Injectable, porous, biohybrid hydrogels incorporating decellularized tissue components for soft tissue applications
- PMID: 29649634
- PMCID: PMC5985206
- DOI: 10.1016/j.actbio.2018.04.003
Injectable, porous, biohybrid hydrogels incorporating decellularized tissue components for soft tissue applications
Abstract
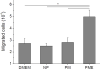
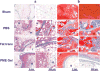
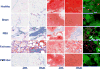
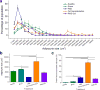
Biodegradable injectable hydrogels have been extensively studied and evaluated in various medical applications such as for bulking agents, drug delivery reservoirs, temporary barriers, adhesives, and cell delivery matrices. Where injectable hydrogels are intended to facilitate a healing response, it may be desirable to encourage rapid cellular infiltration into the hydrogel volume from the tissue surrounding the injection site. In this study, we developed a platform technique to rapidly form pores in a thermally responsive injectable hydrogel, poly(NIPAAm-co-VP-co-MAPLA) by using mannitol particles as porogens. In a rat hindlimb muscle injection model, hydrogels incorporating porosity had significantly accelerated cellular infiltration. To influence the inflammatory response to the injected hydrogel, enzymatically digested urinary bladder matrix (UBM) was mixed with the solubilized hydrogel. The presence of UBM was associated with greater polarization of the recruited macrophage population to the M2 phenotype, indicating a more constructive foreign body response. The hybrid hydrogel positively affected the wound healing outcomes of defects in rabbit adipose tissue with negligible inflammation and fibrosis, whereas scar formation and chronic inflammation were observed with autotransplantation and in saline injected groups. These results demonstrate the value of combining the effects of promoting cell infiltration and mediating the foreign body response for improved biomaterials options soft tissue defect filling applications.
Statement of significance: Our objective was to develop a fabrication process to create porous injectable hydrogels incorporating decellularized tissue digest material. This new hydrogel material was expected to exhibit faster cellular infiltration and a greater extent of pro-M2 macrophage polarization compared to control groups not incorporating each of the functional components. Poly(NIPAAm-co-VP-co-MAPLA) was chosen as the representative thermoresponsive hydrogel, and mannitol particles and digested urinary bladder matrix (UBM) were selected as the porogen and the bioactive decellularized material components respectively. In rat hindlimb intramuscular injection models, this new hydrogel material induced more rapid cellular infiltration and a greater extent of M2 macrophage polarization compared to control groups not incorporating all of the functional components. The hybrid hydrogel positively affected the wound healing outcomes of defects in rabbit adipose tissue with negligible inflammation and fibrosis, whereas scar formation and chronic inflammation were observed with autotransplantation and in saline injected groups. The methodology of this report provides a straightforward and convenient mechanism to promote cell infiltration and mediate foreign body response in injectable hydrogels for soft tissue applications. We believe that the readership of Acta Biomaterialia will find the work of interest both for its specific results and general translatability of the findings.
Keywords: Cell infiltration; Decellularized extracellular matrix; Foreign body response; Hydrogel; Porous biomaterial; Soft tissue repair.
Copyright © 2018 Acta Materialia Inc. Published by Elsevier Ltd. All rights reserved.
Figures










Similar articles
-
Decellularized porcine dermal hydrogel enhances implant-based wound healing in the setting of irradiation.Acta Biomater. 2025 Jan 1;191:260-275. doi: 10.1016/j.actbio.2024.11.009. Epub 2024 Nov 8. Acta Biomater. 2025. PMID: 39522628
-
Intervening to Preserve Function in Ischemic Cardiomyopathy with a Porous Hydrogel and Extracellular Matrix Composite in a Rat Myocardial Infarction Model.Adv Healthc Mater. 2025 Jan;14(2):e2402757. doi: 10.1002/adhm.202402757. Epub 2024 Nov 3. Adv Healthc Mater. 2025. PMID: 39491520 Free PMC article.
-
Body temperature-activated protein-based injectable adhesive hydrogel incorporated with decellularized adipose extracellular matrix for tissue-specific regenerative stem cell therapy.Acta Biomater. 2020 Sep 15;114:244-255. doi: 10.1016/j.actbio.2020.07.033. Epub 2020 Jul 21. Acta Biomater. 2020. PMID: 32702528
-
Extracellular matrix hydrogels from decellularized tissues: Structure and function.Acta Biomater. 2017 Feb;49:1-15. doi: 10.1016/j.actbio.2016.11.068. Epub 2016 Dec 1. Acta Biomater. 2017. PMID: 27915024 Free PMC article. Review.
-
Advances in bioactive glass-containing injectable hydrogel biomaterials for tissue regeneration.Acta Biomater. 2021 Dec;136:1-36. doi: 10.1016/j.actbio.2021.09.034. Epub 2021 Sep 23. Acta Biomater. 2021. PMID: 34562661 Review.
Cited by
-
Programming temporal stiffness cues within extracellular matrix hydrogels for modelling cancer niches.Mater Today Bio. 2024 Feb 16;25:101004. doi: 10.1016/j.mtbio.2024.101004. eCollection 2024 Apr. Mater Today Bio. 2024. PMID: 38420142 Free PMC article.
-
The Unfulfilled Potential of Synthetic and Biological Hydrogel Membranes in the Treatment of Abdominal Hernias.Gels. 2024 Nov 21;10(12):754. doi: 10.3390/gels10120754. Gels. 2024. PMID: 39727512 Free PMC article. Review.
-
Hydrogel Properties and Their Impact on Regenerative Medicine and Tissue Engineering.Molecules. 2020 Dec 8;25(24):5795. doi: 10.3390/molecules25245795. Molecules. 2020. PMID: 33302592 Free PMC article. Review.
-
Development and in vitro evaluation of biomimetic injectable hydrogels from decellularized human nerves for central nervous system regeneration.Mater Today Bio. 2025 Jan 11;31:101483. doi: 10.1016/j.mtbio.2025.101483. eCollection 2025 Apr. Mater Today Bio. 2025. PMID: 39896276 Free PMC article.
-
Sterilization and disinfection methods for decellularized matrix materials: Review, consideration and proposal.Bioact Mater. 2021 Feb 27;6(9):2927-2945. doi: 10.1016/j.bioactmat.2021.02.010. eCollection 2021 Sep. Bioact Mater. 2021. PMID: 33732964 Free PMC article. Review.
References
-
- Ko DY, Shinde UP, Yeon B, Jeong B. Recent progress of in situ formed gels for biomedical applications. Prog Polym Sci. 2012
-
- He C, Kim SW, Lee DS. In situ gelling stimuli-sensitive block copolymer hydrogels for drug delivery. J Control Release. 2008:189–207. - PubMed
-
- Dou QQ, Liow SS, Ye E, Lakshminarayanan R, Loh XJ. Biodegradable Thermogelling Polymers: Working Towards Clinical Applications. Adv Healthc Mater. 2014 n/a-n/a. - PubMed
-
- Miao B, Song C, Ma G. Injectable thermosensitive hydrogels for intra-articular delivery of methotrexate. J Appl Polym Sci. 2011:2139–2145.
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials

