Predictors and Prognostic Value of Worsening Renal Function During Admission in HFpEF Versus HFrEF: Data From the KorAHF (Korean Acute Heart Failure) Registry
- PMID: 29535141
- PMCID: PMC5907555
- DOI: 10.1161/JAHA.117.007910
Predictors and Prognostic Value of Worsening Renal Function During Admission in HFpEF Versus HFrEF: Data From the KorAHF (Korean Acute Heart Failure) Registry
Abstract
Background: Worsening renal function (WRF) is associated with adverse outcomes in patients with heart failure. We investigated the predictors and prognostic value of WRF during admission, in patients with preserved ejection fraction (HFpEF) versus those with reduced ejection fraction (HFrEF).
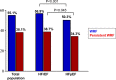
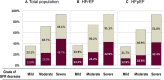
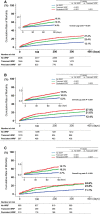
Methods and results: A total of 5625 patients were enrolled in the KorAHF (Korean Acute Heart Failure) registry. WRF was defined as an absolute increase in creatinine of ≥0.3 mg/dL. Transient WRF was defined as recovery of creatinine at discharge, whereas persistent WRF was indicated by a nonrecovered creatinine level. HFpEF and HFrEF were defined as a left ventricle ejection fraction ≥50% and ≤40%, respectively. Among the total population, WRF occurred in 3101 patients (55.1%). By heart failure subgroup, WRF occurred more frequently in HFrEF (57.0% versus 51.3%; P<0.001 in HFrEF and HFpEF). Prevalence of WRF increased as creatinine clearance decreased in both heart failure subgroups. Among various predictors of WRF, chronic renal failure was the strongest predictor. WRF was an independent predictor of adverse in-hospital outcomes (HFrEF: odds ratio; 2.75; 95% confidence interval, 1.50-5.02; P=0.001; HFpEF: odds ratio, 9.48; 95% confidence interval, 1.19-75.89; P=0.034) and 1-year mortality (HFrEF: hazard ratio, 1.41; 95% confidence interval, 1.12-1.78; P=0.004 versus HFpEF: hazard ratio, 1.72; 95% confidence interval, 1.23-2.42; P=0.002). Transient WRF was a risk factor for 1-year mortality, whereas persistent WRF had no additive risk compared to transient WRF.
Conclusions: In patients with acute heart failure patients, WRF is an independent predictor of adverse in-hospital and follow-up outcomes in both HFrEF and HFpEF, though with a different effect size.
Clinical trial registration: URL: https://www.clinicaltrials.gov. Unique identifier: NCT01389843.
Keywords: heart failure; heart failure with preserved ejection fraction; heart failure with reduced ejection fraction; renal function.
© 2018 The Authors. Published on behalf of the American Heart Association, Inc., by Wiley.
Figures
Similar articles
-
Worsening of renal function during 1 year after hospital discharge is a strong and independent predictor of all-cause mortality in acute decompensated heart failure.J Am Heart Assoc. 2014 Nov 4;3(6):e001174. doi: 10.1161/JAHA.114.001174. J Am Heart Assoc. 2014. PMID: 25370599 Free PMC article.
-
Short and long-term prognostic value of hyponatremia in heart failure with preserved ejection fraction versus reduced ejection fraction: An analysis of the Korean Acute Heart Failure registry.Int J Cardiol. 2017 Dec 1;248:239-245. doi: 10.1016/j.ijcard.2017.08.004. Epub 2017 Aug 5. Int J Cardiol. 2017. PMID: 28821416
-
Renin-Angiotensin System Inhibition, Worsening Renal Function, and Outcome in Heart Failure Patients With Reduced and Preserved Ejection Fraction: A Meta-Analysis of Published Study Data.Circ Heart Fail. 2017 Feb;10(2):e003588. doi: 10.1161/CIRCHEARTFAILURE.116.003588. Circ Heart Fail. 2017. PMID: 28209765 Review.
-
Worsening renal function and outcome in heart failure patients with reduced and preserved ejection fraction and the impact of angiotensin receptor blocker treatment: data from the CHARM-study programme.Eur J Heart Fail. 2016 Dec;18(12):1508-1517. doi: 10.1002/ejhf.609. Epub 2016 Jul 18. Eur J Heart Fail. 2016. PMID: 27427441
-
Heart Failure with Reduced Ejection Fraction (HFrEF) and Preserved Ejection Fraction (HFpEF): The Diagnostic Value of Circulating MicroRNAs.Cells. 2019 Dec 16;8(12):1651. doi: 10.3390/cells8121651. Cells. 2019. PMID: 31888288 Free PMC article. Review.
Cited by
-
J-shaped relationship between serum creatinine and mortality in Korean patients with acute heart failure.Clin Res Cardiol. 2024 Aug 27. doi: 10.1007/s00392-024-02469-4. Online ahead of print. Clin Res Cardiol. 2024. PMID: 39190184
-
Acute Decompensated Heart Failure and the Kidney: Physiological, Histological and Transcriptomic Responses to Development and Recovery.J Am Heart Assoc. 2021 Sep 21;10(18):e021312. doi: 10.1161/JAHA.121.021312. Epub 2021 Sep 17. J Am Heart Assoc. 2021. PMID: 34533033 Free PMC article.
-
Insulin-like growth factor-1 (IGF-1) as predictor of cardiovascular mortality in heart failure patients: data from the T.O.S.CA. registry.Intern Emerg Med. 2022 Sep;17(6):1651-1660. doi: 10.1007/s11739-022-02980-4. Epub 2022 Apr 21. Intern Emerg Med. 2022. PMID: 35445917 Free PMC article.
-
Biomarkers in Heart Failure with Preserved Ejection Fraction: A Perpetually Evolving Frontier.J Clin Med. 2024 Aug 7;13(16):4627. doi: 10.3390/jcm13164627. J Clin Med. 2024. PMID: 39200768 Free PMC article. Review.
-
The Prognostic Impact of Estimated Creatinine Clearance by Bioelectrical Impedance Analysis in Heart Failure: Comparison of Different eGFR Formulas.Biomedicines. 2021 Sep 24;9(10):1307. doi: 10.3390/biomedicines9101307. Biomedicines. 2021. PMID: 34680423 Free PMC article.
References
-
- de Silva R, Nikitin NP, Witte KK, Rigby AS, Goode K, Bhandari S, Clark AL, Cleland JG. Incidence of renal dysfunction over 6 months in patients with chronic heart failure due to left ventricular systolic dysfunction: contributing factors and relationship to prognosis. Eur Heart J. 2006;27:569–581. - PubMed
-
- Damman K, Navis G, Voors AA, Asselbergs FW, Smilde TD, Cleland JG, van Veldhuisen DJ, Hillege HL. Worsening renal function and prognosis in heart failure: systematic review and meta‐analysis. J Card Fail. 2007;13:599–608. - PubMed
-
- Damman K, Valente MA, Voors AA, O'Connor CM, van Veldhuisen DJ, Hillege HL. Renal impairment, worsening renal function, and outcome in patients with heart failure: an updated meta‐analysis. Eur Heart J. 2014;35:455–469. - PubMed
-
- Bock JS, Gottlieb SS. Cardiorenal syndrome: new perspectives. Circulation. 2010;121:2592–2600. - PubMed
Publication types
MeSH terms
Substances
Associated data
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

