Longitudinal Assessment of Multidrug-Resistant Organisms in Newly Admitted Nursing Facility Patients: Implications for an Evolving Population
- PMID: 29635360
- PMCID: PMC6117444
- DOI: 10.1093/cid/ciy194
Longitudinal Assessment of Multidrug-Resistant Organisms in Newly Admitted Nursing Facility Patients: Implications for an Evolving Population
Abstract
Background: The spread of multidrug-resistant organisms (MDROs) is a global concern, and much about transmission in healthcare systems remains unknown. To reduce hospital stays, nursing facilities (NFs) have increasingly assumed care of post-acute populations. We estimate the prevalence of MDRO colonization in NF patients on enrollment and discharge to community settings, risk factors for colonization, and rates of acquiring MDROs during the stay.
Methods: We conducted a prospective, longitudinal cohort study of newly admitted patients in 6 NFs in southeast Michigan using active microbial surveillance of multiple anatomic sites sampled at enrollment, days 14 and 30, and monthly thereafter for up to 6 months.
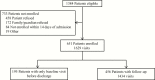
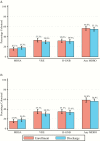
Results: We enrolled 651 patients and collected 7526 samples over 1629 visits, with an average of 29 days of follow-up per participant. Nearly all participants were admitted for post-acute care (95%). More than half (56.8%) were colonized with MDROs at enrollment: methicillin-resistant Staphylococcus aureus (MRSA), 16.1%; vancomycin-resistant enterococci (VRE), 33.2%; and resistant gram-negative bacilli (R-GNB), 32.0%. Risk factors for colonization at enrollment included prolonged hospitalization (>14 days), functional disability, antibiotic use, or device use. Rates per 1000 patient-days of acquiring a new MDRO were MRSA, 3.4; VRE, 8.2; and R-GNB, 13.6. MDRO colonization at discharge was similar to that at enrollment (56.4%): MRSA, 18.4%; VRE, 30.3%; and R-GNB, 33.6%.
Conclusions: Short-stay NF patients exhibit a high prevalence of MDROs near the time of admission, as well as at discharge, and may serve as a reservoir for spread in other healthcare settings. Future interventions to reduce MDROs should specifically target this population.
Figures


References
-
- Medicare Payment Advisory Commission. Report to the Congress: Medicare payment policy 2017. Available at: http://www.medpac.gov/docs/default-source/reports/mar17_entirereport2246.... Accessed 14 November 2017.
-
- Burke RE, Juarez-Colunga E, Levy C, Prochazka AV, Coleman EA, Ginde AA. Rise of post-acute care facilities as a discharge destination of US hospitalizations. JAMA Intern Med 2015; 175:295–6. - PubMed
-
- Jenq GY, Tinetti ME. Post-acute care: who belongs where?JAMA Intern Med 2015; 175:296–7. - PubMed
-
- Weiner LM, Webb AK, Limbago B, et al. . Antimicrobial-resistant pathogens associated with healthcare-associated infections: summary of data reported to the National Healthcare Safety Network at the Centers for Disease Control and Prevention, 2011–2014. Infect Control Hosp Epidemiol 2016; 37:1288–301. - PMC - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

