positive screens for growth hormone deficiency occurred most often. Analysis of responses on self-report questionnaires revealed main effects of both mTBI and hypopituitarism on postconcussive and posttraumatic stress disorder (PTSD) symptoms. Symptoms associated with pituitary dysfunction overlap considerably with those of PTSD. They include cognitive deficiencies, mood and anxiety disorders, sleep problems, diminished quality of life, deleterious changes in metabolism and body composition, and increased cardiovascular mortality. When such symptoms are due to hypopituitarism, they may be alleviated by hormone replacement. These findings suggest consideration of routine post-deployment neuroendocrine screening of service members and veterans who have experienced blast-related mTBI and are reporting postconcussive symptoms.
Keywords: blast; concussion; growth hormone deficiency; military; pituitary; posttraumatic stress disorder; traumatic brain injury; veterans.
Figures
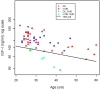
 ) and two of the DC group (
) and two of the DC group ( ) fell below the cutoff line.
) fell below the cutoff line.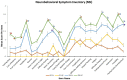
 No significant paired comparisons by Tukey HSD.
No significant paired comparisons by Tukey HSD.  Significant difference between mTBI-HP and DC-N by Tukey HSD.
Significant difference between mTBI-HP and DC-N by Tukey HSD.  Significant difference between mTBI-HP and DC-HP by Tukey HSD.
Significant difference between mTBI-HP and DC-HP by Tukey HSD.  Significant difference between mTBI-N and DC-HP by Tukey HSD.
Significant difference between mTBI-N and DC-HP by Tukey HSD.Similar articles
-
High prevalence of chronic pituitary and target-organ hormone abnormalities after blast-related mild traumatic brain injury.Front Neurol. 2012 Feb 7;3:11. doi: 10.3389/fneur.2012.00011. eCollection 2012. Front Neurol. 2012. PMID: 22347210 Free PMC article.
-
Independent and Synergistic Associations Between TBI Characteristics and PTSD Symptom Clusters on Cognitive Performance and Postconcussive Symptoms in Iraq and Afghanistan Veterans.J Neuropsychiatry Clin Neurosci. 2021 Spring;33(2):98-108. doi: 10.1176/appi.neuropsych.20050128. Epub 2021 Jan 14. J Neuropsychiatry Clin Neurosci. 2021. PMID: 33441014
-
Combat TBI: History, Epidemiology, and Injury Modes.In: Kobeissy FH, editor. Brain Neurotrauma: Molecular, Neuropsychological, and Rehabilitation Aspects. Boca Raton (FL): CRC Press/Taylor & Francis; 2015. Chapter 2. In: Kobeissy FH, editor. Brain Neurotrauma: Molecular, Neuropsychological, and Rehabilitation Aspects. Boca Raton (FL): CRC Press/Taylor & Francis; 2015. Chapter 2. PMID: 26269923 Free Books & Documents. Review.
-
Postconcussive symptoms after blast and nonblast-related mild traumatic brain injuries in Afghanistan and Iraq war veterans.J Int Neuropsychol Soc. 2010 Sep;16(5):856-66. doi: 10.1017/S1355617710000743. Epub 2010 Aug 4. J Int Neuropsychol Soc. 2010. PMID: 20682086
-
[Mild traumatic brain injury and postconcussive syndrome: a re-emergent questioning].Encephale. 2012 Sep;38(4):329-35. doi: 10.1016/j.encep.2011.07.003. Epub 2011 Aug 31. Encephale. 2012. PMID: 22980474 Review. French.
Cited by
-
Preliminary Evidence for a Window of Increased Vulnerability to Sustain a Concussion in Females: A Brief Report.Front Neurol. 2019 Jul 9;10:691. doi: 10.3389/fneur.2019.00691. eCollection 2019. Front Neurol. 2019. PMID: 31338057 Free PMC article.
-
Experience of a Pituitary Clinic for US Military Veterans With Traumatic Brain Injury.J Endocr Soc. 2021 Jan 25;5(4):bvab005. doi: 10.1210/jendso/bvab005. eCollection 2021 Apr 1. J Endocr Soc. 2021. PMID: 33655093 Free PMC article.
-
Traumatic brain injuries induced pituitary dysfunction: a call for algorithms.Endocr Connect. 2020 May;9(5):R112-R123. doi: 10.1530/EC-20-0117. Endocr Connect. 2020. PMID: 32412425 Free PMC article. Review.
-
Sex as a Biological Variable in Preclinical Modeling of Blast-Related Traumatic Brain Injury.Front Neurol. 2020 Sep 30;11:541050. doi: 10.3389/fneur.2020.541050. eCollection 2020. Front Neurol. 2020. PMID: 33101170 Free PMC article. Review.
-
Menstrual Cycle Patterns After Concussion in Adolescent Patients.J Pediatr. 2023 Nov;262:113349. doi: 10.1016/j.jpeds.2023.02.002. Epub 2023 Feb 15. J Pediatr. 2023. PMID: 36796579 Free PMC article.
References
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials

