Vascular Abnormalities within Normal Appearing Tissue in Chronic Traumatic Brain Injury
- PMID: 29609518
- PMCID: PMC6157375
- DOI: 10.1089/neu.2018.5684
Vascular Abnormalities within Normal Appearing Tissue in Chronic Traumatic Brain Injury
Abstract
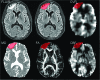
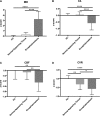
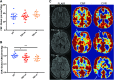
Magnetic resonance imaging (MRI) is a powerful tool for visualizing traumatic brain injury(TBI)-related lesions. Trauma-induced encephalomalacia is frequently identified by its hyperintense appearance on fluid-attenuated inversion recovery (FLAIR) sequences. In addition to parenchymal lesions, TBI commonly results in cerebral microvascular injury, but its anatomical relationship to parenchymal encephalomalacia is not well characterized. The current study utilized a multi-modal MRI protocol to assess microstructural tissue integrity (by mean diffusivity [MD] and fractional aniosotropy [FA]) and altered vascular function (by cerebral blood flow [CBF] and cerebral vascular reactivity [CVR]) within regions of visible encephalomalacia and normal appearing tissue in 27 chronic TBI (minimum 6 months post-injury) subjects. Fifteen subjects had visible encephalomalacias whereas 12 did not have evident lesions on MRI. Imaging from 14 age-matched healthy volunteers were used as controls. CBF was assessed by arterial spin labeling (ASL) and CVR by measuring the change in blood-oxygen-level-dependent (BOLD) MRI during a hypercapnia challenge. There was a significant reduction in FA, CBF, and CVR with a complementary increase in MD within regions of FLAIR-visible encephalomalacia (p < 0.05 for all comparisons). In normal-appearing brain regions, only CVR was significantly reduced relative to controls (p < 0.05). These findings indicate that vascular dysfunction represents a TBI endophenotype that is distinct from structural injury detected using conventional MRI, may be present even in the absence of visible structural injury, and persists long after trauma. CVR may serve as a useful diagnostic and pharmacodynamic imaging biomarker of traumatic microvascular injury.
Keywords: FLAIR; cerebral blood flow; cerebral vascular reactivity; diffusion tensor imaging; traumatic brain injury.
Conflict of interest statement
No competing financial interests exist.
Figures

Similar articles
-
Imaging biomarkers of vascular and axonal injury are spatially distinct in chronic traumatic brain injury.J Cereb Blood Flow Metab. 2021 Aug;41(8):1924-1938. doi: 10.1177/0271678X20985156. Epub 2021 Jan 14. J Cereb Blood Flow Metab. 2021. PMID: 33444092 Free PMC article.
-
Imaging of Cerebrovascular Function in Chronic Traumatic Brain Injury.J Neurotrauma. 2018 May 15;35(10):1116-1123. doi: 10.1089/neu.2017.5114. Epub 2018 Mar 20. J Neurotrauma. 2018. PMID: 29065769 Free PMC article.
-
Assessment of cerebrovascular dysfunction after traumatic brain injury with fMRI and fNIRS.Neuroimage Clin. 2020;25:102086. doi: 10.1016/j.nicl.2019.102086. Epub 2019 Nov 11. Neuroimage Clin. 2020. PMID: 31790877 Free PMC article.
-
Advanced neuroimaging in traumatic brain injury: an overview.Neurosurg Focus. 2019 Dec 1;47(6):E17. doi: 10.3171/2019.9.FOCUS19652. Neurosurg Focus. 2019. PMID: 32364704 Review.
-
Cerebral Vascular Injury in Traumatic Brain Injury.Exp Neurol. 2016 Jan;275 Pt 3:353-366. doi: 10.1016/j.expneurol.2015.05.019. Epub 2015 Jun 3. Exp Neurol. 2016. PMID: 26048614 Review.
Cited by
-
Potential Neuroprotective Role of Neurotrophin in Traumatic Brain Injury.CNS Neurol Disord Drug Targets. 2024;23(10):1189-1202. doi: 10.2174/0118715273289222231219094225. CNS Neurol Disord Drug Targets. 2024. PMID: 38279761 Review.
-
Changes in Plasma von Willebrand Factor and Cellular Fibronectin in MRI-Defined Traumatic Microvascular Injury.Front Neurol. 2019 Mar 26;10:246. doi: 10.3389/fneur.2019.00246. eCollection 2019. Front Neurol. 2019. PMID: 30972003 Free PMC article.
-
Delayed Traumatic Intracerebral Hematoma: A Pathophysiological Classification and Literature Review.Cureus. 2023 Aug 5;15(8):e42987. doi: 10.7759/cureus.42987. eCollection 2023 Aug. Cureus. 2023. PMID: 37671206 Free PMC article. Review.
-
Psilocybin as a Treatment for Repetitive Mild Head Injury: Evidence from Neuroradiology and Molecular Biology.bioRxiv [Preprint]. 2025 Feb 11:2025.02.03.636248. doi: 10.1101/2025.02.03.636248. bioRxiv. 2025. PMID: 39975204 Free PMC article. Preprint.
-
Cerebral Blood Flow and Its Connectivity Deficits in Mild Traumatic Brain Injury at the Acute Stage.Neural Plast. 2020 Jul 1;2020:2174371. doi: 10.1155/2020/2174371. eCollection 2020. Neural Plast. 2020. PMID: 32684919 Free PMC article.
References
-
- Center for Disease Control and Prevention, National Center for Injury Prevention and Control, Division of Unintentional Injury Prevention. (2010). Rates of TBI-related Emergency Department Visits, Hospitalizations, and Deaths: United States, 2001–2010 | Data | Centers for Disease Control and Prevention. Available at https://data.cdc.gov/Traumatic-Brain-Injury-/Rates-of-TBI-related-Emerge....
-
- Kenney K., Amyot F., Haber M., Pronger A., Bogoslovsky T., Moore C., and Diaz-Arrastia R. (2016). Cerebral vascular injury in traumatic brain injury. Exp. Neurol. 275, Pt. 3, 353–366 - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

