Post-Exercise Oxygen Uptake Recovery Delay: A Novel Index of Impaired Cardiac Reserve Capacity in Heart Failure
- PMID: 29525330
- PMCID: PMC5880321
- DOI: 10.1016/j.jchf.2018.01.007
Post-Exercise Oxygen Uptake Recovery Delay: A Novel Index of Impaired Cardiac Reserve Capacity in Heart Failure
Abstract
Objectives: This study sought to characterize the functional and prognostic significance of oxygen uptake (VO2) kinetics following peak exercise in individuals with heart failure (HF).
Background: It is unknown to what extent patterns of VO2 recovery following exercise reflect circulatory response during exercise in HF with preserved ejection fraction (HFpEF) and HF with reduced ejection fraction (HFrEF).
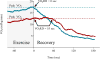
Methods: We investigated patients (30 HFpEF, 20 HFrEF, and 22 control subjects) who underwent cardiopulmonary exercise testing with invasive hemodynamic monitoring and a second distinct HF cohort (n = 106) who underwent noninvasive cardiopulmonary exercise testing with assessment of long-term outcomes. Fick cardiac output (CO) and cardiac filling pressures were measured at rest and throughout exercise in the initial cohort. A novel metric, VO2 recovery delay (VO2RD), defined as time until post-exercise VO2 falls permanently below peak VO2, was measured to characterize VO2 recovery kinetics.
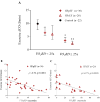
Results: VO2RD in patients with HFpEF (median 25 s [interquartile range (IQR): 9 to 39 s]) and HFrEF (28 s [IQR: 2 to 52 s]) was in excess of control subjects (5 s [IQR: 0 to 7 s]; p < 0.0001 and p = 0.003, respectively). VO2RD was inversely related to cardiac output augmentation during exercise in HFpEF (ρ = -0.70) and HFrEF (ρ = -0.73, both p < 0.001). In the second cohort, VO2RD predicted transplant-free survival in univariate and multivariable Cox regression analysis (Cox hazard ratios: 1.49 and 1.37 per 10-s increase in VO2RD, respectively; both p < 0.005).
Conclusions: Post-exercise VO2RD is an easily recognizable, noninvasively derived pattern that signals impaired cardiac output augmentation during exercise and predicts outcomes in HF. The presence and duration of VO2RD may complement established exercise measurements for assessment of cardiac reserve capacity.
Keywords: cardiopulmonary exercise testing; exercise hemodynamics; heart failure; recovery kinetics.
Copyright © 2018 American College of Cardiology Foundation. Published by Elsevier Inc. All rights reserved.
Figures



Comment in
-
"Recovering" the Recognition for VO2 Kinetics During Exercise Recovery in Heart Failure: A Good Practice in Need of More Exercise.JACC Heart Fail. 2018 Apr;6(4):340-342. doi: 10.1016/j.jchf.2018.01.020. Epub 2018 Mar 7. JACC Heart Fail. 2018. PMID: 29525331 No abstract available.
References
-
- Balady GJ, Arena R, Sietsema K, et al. Clinician’s Guide to cardiopulmonary exercise testing in adults: a scientific statement from the American Heart Association. Circulation. 2010;122:191–225. - PubMed
-
- O’Neill JO, Young JB, Pothier CE, Lauer MS. Peak oxygen consumption as a predictor of death in patients with heart failure receiving beta-blockers. Circulation. 2005;111:2313–8. - PubMed
-
- Mancini DM, Eisen H, Kussmaul W, Mull R, Edmunds LH, Jr, Wilson JR. Value of peak exercise oxygen consumption for optimal timing of cardiac transplantation in ambulatory patients with heart failure. Circulation. 1991;83:778–86. - PubMed
-
- Guazzi M, Dickstein K, Vicenzi M, Arena R. Six-minute walk test and cardiopulmonary exercise testing in patients with chronic heart failure: a comparative analysis on clinical and prognostic insights. Circulation Heart failure. 2009;2:549–55. - PubMed
-
- Malhotra R, Bakken K, D’Elia E, Lewis GD. Cardiopulmonary Exercise Testing in Heart Failure. JACC Heart failure. 2016;4:607–16. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

