ABCs of the degenerative spine
- PMID: 29569215
- PMCID: PMC5893484
- DOI: 10.1007/s13244-017-0584-z
ABCs of the degenerative spine
Abstract
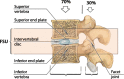
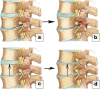
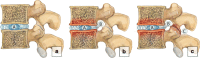
Degenerative changes in the spine have high medical and socioeconomic significance. Imaging of the degenerative spine is a frequent challenge in radiology. The pathogenesis of this degenerative process represents a biomechanically related continuum of alterations, which can be identified with different imaging modalities. The aim of this article is to review radiological findings involving the intervertebral discs, end plates, bone marrow changes, facet joints and the spinal canal in relation to the pathogenesis of degenerative changes in the spine. Findings are described in association with the clinical symptoms they may cause, with a brief review of the possible treatment options. The article provides an illustrated review on the topic for radiology residents.
Teaching points: • The adjacent vertebrae, intervertebral disc, ligaments and facet joints constitute a spinal unit. • Degenerative change is a response to insults, such as mechanical or metabolic injury. • Spine degeneration is a biomechanically related continuum of alterations evolving over time.
Keywords: Degenerative spine; Intervertebral disc herniation; Modic changes; Spinal canal stenosis; Spondylosis.
Figures
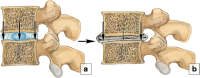



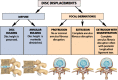
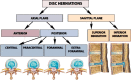
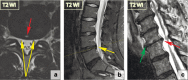
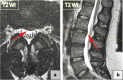
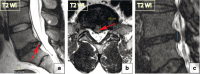
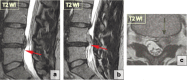




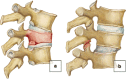

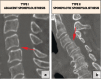

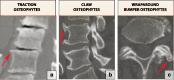
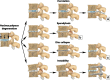

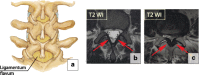
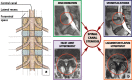



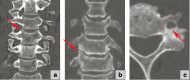
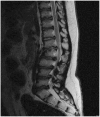
Similar articles
-
[Adjacent segment degeneration after lumbosacral fusion in spondylolisthesis: a retrospective radiological and clinical analysis].Acta Chir Orthop Traumatol Cech. 2010 Apr;77(2):124-30. Acta Chir Orthop Traumatol Cech. 2010. PMID: 20447355 Czech.
-
[Pathophysiology, neurology and diagnostic radiology of degenerative diseases of the lumbar spine].Radiologe. 2007 Feb;47(2):167-83; quiz 184-5. doi: 10.1007/s00117-007-1471-2. Radiologe. 2007. PMID: 17285273 Review. German.
-
[Anatomical background of low back pain: variability and degeneration of the lumbar spinal canal and intervertebral disc].Schmerz. 2001 Dec;15(6):418-24. doi: 10.1007/s004820100026. Schmerz. 2001. PMID: 11793145 German.
-
The radiological symptoms of lumbar disc herniation and degenerative changes of the lumbar intervertebral discs.Med Sci Monit. 2004 Jun;10 Suppl 3:112-4. Med Sci Monit. 2004. PMID: 16538211
-
Cervical spondylosis anatomy: pathophysiology and biomechanics.Neurosurgery. 2007 Jan;60(1 Supp1 1):S7-13. doi: 10.1227/01.NEU.0000215430.86569.C4. Neurosurgery. 2007. PMID: 17204889 Review.
Cited by
-
Natural products can modulate inflammation in intervertebral disc degeneration.Front Pharmacol. 2023 Feb 16;14:1150835. doi: 10.3389/fphar.2023.1150835. eCollection 2023. Front Pharmacol. 2023. PMID: 36874009 Free PMC article. Review.
-
Association of Hallux Valgus with Degenerative Spinal Diseases: A Population-Based Cohort Study.Int J Environ Res Public Health. 2023 Jan 9;20(2):1152. doi: 10.3390/ijerph20021152. Int J Environ Res Public Health. 2023. PMID: 36673906 Free PMC article.
-
Perspective on Intradiscal Therapies for Lumbar Discogenic Pain: State of the Science, Knowledge Gaps, and Imperatives for Clinical Adoption.J Pain Res. 2024 Mar 18;17:1171-1182. doi: 10.2147/JPR.S441180. eCollection 2024. J Pain Res. 2024. PMID: 38524692 Free PMC article.
-
Unlocking Osteoporosis Diagnosis: Unveiling the Potential of MRI-Based Vertebral Bone Quality Score.Cureus. 2025 Apr 12;17(4):e82154. doi: 10.7759/cureus.82154. eCollection 2025 Apr. Cureus. 2025. PMID: 40364868 Free PMC article.
-
Perivascular mechanical environment: A narrative review of the role of externally applied mechanical force in the pathogenesis of atherosclerosis.Front Cardiovasc Med. 2022 Oct 19;9:944356. doi: 10.3389/fcvm.2022.944356. eCollection 2022. Front Cardiovasc Med. 2022. PMID: 36337892 Free PMC article. Review.
References
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources

