Phenotyping Cardiac Arrest: Bench and Bedside Characterization of Brain and Heart Injury Based on Etiology
- PMID: 29533310
- PMCID: PMC5953808
- DOI: 10.1097/CCM.0000000000003070
Phenotyping Cardiac Arrest: Bench and Bedside Characterization of Brain and Heart Injury Based on Etiology
Abstract
Objectives: Cardiac arrest etiology may be an important source of between-patient heterogeneity, but the impact of etiology on organ injury is unknown. We tested the hypothesis that asphyxial cardiac arrest results in greater neurologic injury than cardiac etiology cardiac arrest (ventricular fibrillation cardiac arrest), whereas ventricular fibrillation cardiac arrest results in greater cardiovascular dysfunction after return of spontaneous circulation.
Design: Prospective observational human and randomized animal study.
Setting: University laboratory and ICUs.
Patients: Five-hundred forty-three cardiac arrest patients admitted to ICU.
Subjects: Seventy-five male Sprague-Dawley rats.
Interventions: We examined neurologic and cardiovascular injury in Isoflurane-anesthetized rat cardiac arrest models matched by ischemic time. Hemodynamic and neurologic outcomes were assessed after 5 minutes no flow asphyxial cardiac arrest or ventricular fibrillation cardiac arrest. Comparison was made to injury patterns observed after human asphyxial cardiac arrest or ventricular fibrillation cardiac arrest.
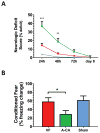
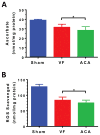
Measurements and main results: In rats, cardiac output (20 ± 10 vs 45 ± 9 mL/min) and pH were lower and lactate higher (9.5 ± 1.0 vs 6.4 ± 1.3 mmol/L) after return of spontaneous circulation from ventricular fibrillation cardiac arrest versus asphyxial cardiac arrest (all p < 0.01). Asphyxial cardiac arrest resulted in greater early neurologic deficits, 7-day neuronal loss, and reduced freezing time (memory) after conditioned fear (all p < 0.05). Brain antioxidant reserves were more depleted following asphyxial cardiac arrest. In adjusted analyses, human ventricular fibrillation cardiac arrest was associated with greater cardiovascular injury based on peak troponin (7.8 ng/mL [0.8-57 ng/mL] vs 0.3 ng/mL [0.0-1.5 ng/mL]) and ejection fraction by echocardiography (20% vs 55%; all p < 0.0001), whereas asphyxial cardiac arrest was associated with worse early neurologic injury and poor functional outcome at hospital discharge (n = 46 [18%] vs 102 [44%]; p < 0.0001). Most ventricular fibrillation cardiac arrest deaths (54%) were the result of cardiovascular instability, whereas most asphyxial cardiac arrest deaths (75%) resulted from neurologic injury (p < 0.0001).
Conclusions: In transcending rat and human studies, we find a consistent phenotype of heart and brain injury after cardiac arrest based on etiology: ventricular fibrillation cardiac arrest produces worse cardiovascular dysfunction, whereas asphyxial cardiac arrest produces worsened neurologic injury associated with greater oxidative stress.
Figures

References
-
- Mozaffarian D, Benjamin EJ, Go AS, et al. Heart disease and stroke statistics--2015 update: a report from the American Heart Association. Circulation. 2015;131(4):e29–322. - PubMed
-
- Link MS, Berkow LC, Kudenchuk PJ, et al. Part 7: Adult Advanced Cardiovascular Life Support: 2015 American Heart Association Guidelines Update for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation. 2015;132(18 suppl 2):S444–S464. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

