Interleukin-15-Cultured Dendritic Cells Enhance Anti-Tumor Gamma Delta T Cell Functions through IL-15 Secretion
- PMID: 29692776
- PMCID: PMC5902500
- DOI: 10.3389/fimmu.2018.00658
Interleukin-15-Cultured Dendritic Cells Enhance Anti-Tumor Gamma Delta T Cell Functions through IL-15 Secretion
Abstract
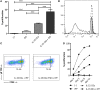
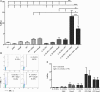
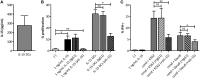
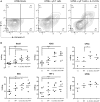
Dendritic cell (DC) vaccination can be an effective post-remission therapy for acute myeloid leukemia (AML). Yet, current DC vaccines do not encompass the ideal stimulatory triggers for innate gamma delta (γδ) T cell anti-tumor activity. Promoting type 1 cytotoxic γδ T cells in patients with AML is, however, most interesting, considering these unconventional T cells are primed for rapid function and exert meaningful control over AML. In this work, we demonstrate that interleukin (IL)-15 DCs have the capacity to enhance the anti-tumoral functions of γδ T cells. IL-15 DCs of healthy donors and of AML patients in remission induce the upregulation of cytotoxicity-associated and co-stimulatory molecules on the γδ T cell surface, but not of co-inhibitory molecules, incite γδ T cell proliferation and stimulate their interferon-γ production in the presence of blood cancer cells and phosphoantigens. Moreover, the innate cytotoxic capacity of γδ T cells is significantly enhanced upon interaction with IL-15 DCs, both towards leukemic cell lines and allogeneic primary AML blasts. Finally, we address soluble IL-15 secreted by IL-15 DCs as the main mechanism behind the IL-15 DC-mediated γδ T cell activation. These results indicate that the application of IL-15-secreting DC subsets could render DC-based anti-cancer vaccines more effective through, among others, the involvement of γδ T cells in the anti-leukemic immune response.
Keywords: acute myeloid leukemia; dendritic cell vaccination; immunotherapy; interleukin-15; γδ T cells.
Figures
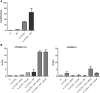
References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

