Potent antitumor efficacy of anti-GD2 CAR T cells in H3-K27M+ diffuse midline gliomas
- PMID: 29662203
- PMCID: PMC6214371
- DOI: 10.1038/s41591-018-0006-x
Potent antitumor efficacy of anti-GD2 CAR T cells in H3-K27M+ diffuse midline gliomas
Abstract
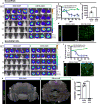
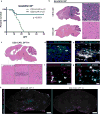
Diffuse intrinsic pontine glioma (DIPG) and other diffuse midline gliomas (DMGs) with mutated histone H3 K27M (H3-K27M)1-5 are aggressive and universally fatal pediatric brain cancers 6 . Chimeric antigen receptor (CAR)-expressing T cells have mediated impressive clinical activity in B cell malignancies7-10, and recent results suggest benefit in central nervous system malignancies11-13. Here, we report that patient-derived H3-K27M-mutant glioma cell cultures exhibit uniform, high expression of the disialoganglioside GD2. Anti-GD2 CAR T cells incorporating a 4-1BBz costimulatory domain 14 demonstrated robust antigen-dependent cytokine generation and killing of DMG cells in vitro. In five independent patient-derived H3-K27M+ DMG orthotopic xenograft models, systemic administration of GD2-targeted CAR T cells cleared engrafted tumors except for a small number of residual GD2lo glioma cells. To date, GD2-targeted CAR T cells have been well tolerated in clinical trials15-17. Although GD2-targeted CAR T cell administration was tolerated in the majority of mice bearing orthotopic xenografts, peritumoral neuroinflammation during the acute phase of antitumor activity resulted in hydrocephalus that was lethal in a fraction of animals. Given the precarious neuroanatomical location of midline gliomas, careful monitoring and aggressive neurointensive care management will be required for human translation. With a cautious multidisciplinary clinical approach, GD2-targeted CAR T cell therapy for H3-K27M+ diffuse gliomas of pons, thalamus and spinal cord could prove transformative for these lethal childhood cancers.
Conflict of interest statement
C.L.M, M.M., R.G.M., and C.W.M. are inventors on a patent application for GD2-directed CAR use for H3K27M DMG.
Figures


Comment in
-
CAR T cells for childhood diffuse midline gliomas.Nat Med. 2018 May;24(5):534-535. doi: 10.1038/s41591-018-0031-9. Nat Med. 2018. PMID: 29736025 No abstract available.
-
Anti-GD2 CAR T cells could prove transformative for H3-K27M+ diffuse midline gliomas.Transl Cancer Res. 2019 Mar;8(Suppl 2):S87-S93. doi: 10.21037/tcr.2018.08.21. Transl Cancer Res. 2019. PMID: 35117070 Free PMC article. No abstract available.
References
Methods-only References
-
- Sen G, Chakraborty M, Foon KA, Reisfeld RA, Bhattacharya-Chatterjee MB. Induction of IgG antibodies by an anti-idiotype antibody mimicking disialoganglioside GD2. J Immunother. 1998;21:75–83. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

