The role of the general practitioner in multidisciplinary teams: a qualitative study in elderly care
- PMID: 29523092
- PMCID: PMC5845178
- DOI: 10.1186/s12875-018-0726-5
The role of the general practitioner in multidisciplinary teams: a qualitative study in elderly care
Abstract
Background: In the western world, a growing number of the older people live at home. In the Netherlands, GPs are expected to play a pivotal role in the organization of integrated care for this patient group. However, little is known about how GPs can play this role best. Our aim for this study was to unravel how GPs can play a successful role in elderly care, in particular in multidisciplinary teams, and to define key concepts for success.
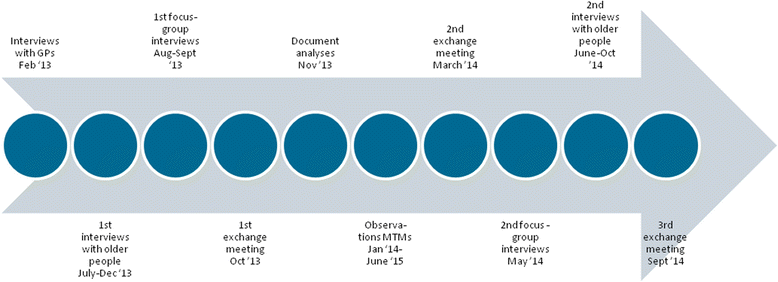
Methods: A mixed qualitative research model in four multidisciplinary teams for elderly care in the Netherlands was used. With these four teams, consisting of 46 health care and social service professionals, we carried out two rounds of focus-group interviews. Moreover, we performed semi-structured interviews with four GPs. We analysed data using a hybrid inductive/deductive thematic analysis.
Results: According to the health care and social service professionals in our study, the role of GPs in multidisciplinary teams for elderly care was characterized by the ability to 'see the bigger picture'. We identified five key activities that constitute a successful GP role: networking, facilitating, team building, integrating care elements, and showing leadership. Practice setting and phase of multidisciplinary team development influenced the way in which GPs fulfilled their roles. According to team members, GPs were the central professionals in care services for older people. The opinions of GPs about their own roles were diverse.
Conclusions: GPs took an important role in successful care settings for older people. Five key concepts seemed to be important for best practices in care for frail older people: networking (community), facilitating (organization), team building (professional), integrating care elements (patient), and leadership (personal). Team members from primary care and social services indicated that GPs had an indispensable role in such teams. It would be advantageous for GPs to be aware of this attributed role. Attention to leadership competencies and to the diversity of roles in multidisciplinary teams in GP training programmes seems useful. The challenge is to convince GPs to take a lead, also when they are not inclined to take this role in organizing multidisciplinary teams for older people.
Keywords: Focus groups; Frail older people; General practitioner; Integrated health care systems; Leadership; Multidisciplinary team meetings; Qualitative research.
Conflict of interest statement
Authors’ information
SG: MSc, researcher, Department of Primary and Community Care and policy advisor integrated care, Corporate Staff Strategy Development, Radboud University Medical Center, Nijmegen, NL. GM: PhD, researcher, manager healthy living, Department of Primary and Community Care, Radboud University Medical Center, Nijmegen and Community Health Service Gelderland-Zuid, Department of Healthy Living, Nijmegen, NL. AK: BSc, researcher, Department of Primary and Community Care, Radboud University Medical Center, Nijmegen, NL. RS, PhD, professor primary and community care. Lectureship of primary and community care, Han University of Applied Sciences, Nijmegen, NL. GF: PhD, researcher, team manager healthy community. Department of Primary and Community Care, Radboud University Medical Center, Nijmegen and Community Health Service Gelderland-Zuid, Department of Healthy Living, Nijmegen, NL. WA: MD, PhD, professor in general practice, Department of Primary and Community Care, Radboud University Medical Center, Nijmegen, NL. HS: MD, PhD, researcher and GP. Department of Primary and Community Care, Radboud University Medical Center, Nijmegen, NL.
Ethics approval and consent to participate
None required, according to the Arnhem and Nijmegen Research Ethics Committee (file number 2017-3516). According to the Committee, the respondents in our research were not subjected to any actions or behaviour that indicated that the research should be considered as a research under the Medical Research Act (WMO [Wet Medisch Onderzoek]). Therefore, it was not necessary for the CMO region Arnhem–Nijmegen or another recognized review committee to make a positive assessment. The participants signed an informed consent form to be included in this study.
Consent for publication
All participants gave written consent for the use of anonymized quotations from the focus-group discussions in presentations and publications arising from the research.
Competing interests
The authors declare that they have no competing interests.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Figures
Similar articles
-
Collaboration in teams with nurse practitioners and general practitioners during out-of-hours and implications for patient care; a qualitative study.BMC Health Serv Res. 2017 Aug 23;17(1):589. doi: 10.1186/s12913-017-2548-x. BMC Health Serv Res. 2017. PMID: 28830410 Free PMC article.
-
Caring for frail older people in the last phase of life - the general practitioners' view.BMC Palliat Care. 2016 Jun 2;15:52. doi: 10.1186/s12904-016-0124-5. BMC Palliat Care. 2016. PMID: 27255464 Free PMC article.
-
Skill mix change between general practitioners, nurse practitioners, physician assistants and nurses in primary healthcare for older people: a qualitative study.BMC Fam Pract. 2018 May 2;19(1):51. doi: 10.1186/s12875-018-0746-1. BMC Fam Pract. 2018. PMID: 29720099 Free PMC article.
-
[Charisma and leadership: new challenges for psychiatry].Encephale. 2013 Dec;39(6):445-51. doi: 10.1016/j.encep.2012.10.006. Epub 2012 Dec 13. Encephale. 2013. PMID: 23246329 Review. French.
-
Community-based rehabilitation services implemented by multidisciplinary teams among adults with stroke: a scoping review with a focus on Chinese experience.BMC Public Health. 2024 Mar 7;24(1):740. doi: 10.1186/s12889-024-18218-1. BMC Public Health. 2024. PMID: 38454384 Free PMC article.
Cited by
-
'Some of my patients only come to renew their prescriptions. They are not interested in any additional advice or support'. Physicians' perceptions on their roles in cardiovascular diseases risk reduction and management in Fiji.Prim Health Care Res Dev. 2023 Feb 8;24:e11. doi: 10.1017/S1463423622000779. Prim Health Care Res Dev. 2023. PMID: 36752134 Free PMC article.
-
Adults with intellectual disabilities and mental health disorders in primary care: a scoping review.Br J Gen Pract. 2022 Feb 24;72(716):e168-e178. doi: 10.3399/BJGP.2021.0164. Print 2022 Mar. Br J Gen Pract. 2022. PMID: 34903519 Free PMC article.
-
Clinical leadership and integrated primary care: A systematic literature review.Eur J Gen Pract. 2019 Jan;25(1):7-18. doi: 10.1080/13814788.2018.1515907. Epub 2018 Nov 26. Eur J Gen Pract. 2019. PMID: 30474447 Free PMC article.
-
How to promote changes in primary care? The Florentine experience of the House of Community.Front Public Health. 2023 Sep 5;11:1216814. doi: 10.3389/fpubh.2023.1216814. eCollection 2023. Front Public Health. 2023. PMID: 37732087 Free PMC article.
-
Differences in the healthcare needs of older adults attending primary health centers in urban and rural areas of Taiwan.BMC Prim Care. 2023 Oct 19;24(1):213. doi: 10.1186/s12875-023-02174-7. BMC Prim Care. 2023. PMID: 37858077 Free PMC article.
References
-
- Boeckxstaens P, De Graaf P. Primary care and care for older persons: position paper of the European forum for primary care. Qual Prim Care. 2011;19(6):369–389. - PubMed
-
- OECD . OECD insights. Paris: OECD; 2015. Ageing: debate the issues.
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources