Spontaneous breathing during veno-venous extracorporeal membrane oxygenation
- PMID: 29732184
- PMCID: PMC5911559
- DOI: 10.21037/jtd.2017.10.27
Spontaneous breathing during veno-venous extracorporeal membrane oxygenation
Abstract
Veno-venous extracorporeal membrane oxygenation (VV ECMO) has started to be applied in awake spontaneously breathing patients as an alternative to invasive mechanical ventilation. As the physiologic cardiorespiratory variability is increased in this condition, the dynamic interaction between patient respiratory activity and extracorporeal system function affects the clinical management. The effect of extracorporeal CO2 removal on patient respiratory drive is variable and not always predictable, with some patients responding to CO2 removal with a decrease in respiratory rate and effort and other patients demonstrating a persistently high work of breathing independent on CO2 unload. While the pathophysiological mechanisms of this different interactions are still to be clarified, improved monitoring ability is needed both to titrate the support in responders and to avoid the risk of ventilation injury in non-responders. Acute changes in patient respiratory patterns may also occur during spontaneous breathing, making it difficult to maintain constant levels of extracorporeal respiratory support, also because changes in the distribution of venous blood volume due to lung-heart interactions affect extracorporeal blood flow. Assessment of native lung function and of its evolution over time is challenging while respiratory gas exchanges are provided by the extracorporeal system, since both oxygenation and decarboxylation capabilities can be fully evaluated only when alveolar ventilation is restored reducing extracorporeal CO2 removal. The rationale for using "awake ECMO" varies across different types of acute respiratory failure: the pathophysiological mechanisms of the underlying disease affect the patient-ECMO interaction and the goal of support. In this review we discuss the pathophysiology, technical challenges and monitoring issues of the use of ECMO in awake spontaneously breathing patients with acute respiratory failure of different etiologies.
Keywords: Awake; acute respiratory distress syndrome (ARDS); bridge to lung transplant; chronic obstructive pulmonary disease (COPD); extracorporeal membrane oxygenation (ECMO); spontaneous breathing; veno-venous (VV).
Conflict of interest statement
Conflicts of Interest: The authors have no conflicts of interest to declare.
Figures


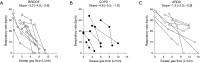
Comment in
-
Awake extracorporeal membrane oxygenation patients expanding the horizons.J Thorac Dis. 2018 Jul;10(Suppl 18):S2215-S2216. doi: 10.21037/jtd.2018.06.28. J Thorac Dis. 2018. PMID: 30123565 Free PMC article. No abstract available.
References
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials
