Germline breast cancer susceptibility gene mutations and breast cancer outcomes
- PMID: 29566657
- PMCID: PMC5863855
- DOI: 10.1186/s12885-018-4229-5
Germline breast cancer susceptibility gene mutations and breast cancer outcomes
Abstract
Background: It is unclear whether germline breast cancer susceptibility gene mutations affect breast cancer related outcomes. We wanted to evaluate mutation patterns in 20 breast cancer susceptibility genes and correlate the mutations with clinical characteristics to determine the effects of these germline mutations on breast cancer prognosis.
Methods: The study cohort included 480 ethnic Chinese individuals in Taiwan with at least one of the six clinical risk factors for hereditary breast cancer: family history of breast or ovarian cancer, young age of onset for breast cancer, bilateral breast cancer, triple negative breast cancer, both breast and ovarian cancer, and male breast cancer. PCR-enriched amplicon-sequencing on a next generation sequencing platform was used to determine the germline DNA sequences of all exons and exon-flanking regions of the 20 genes. Protein-truncating variants were identified as pathogenic.
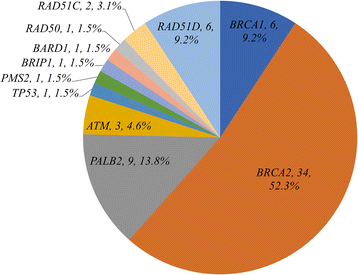
Results: We detected a 13.5% carrier rate of pathogenic germline mutations, with BRCA2 being the most prevalent and the non-BRCA genes accounting for 38.5% of the mutation carriers. BRCA mutation carriers were more likely to be diagnosed of breast cancer with lymph node involvement (66.7% vs 42.6%; P = 0.011), and had significantly worse breast cancer specific outcomes. The 5-year disease-free survival was 73.3% for BRCA mutation carriers and 91.1% for non-carriers (hazard ratio for recurrence or death 2.42, 95% CI 1.29-4.53; P = 0.013). After adjusting for clinical prognostic factors, BRCA mutation remained an independent poor prognostic factor for cancer recurrence or death (adjusted hazard ratio 3.04, 95% CI 1.40-6.58; P = 0.005). Non-BRCA gene mutation carriers did not exhibit any significant difference in cancer characteristics or outcomes compared to those without detected mutations. Among the risk factors for hereditary breast cancer, the odds of detecting a germline mutation increased significantly with having bilateral breast cancer (adjusted odds ratio 3.27, 95% CI 1.64-6.51; P = 0.0008) or having more than one risk factor (odds ratio 2.07, 95% CI 1.22-3.51; P = 0.007).
Conclusions: Without prior knowledge of the mutation status, BRCA mutation carriers had more advanced breast cancer on initial diagnosis and worse cancer-related outcomes. Optimal approach to breast cancer treatment for BRCA mutation carriers warrants further investigation.
Keywords: BRCA1 & BRCA2; Breast cancer; Breast cancer prognosis; Cancer susceptibility gene; Next generation sequencing.
Conflict of interest statement
Ethics approval and consent to participate
The study was conducted in accordance with the Declaration of Helsinki, and the study protocol was approved by the Institutional Review Board Committee at Koo Foundation Sun Yat-Sen Cancer Center (case No. 20141222A). Written informed consent was obtained from each study participant.
Consent for publication
Not applicable.
Competing interests
None of the authors have any competing interests.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Figures

References
-
- Robson ME, Bradbury AR, Arun B, Domchek SM, Ford JM, Hampel HL, et al. American Society of Clinical Oncology policy statement update: genetic and genomic testing for Cancer susceptibility. Journal of clinical oncology : official journal of the American Society of Clinical Oncology. 2015;33:3660–3667. doi: 10.1200/JCO.2015.63.0996. - DOI - PubMed
-
- Kurian AW, Hare EE, Mills MA, Kingham KE, McPherson L, Whittemore AS, et al. Clinical evaluation of a multiple-gene sequencing panel for hereditary cancer risk assessment. Journal of clinical oncology : official journal of the American Society of Clinical Oncology. 2014;32:2001–2009. doi: 10.1200/JCO.2013.53.6607. - DOI - PMC - PubMed
Publication types
MeSH terms
Grants and funding
- MOST104-3114-Y-368-002/Ministry of Science and Technology, Taiwan/International
- MOST106-0210-01-15-02/Ministry of Science and Technology, Taiwan/International
- MOST106-0210-01-15-04/Ministry of Science and Technology, Taiwan/International
- MOHW106-TDU-B-212-134004/Ministry of Health and Welfare/International
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

