Multimodality Imaging in Patients with Secondary Hypertension: With a Focus on Appropriate Imaging Approaches Depending on the Etiologies
- PMID: 29520185
- PMCID: PMC5840056
- DOI: 10.3348/kjr.2018.19.2.272
Multimodality Imaging in Patients with Secondary Hypertension: With a Focus on Appropriate Imaging Approaches Depending on the Etiologies
Abstract
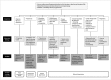
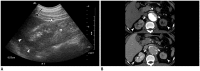
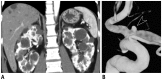
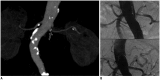
Although the causes of hypertension are usually unknown, about 10% of the cases occur secondary to specific etiologies, which are often treatable. Common categories of secondary hypertension include renal parenchymal disease, renovascular stenosis, vascular and endocrinologic disorders. For diseases involving the renal parenchyma and adrenal glands, ultrasonography (US), computed tomography (CT) or magnetic resonance (MR) imaging is recommended. For renovascular stenosis and vascular disorders, Doppler US, conventional or noninvasive (CT or MR) angiography is an appropriate modality. Nuclear imaging can be useful in the differential diagnosis of endocrine causes. Radiologists should understand the role of each imaging modality and its typical findings in various causes of secondary hypertension. This article focuses on appropriate imaging approaches in accordance with the categorized etiologies leading to hypertension.
Keywords: Computed tomography; Diagnostic imaging; Magnetic resonance imaging; Nuclear imaging; Secondary hypertension; Ultrasonography.
Figures
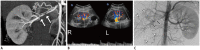
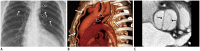
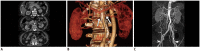
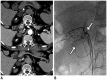
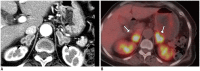
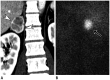
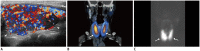
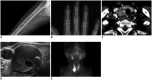
References
-
- Sinclair AM, Isles CG, Brown I, Cameron H, Murray GD, Robertson JW. Secondary hypertension in a blood pressure clinic. Arch Intern Med. 1987;147:1289–1293. - PubMed
-
- Anderson GH, Jr, Blakeman N, Streeten DH. The effect of age on prevalence of secondary forms of hypertension in 4429 consecutively referred patients. J Hypertens. 1994;12:609–615. - PubMed
-
- Rimoldi SF, Scherrer U, Messerli FH. Secondary arterial hypertension: when, who, and how to screen? Eur Heart J. 2014;35:1245–1254. - PubMed
-
- Shimamoto K, Ando K, Fujita T, Hasebe N, Higaki J, Horiuchi M, et al. The Japanese society of hypertension guidelines for the management of hypertension (JSH 2014) Hypertens Res. 2014;37:253–390. - PubMed
-
- Akpunonu BE, Mulrow PJ, Hoffman EA. Secondary hypertension: evaluation and treatment. Dis Mon. 1996;42:609–722. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

