Association of Inhaled Corticosteroids and Long-Acting Muscarinic Antagonists With Asthma Control in Patients With Uncontrolled, Persistent Asthma: A Systematic Review and Meta-analysis
- PMID: 29554174
- PMCID: PMC5876909
- DOI: 10.1001/jama.2018.2757
Association of Inhaled Corticosteroids and Long-Acting Muscarinic Antagonists With Asthma Control in Patients With Uncontrolled, Persistent Asthma: A Systematic Review and Meta-analysis
Erratum in
-
Error in a Figure.JAMA. 2018 May 8;319(18):1939. doi: 10.1001/jama.2018.5089. JAMA. 2018. PMID: 29800997 Free PMC article. No abstract available.
Abstract
Importance: Long-acting muscarinic antagonists (LAMAs) are a potential adjunct therapy to inhaled corticosteroids in the management of persistent asthma.
Objective: To conduct a systematic review and meta-analysis of the effects associated with LAMA vs placebo or vs other controllers as an add-on therapy to inhaled corticosteroids and the use of a LAMA as add-on therapy to inhaled corticosteroids and long-acting β-agonists (LABAs; hereafter referred to as triple therapy) vs inhaled corticosteroids and LABA in patients with uncontrolled, persistent asthma.
Data sources: MEDLINE, EMBASE, Cochrane databases, and clinical trial registries (earliest date through November 28, 2017).
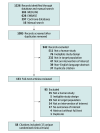
Study selection: Two reviewers selected randomized clinical trials or observational studies evaluating a LAMA vs placebo or vs another controller as an add-on therapy to inhaled corticosteroids or triple therapy vs inhaled corticosteroids and LABA in patients with uncontrolled, persistent asthma reporting on an outcome of interest.
Data extraction and synthesis: Meta-analyses using a random-effects model was conducted to calculate risk ratios (RRs), risk differences (RDs), and mean differences (MDs) with corresponding 95% CIs. Citation screening, data abstraction, risk assessment, and strength-of-evidence grading were completed by 2 independent reviewers.
Main outcomes and measures: Asthma exacerbations.
Results: Of 1326 records identified, 15 randomized clinical trials (N = 7122 patients) were included. Most trials assessed adding LAMA vs placebo or LAMA vs LABA to inhaled corticosteroids. Adding LAMA vs placebo to inhaled corticosteroids was associated with a significantly reduced risk of exacerbation requiring systemic corticosteroids (RR, 0.67 [95% CI, 0.48 to 0.92]; RD, -0.02 [95% CI, -0.04 to 0.00]). Compared with adding LABA, adding LAMA to inhaled corticosteroids was not associated with significant improvements in exacerbation risk (RR, 0.87 [95% CI, 0.53 to 1.42]; RD, 0.00 [95% CI, -0.02 to 0.02]), or any other outcomes of interest. Triple therapy was not significantly associated with improved exacerbation risk vs inhaled corticosteroids and LABA (RR, 0.84 [95% CI, 0.57 to 1.22]; RD, -0.01 [95% CI, -0.08 to 0.07]).
Conclusions and relevance: In this systematic review and meta-analysis, the use of LAMA compared with placebo as add-on therapy to inhaled corticosteroids was associated with a lower risk of asthma exacerbations; however, the association of LAMA with benefit may not be greater than that with LABA. Triple therapy was not associated with a lower risk of exacerbations.
Conflict of interest statement
Figures


Comment in
-
Time to Converge FDA Decisions and Evidence Syntheses for Long-Acting Muscarinic Antagonists and SMART in Guidelines for the Treatment of Asthma.JAMA. 2018 Apr 10;319(14):1441-1443. doi: 10.1001/jama.2018.2029. JAMA. 2018. PMID: 29554261 No abstract available.
-
Review: In uncontrolled, persistent asthma, adding LAMAs to inhaled corticosteroids reduce exacerbations.Ann Intern Med. 2018 Jul 17;169(2):JC4. doi: 10.7326/ACPJC-2018-169-2-004. Ann Intern Med. 2018. PMID: 30014093 No abstract available.
References
-
- National Heart, Lung, and Blood Institute . Expert panel report 3: guidelines for the diagnosis and management of asthma. https://www.ncbi.nlm.nih.gov/books/NBK7232/pdf/Bookshelf_NBK7232.pdf. Accessed March 5, 2018.
-
- Spiriva Respimat [package insert]. Ridgefield, CT: Boehringer Ingelheim Pharmaceuticals; 2016.
-
- National Heart, Lung and Blood Advisory Council Asthma Expert Working Group . Needs Assessment Report for Potential Update of the Expert Panel Report-3 (2007). Guidelines for the Diagnosis and Management of Asthma; 2015.
-
- Agency for Healthcare Research and Quality . Systematic review of intermittent inhaled corticosteroids and of long-acting muscarinic antagonists for asthma: research protocol. https://ahrq-ehc-application.s3.amazonaws.com/media/pdf/asthma-pharmacol.... Accessed March 5, 2018. - PubMed
-
- Sobieraj DM, Baker WL, Weeda ER, et al. Intermittent inhaled corticosteroids and long-acting muscarinic antagonists for asthma: comparative effectiveness review No. 194. https://effectivehealthcare.ahrq.gov/topics/asthma-pharmacologic-treatme.... Accessed March 19, 2018. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

