Cost-benefit analysis of antibiofilm microbiological techniques for peri-prosthetic joint infection diagnosis
- PMID: 29609540
- PMCID: PMC5879767
- DOI: 10.1186/s12879-018-3050-8
Cost-benefit analysis of antibiofilm microbiological techniques for peri-prosthetic joint infection diagnosis
Abstract
Background: Implant-related infections, including those of peri-prosthetic joint (PJIs), osteosynthesis and other biomaterials, are biofilm-related. Pathogen identification is considered the diagnostic benchmark; however, the presence of bacterial biofilms makes pathogen detection with traditional microbiological techniques only partially effective. To improve microbiological diagnostic accuracy, some biofilm debonding techniques have been recently proposed. Aim of this health economics assessment study was to evaluate their economic impact on hospital costs.
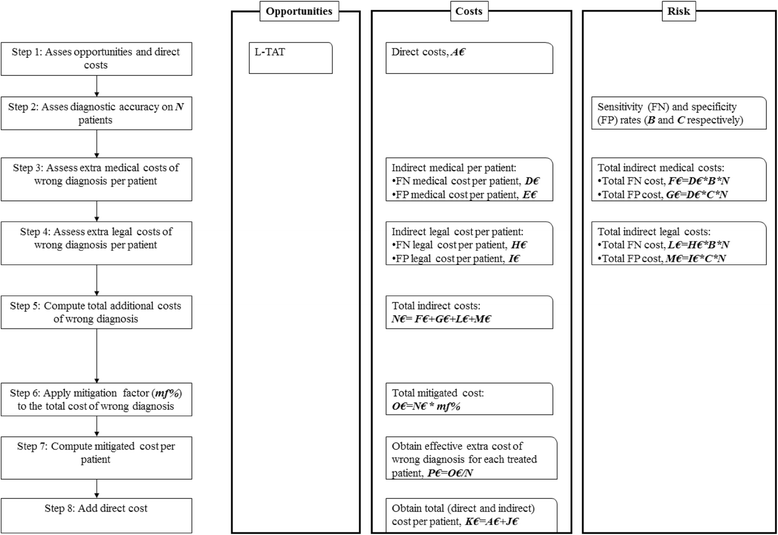
Methods: Direct and indirect hospital costs connected with the routine introduction of sonication and dithiothreitol treatment applied to hip and knee PJIs and of tissue cultures were examined. In particular the consequences of diagnostic inaccuracy, the opportunities, costs, and risks of each technique were calculated.
Results: Considering an average of five samples per patient, processed separately with traditional tissue culture with or without sonication of prosthetic components, or pooled together using the MicroDTTect device (a close system for sample collection, transport and treatment with Dithiothreitol for microbial release from biofilm), the overall mean direct cost per patient was € 397 and € 393 for sonication or MicroDTTect, respectively, compared to € 308 for traditional tissue cultures. In terms of opportunity costs, MicroDTTect was the most effective technique, allowing for a 35% or 55% reduction in time required for sample treatment, compared to tissue cultures combined or not with sonication, respectively. Pooling together direct and indirect costs associated with false positive and negative results of the different diagnostic techniques, unnecessary medical treatments and possible medical claims, MicroDTTect or sonication become increasingly cost-effective when the extra-costs, generated by diagnostic inaccuracy of traditional tissue culture, took place, respectively, in 2% or 20% or more of the patients.
Conclusions: This is the first study specifically focused on the economic impact of the routine clinical use of microbiological antibiofilm sampling and processing techniques in orthopaedics. Although our results may suffer from a potential country and hospital bias, as the data collection process for direct and indirect costs is specific to each institution and country, this analysis highlights the potential economic advantage to hospitals associated with the routine introduction of antibiofilm techniques for microbiological diagnosis of PJI.
Keywords: Analysis; Benefit; Biofilm; Cost; Diagnostic; Economics; Joint infection.
Conflict of interest statement
Ethics approval and consent to participate
Not applicable
Consent for publication
Not applicable
Competing interests
The authors declare that they have no competing interests
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Figures
References
-
- No author cited . The diagnosis of periprosthetic joint infections in the hip or knee. Guideline and evidence report. 1. Rosmont: American Academy of Orthopedic Surgeons; 2010.
-
- Parvizi J, Zmistowski B, Berbari EF, Bauer TW, Springer BD, Della Valle CJ, Garvin KL, Mont MA, Wongworawat MD, Zalavras CG. New definition for periprosthetic joint infection: from the workgroup of the musculoskeletal infection society. Clin Orthop Relat Res. 2011;469:2992–2994. doi: 10.1007/s11999-011-2102-9. - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources