Clinical outcomes of Transepithelial photorefractive keratectomy to treat low to moderate myopic astigmatism
- PMID: 29743044
- PMCID: PMC5944066
- DOI: 10.1186/s12886-018-0775-5
Clinical outcomes of Transepithelial photorefractive keratectomy to treat low to moderate myopic astigmatism
Abstract
Background: To evaluate the refractive and visual outcomes of Transepithelial photorefractive keratectomy (TransPRK) in the treatment of low to moderate myopic astigmatism.
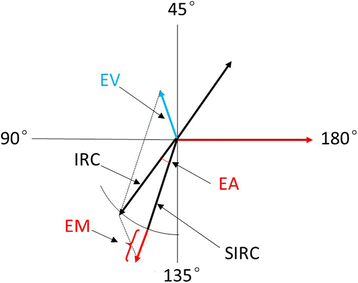
Methods: This retrospective study enrolled a total of 47 eyes that had undergone Transepithelial photorefractive keratectomy. Preoperative cylinder diopters ranged from - 0.75D to - 2.25D (mean - 1.11 ± 0.40D), and the sphere was between - 1.50D to - 5.75D. Visual outcomes and vector analysis of astigmatism that included error ratio (ER), correction ratio (CR), error of magnitude (EM) and error of angle (EA) were evaluated.
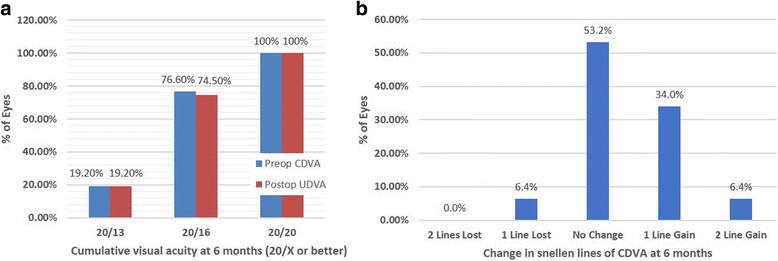
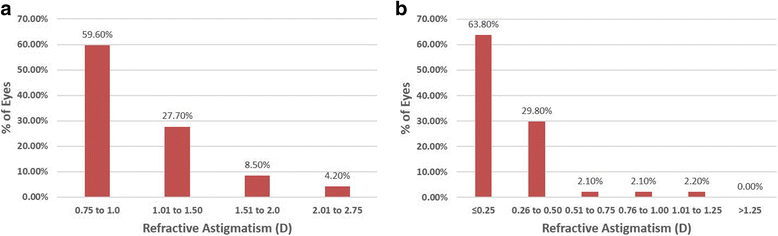
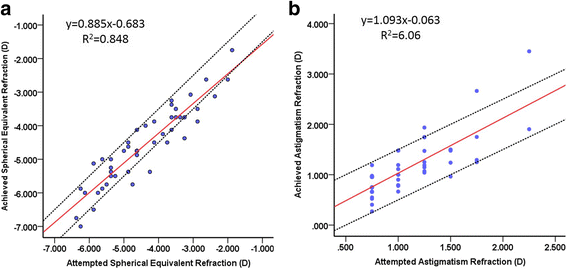
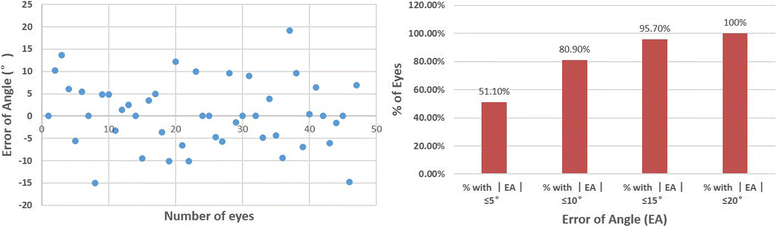
Results: At 6 months after TransPRK, all eyes had an uncorrected distance visual acuity of 20/20 or better, no eyes lost ≥2 lines of corrected distant visual acuity (CDVA), and 93.6% had residual refractive cylinder within ±0.50D of intended correction. On vector analysis, the mean correction ratio for refractive cylinder was 1.03 ± 0.30. The mean error magnitude was - 0.04 ± 0.36. The mean error of angle was 0.44° ± 7.42°and 80.9% of eyes had axis shift within ±10°. The absolute astigmatic error of magnitude was statistically significantly correlated with the intended cylinder correction (r = 0.48, P < 0.01).
Conclusions: TransPRK showed safe, effective and predictable results in the correction of low to moderate astigmatism and myopia.
Keywords: Astigmatism; Myopia; Transepithelial photorefractive keratectomy.
Conflict of interest statement
Ethics approval and consent to participate
This study followed the tenets of the Declaration of Helsinki and approved by the ethics committee of the Department of Ophthalmology, Peking University International Hospital. Informed written consent was obtained from all participants.
Competing interests
The authors declare that they have no competing interests.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Figures
References
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources

