Canagliflozin and Heart Failure in Type 2 Diabetes Mellitus: Results From the CANVAS Program
- PMID: 29526832
- PMCID: PMC6075881
- DOI: 10.1161/CIRCULATIONAHA.118.034222
Canagliflozin and Heart Failure in Type 2 Diabetes Mellitus: Results From the CANVAS Program
Abstract
Background: Canagliflozin is a sodium glucose cotransporter 2 inhibitor that reduces the risk of cardiovascular events. We report the effects on heart failure (HF) and cardiovascular death overall, in those with and without a baseline history of HF, and in other participant subgroups.
Methods: The CANVAS Program (Canagliflozin Cardiovascular Assessment Study) enrolled 10 142 participants with type 2 diabetes mellitus and high cardiovascular risk. Participants were randomly assigned to canagliflozin or placebo and followed for a mean of 188 weeks. The primary end point for these analyses was adjudicated cardiovascular death or hospitalized HF.
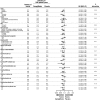
Results: Participants with a history of HF at baseline (14.4%) were more frequently women, white, and hypertensive and had a history of prior cardiovascular disease (all P<0.001). Greater proportions of these patients were using therapies such as blockers of the renin angiotensin aldosterone system, diuretics, and β-blockers at baseline (all P<0.001). Overall, cardiovascular death or hospitalized HF was reduced in those treated with canagliflozin compared with placebo (16.3 versus 20.8 per 1000 patient-years; hazard ratio [HR], 0.78; 95% confidence interval [CI], 0.67-0.91), as was fatal or hospitalized HF (HR, 0.70; 95% CI, 0.55-0.89) and hospitalized HF alone (HR, 0.67; 95% CI, 0.52-0.87). The benefit on cardiovascular death or hospitalized HF may be greater in patients with a prior history of HF (HR, 0.61; 95% CI, 0.46-0.80) compared with those without HF at baseline (HR, 0.87; 95% CI, 0.72-1.06; P interaction =0.021). The effects of canagliflozin compared with placebo on other cardiovascular outcomes and key safety outcomes were similar in participants with and without HF at baseline (all interaction P values >0.130), except for a possibly reduced absolute rate of events attributable to osmotic diuresis among those with a prior history of HF ( P=0.03).
Conclusions: In patients with type 2 diabetes mellitus and an elevated risk of cardiovascular disease, canagliflozin reduced the risk of cardiovascular death or hospitalized HF across a broad range of different patient subgroups. Benefits may be greater in those with a history of HF at baseline.
Clinical trial registration: URL: https://www.clinicaltrials.gov . Unique identifiers: NCT01032629 and NCT01989754.
Keywords: SGLT2 inhibitor; canagliflozin; heart failure; randomized trial; type 2 diabetes mellitus.
Figures



Comment in
-
Cardioprotection: SGLT2 blockers in T2DM.Nat Rev Cardiol. 2018 May;15(5):255. doi: 10.1038/nrcardio.2018.35. Epub 2018 Mar 29. Nat Rev Cardiol. 2018. PMID: 29593287 No abstract available.
-
Letter by Koh Regarding Article, "Canagliflozin and Heart Failure in Type 2 Diabetes Mellitus: Results From the CANVAS Program (Canagliflozin Cardiovascular Assessment Study)".Circulation. 2019 Jan 15;139(3):416-417. doi: 10.1161/CIRCULATIONAHA.118.037209. Circulation. 2019. PMID: 30640544 No abstract available.
-
Response by Figtree et al to Letter Regarding Article, "Canagliflozin and Heart Failure in Type 2 Diabetes Mellitus: Results From the CANVAS Program (Canagliflozin Cardiovascular Assessment Study)".Circulation. 2019 Jan 15;139(3):418-419. doi: 10.1161/CIRCULATIONAHA.118.038477. Circulation. 2019. PMID: 30640545 No abstract available.
References
-
- Liyanage T, Ninomiya T, Jha V, Neal B, Patrice HM, Okpechi I, Zhao MH, Lv J, Garg AX, Knight J, Rodgers A, Gallagher M, Kotwal S, Cass A, Perkovic V. Worldwide access to treatment for end-stage kidney disease: a systematic review. Lancet. 2015;385:1975–1982. doi: 10.1016/S0140-6736(14)61601-9. - PubMed
-
- Whiting DR, Guariguata L, Weil C, Shaw J. IDF diabetes atlas: global estimates of the prevalence of diabetes for 2011 and 2030. Diabetes Res Clin Pract. 2011;94:311–321. doi: 10.1161/CIRCULATIONAHA.117.030209. - PubMed
-
- Shah AD, Langenberg C, Rapsomaniki E, Denaxas S, Pujades-Rodriguez M, Gale CP, Deanfield J, Smeeth L, Timmis A, Hemingway H. Type 2 diabetes and incidence of cardiovascular diseases: a cohort study in 1·9 million people. Lancet Diabetes Endocrinol. 2015;3:105–113. doi: 10.1016/S2213-8587(14)70219-0. - PMC - PubMed
-
- Lehrke M, Marx N. Diabetes mellitus and heart failure. Am J Cardiol. 2017;120(1S):S37–S47. doi: 10.1016/j.amjcard.2017.05.014. - PubMed
-
- Nielsen R, Jorsal A, Iversen P, Tolbod L, Bouchelouche K, Sørensen J, Harms HJ, Flyvbjerg A, Bøtker HE, Wiggers H. Heart failure patients with prediabetes and newly diagnosed diabetes display abnormalities in myocardial metabolism. J Nucl Cardiol. 2018;25:169–176. doi: 10.1007/s12350-016-0622-0. - PubMed
Publication types
MeSH terms
Substances
Associated data
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

