Statin use and the risk of Clostridium difficile infection: a systematic review with meta-analysis
- PMID: 29559802
- PMCID: PMC5856044
- DOI: 10.2147/IDR.S156475
Statin use and the risk of Clostridium difficile infection: a systematic review with meta-analysis
Abstract
Purpose: Statins have pleiotropic effects beyond cholesterol lowering by immune modulation. The association of statins with primary Clostridium difficile infection (CDI) is unclear as studies have reported conflicting findings. We performed a systematic review and meta-analysis to evaluate the association between statin use and CDI.
Patients and methods: We searched MEDLINE, Embase, and Web of Science from January 1978 to December 2016 for studies assessing the association between statin use and CDI. The Newcastle-Ottawa Scale was used to assess the methodologic quality of included studies. Weighted summary estimates were calculated using generalized inverse variance with random-effects model.
Results: Eight studies (6 case-control and 2 cohort) were included in the meta-analysis, which comprised 156,722 patients exposed to statins and 356,185 controls, with 34,849 total cases of CDI available in 7 studies. The rate of CDI in patients with statin use was 4.3%, compared with 7.8% in patients without statin use. An overall meta-analysis of 8 studies using the random-effects model demonstrated that statins may be associated with a decreased risk of CDI (maximally adjusted odds ratio [OR], 0.80; 95% CI, 0.66-0.97; P=0.02). There was significant heterogeneity among the studies, with an I2 of 79%. No publication bias was seen. Meta-analysis of studies that adjusted for confounders revealed no protective effect of statins (adjusted OR, 0.84; 95% CI, 0.70-1.01; P=0.06, I2=75%). However, a meta-analysis of only full-text studies using the random-effects model demonstrated a decreased risk of CDI with the use of statins (OR 0.77; 95% CI, 0.61-0.99; P=0.04, I2=85%).
Conclusion: Meta-analyses of existing studies suggest that patients prescribed a statin may be at decreased risk for CDI. The results must be interpreted with caution given the significant heterogeneity and lack of benefit on analysis of studies that adjusted for confounders.
Keywords: Clostridium difficile infection; incidence; meta-analysis; statins.
Conflict of interest statement
Disclosure The authors report no conflicts of interest in this work.
Figures

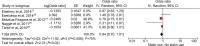

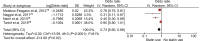
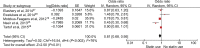

Similar articles
-
Statins & risk of Clostridium difficile infection: A meta-analysis.Indian J Med Res. 2019 Oct;150(4):359-364. doi: 10.4103/ijmr.IJMR_1973_17. Indian J Med Res. 2019. PMID: 31823917 Free PMC article.
-
Low Risk of Primary Clostridium difficile Infection With Tetracyclines: A Systematic Review and Metaanalysis.Clin Infect Dis. 2018 Feb 1;66(4):514-522. doi: 10.1093/cid/cix833. Clin Infect Dis. 2018. PMID: 29401273
-
Statin Effects on Incidence, Treatment Success, and Mortality of Clostridium difficile Infections.J Pharm Pract. 2020 Aug;33(4):497-505. doi: 10.1177/0897190019854956. Epub 2019 Jun 19. J Pharm Pract. 2020. PMID: 31216928 Review.
-
Meta-analysis comparing the effects of statins on the risk of Clostridium difficile diarrhea.Proc (Bayl Univ Med Cent). 2018 Sep 19;31(4):447-452. doi: 10.1080/08998280.2018.1472994. eCollection 2018 Oct. Proc (Bayl Univ Med Cent). 2018. PMID: 31007627 Free PMC article.
-
The Impact of Clostridium difficile Infection on Mortality in Patients With Inflammatory Bowel Disease: A Systematic Review and Meta-Analysis.J Clin Gastroenterol. 2019 Feb;53(2):127-133. doi: 10.1097/MCG.0000000000000968. J Clin Gastroenterol. 2019. PMID: 29206751
Cited by
-
Novel risk factors and outcomes in inflammatory bowel disease patients with Clostridioides difficile infection.Therap Adv Gastroenterol. 2021 Mar 12;14:1756284821997792. doi: 10.1177/1756284821997792. eCollection 2021. Therap Adv Gastroenterol. 2021. PMID: 33786065 Free PMC article.
-
Effect of Statins on the Risk of Poststroke Pneumonia: National Population-Based Cohort Study.Infect Drug Resist. 2020 Aug 6;13:2689-2698. doi: 10.2147/IDR.S258420. eCollection 2020. Infect Drug Resist. 2020. PMID: 32982323 Free PMC article.
-
Statins & risk of Clostridium difficile infection: A meta-analysis.Indian J Med Res. 2019 Oct;150(4):359-364. doi: 10.4103/ijmr.IJMR_1973_17. Indian J Med Res. 2019. PMID: 31823917 Free PMC article.
-
Clostridium difficile Infection: An Epidemiology Update.Clin Colon Rectal Surg. 2020 Mar;33(2):49-57. doi: 10.1055/s-0040-1701229. Epub 2020 Feb 25. Clin Colon Rectal Surg. 2020. PMID: 32104156 Free PMC article. Review.
References
-
- Khanna S, Pardi DS. The growing incidence and severity of Clostridium difficile infection in inpatient and outpatient settings. Expert Rev Gastroenterol Hepatol. 2010;4(4):409–416. - PubMed
-
- Li SS, Zhu A, Benes V, et al. Durable coexistence of donor and recipient strains after fecal microbiota transplantation. Science. 2016;352(6285):586–589. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources

