Development and Validation of a Novel Pediatric Appendicitis Risk Calculator (pARC)
- PMID: 29535251
- PMCID: PMC5869337
- DOI: 10.1542/peds.2017-2699
Development and Validation of a Novel Pediatric Appendicitis Risk Calculator (pARC)
Abstract
Objectives: We sought to develop and validate a clinical calculator that can be used to quantify risk for appendicitis on a continuous scale for patients with acute abdominal pain.
Methods: The pediatric appendicitis risk calculator (pARC) was developed and validated through secondary analyses of 3 distinct cohorts. The derivation sample included visits to 9 pediatric emergency departments between March 2009 and April 2010. The validation sample included visits to a single pediatric emergency department from 2003 to 2004 and 2013 to 2015. Variables evaluated were as follows: age, sex, temperature, nausea and/or vomiting, pain duration, pain location, pain with walking, pain migration, guarding, white blood cell count, and absolute neutrophil count. We used stepwise regression to develop and select the best model. Test performance of the pARC was compared with the Pediatric Appendicitis Score (PAS).
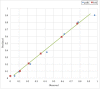
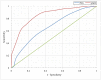
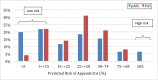
Results: The derivation sample included 2423 children, 40% of whom had appendicitis. The validation sample included 1426 children, 35% of whom had appendicitis. The final pARC model included the following variables: sex, age, duration of pain, guarding, pain migration, maximal tenderness in the right-lower quadrant, and absolute neutrophil count. In the validation sample, the pARC exhibited near perfect calibration and a high degree of discrimination (area under the curve: 0.85; 95% confidence interval: 0.83 to 0.87) and outperformed the PAS (area under the curve: 0.77; 95% confidence interval: 0.75 to 0.80). By using the pARC, almost half of patients in the validation cohort could be accurately classified as at <15% risk or ≥85% risk for appendicitis, whereas only 23% would be identified as having a comparable PAS of <3 or >8.
Conclusions: In our validation cohort of patients with acute abdominal pain, the pARC accurately quantified risk for appendicitis.
Copyright © 2018 by the American Academy of Pediatrics.
Conflict of interest statement
POTENTIAL CONFLICT OF INTEREST: The authors have indicated they have no potential conflicts of interest to disclose. The funding agencies took no part in data analysis, interpretation, or manuscript preparation. No person received any honorarium or other payment to produce this manuscript. This article was written by Dr Anupam Kharbanda, and all authors take full responsibility for the integrity of the data and the accuracy of data analysis.
Figures
Similar articles
-
Validation of the Pediatric Appendicitis Risk Calculator (pARC) in a Community Emergency Department Setting.Ann Emerg Med. 2019 Oct;74(4):471-480. doi: 10.1016/j.annemergmed.2019.04.023. Epub 2019 Jun 19. Ann Emerg Med. 2019. PMID: 31229394 Free PMC article.
-
Prospective validation of the pediatric appendicitis score.J Pediatr. 2008 Aug;153(2):278-82. doi: 10.1016/j.jpeds.2008.01.033. Epub 2008 Mar 19. J Pediatr. 2008. PMID: 18534219
-
A new clinical score to identify children at low risk for appendicitis.Am J Emerg Med. 2020 Mar;38(3):554-561. doi: 10.1016/j.ajem.2019.05.050. Epub 2019 May 28. Am J Emerg Med. 2020. PMID: 31171439
-
Recognizing the various presentations of appendicitis.Nurse Pract. 1999 Aug;24(8):42, 44, 49, 52-3; quiz 54-5. Nurse Pract. 1999. PMID: 10479109 Review.
-
Evidence-based approach to the diagnosis of appendicitis in children.Pediatr Emerg Care. 2004 Oct;20(10):690-8; quiz 699-701. doi: 10.1097/01.pec.0000142957.34501.8d. Pediatr Emerg Care. 2004. PMID: 15454747 Review. No abstract available.
Cited by
-
A Descriptive Analysis of the Cumulative Experiences of Emergency Medicine Residents in the Pediatric Emergency Department.AEM Educ Train. 2020 Jun 25;5(2):e10462. doi: 10.1002/aet2.10462. eCollection 2021 Apr. AEM Educ Train. 2020. PMID: 33796805 Free PMC article.
-
Survey of efficacy of pediatric appendicitis score in Iranian patients less than 18 years old referred to the emergency department.J Family Med Prim Care. 2019 Nov 15;8(11):3700-3705. doi: 10.4103/jfmpc.jfmpc_740_19. eCollection 2019 Nov. J Family Med Prim Care. 2019. PMID: 31803676 Free PMC article.
-
Predictive Factors of Acute Appendicitis and Its Outcomes Among the Pediatric Age Group.Cureus. 2025 Jan 24;17(1):e77925. doi: 10.7759/cureus.77925. eCollection 2025 Jan. Cureus. 2025. PMID: 39996225 Free PMC article.
-
Validation and Comparison of Pediatric Appendicitis Scores and Management Strategies (Project SPASMS): Protocol for a Prospective Multicenter Observational Study.JMIR Res Protoc. 2025 Jun 27;14:e67941. doi: 10.2196/67941. JMIR Res Protoc. 2025. PMID: 40577711 Free PMC article.
-
Trends and Predictors of Pediatric Negative Appendectomy Rates: A Single-Centre Retrospective Study.Children (Basel). 2023 May 15;10(5):887. doi: 10.3390/children10050887. Children (Basel). 2023. PMID: 37238435 Free PMC article.
References
-
- Barrett ML, Hines AL, Andrews RM. Trends in Rates of Perforated Appendix, 2001-2010: Healthcare Cost and Utilization Project (HCUP) Statistical Brief #159. Rockville, MD: Agency for Healthcare Research and Quality; 2013
-
- Shah SR, Sinclair KA, Theut SB, Johnson KM, Holcomb GW III, St Peter SD. Computed tomography utilization for the diagnosis of acute appendicitis in children decreases with a diagnostic algorithm. Ann Surg. 2016;264(3):474–481 - PubMed
-
- Depinet H, von Allmen D, Towbin A, Hornung R, Ho M, Alessandrini E. Risk stratification to decrease unnecessary diagnostic imaging for acute appendicitis. Pediatrics. 2016;138(3):e20154031. - PubMed
-
- Kharbanda AB, Madhok M, Krause E, et al. . Implementation of electronic clinical decision support for pediatric appendicitis. Pediatrics. 2016;137(5):e20151745. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

